Pneumonic-type lung adenocarcinoma with different ranges exhibiting different clinical, imaging, and pathological characteristics
- PMID: 34787725
- PMCID: PMC8599601
- DOI: 10.1186/s13244-021-01114-2
Pneumonic-type lung adenocarcinoma with different ranges exhibiting different clinical, imaging, and pathological characteristics
Abstract
Background: Pneumonic-type lung adenocarcinoma (PLADC) with different ranges might exhibit different imaging and clinicopathological features. This study divided PLADC into localized PLADC (L-PLADC) and diffuse PLADC (D-PLADC) based on imaging and aimed to clarify the differences in clinical, imaging, and pathologic characteristics between the two new subtypes.
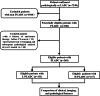
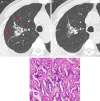
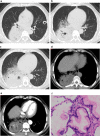
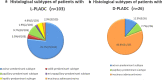
Results: The data of 131 patients with L-PLADC and 117 patients with D-PLADC who were pathologically confirmed and underwent chest computed tomography (CT) at our institute from December 2014 to December 2020 were retrospectively collected. Patients with L-PLADC were predominantly female, non-smokers, and without respiratory symptoms and elevated white blood cell count and C-reactive protein level, whereas those with D-PLADC were predominantly male, smokers, and had respiratory symptoms and elevated white blood cell count and C-reactive protein level (all p < 0.05). Pleural retraction was more common in L-PLADC, whereas interlobular fissure bulging, hypodense sign, air space, CT angiogram sign, coexisting nodules, pleural effusion, and lymphadenopathy were more frequent in D-PLADC (all p < 0.001). Among the 129 patients with surgically resected PLADC, the most common histological subtype of L-PLADC was acinar-predominant growth pattern (76.7%, 79/103), whereas that of D-PLADC was invasive mucinous adenocarcinoma (80.8%, 21/26). Among the 136 patients with EGFR mutation status, L-PLADC had a significantly higher EGFR mutation rate than D-PLADC (p < 0.001).
Conclusions: L-PLADC and D-PLADC have different clinical, imaging, and pathological characteristics. This new imaging-based classification may help improve our understanding of PLADC and develop personalized treatment plans, with concomitant implications for patient outcomes.
Keywords: Epidermal growth factor receptor; Pneumonic-type lung adenocarcinoma; Tomography (X-ray computed).
© 2021. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
Similar articles
-
Pneumonic-type invasive mucinous adenocarcinoma and infectious pneumonia: clinical and CT imaging analysis from multiple centers.BMC Pulm Med. 2022 Dec 3;22(1):460. doi: 10.1186/s12890-022-02268-5. BMC Pulm Med. 2022. PMID: 36461012 Free PMC article.
-
Differential diagnosis of localized pneumonic-type lung adenocarcinoma and pulmonary inflammatory lesion.Insights Imaging. 2022 Mar 22;13(1):49. doi: 10.1186/s13244-022-01200-z. Insights Imaging. 2022. PMID: 35316418 Free PMC article.
-
Differentiation of localized pneumonic-type lung adenocarcinoma from localized pulmonary inflammatory lesion based on clinical data and multi-slice spiral computed tomography imaging features.Transl Cancer Res. 2023 Jan 30;12(1):113-124. doi: 10.21037/tcr-22-2525. Epub 2022 Dec 19. Transl Cancer Res. 2023. PMID: 36760374 Free PMC article.
-
[Advanced Pneumonic-type Lung Carcinoma: A Retrospective Study of Clinical-radiological-pathological Characteristics with Survival Analysis in A Single Chinese Hospital].Zhongguo Fei Ai Za Zhi. 2019 Jun 20;22(6):329-335. doi: 10.3779/j.issn.1009-3419.2019.06.01. Zhongguo Fei Ai Za Zhi. 2019. PMID: 31196365 Free PMC article. Chinese.
-
Association between the novel classification of lung adenocarcinoma subtypes and EGFR/KRAS mutation status: A systematic literature review and pooled-data analysis.Eur J Surg Oncol. 2019 May;45(5):870-876. doi: 10.1016/j.ejso.2019.02.006. Epub 2019 Feb 16. Eur J Surg Oncol. 2019. PMID: 30833014
Cited by
-
The More You See, the More Confusion: Two Cases of Pneumonia With Confusing Imaging Findings of Adenocarcinoma.Cureus. 2024 Aug 24;16(8):e67671. doi: 10.7759/cureus.67671. eCollection 2024 Aug. Cureus. 2024. PMID: 39318949 Free PMC article.
-
Radiological and clinical features of large consolidative-type pulmonary invasive mucinous adenocarcinoma.Clin Respir J. 2024 Mar;18(3):e13743. doi: 10.1111/crj.13743. Clin Respir J. 2024. PMID: 38529681 Free PMC article.
-
Pneumonic-type invasive mucinous adenocarcinoma and infectious pneumonia: clinical and CT imaging analysis from multiple centers.BMC Pulm Med. 2022 Dec 3;22(1):460. doi: 10.1186/s12890-022-02268-5. BMC Pulm Med. 2022. PMID: 36461012 Free PMC article.
-
State of the Art: Lung Cancer Staging Using Updated Imaging Modalities.Bioengineering (Basel). 2022 Sep 22;9(10):493. doi: 10.3390/bioengineering9100493. Bioengineering (Basel). 2022. PMID: 36290461 Free PMC article. Review.
-
Clinicopathological and computed tomography features associated with recurrence-free survival of patients with small-sized peripheral invasive lung adenocarcinoma after sublobectomy.Quant Imaging Med Surg. 2023 Dec 1;13(12):8144-8156. doi: 10.21037/qims-23-559. Epub 2023 Oct 16. Quant Imaging Med Surg. 2023. PMID: 38106273 Free PMC article.
References
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

