Transcatheter aortic valve thrombosis: a review of potential mechanisms
- PMID: 34814733
- PMCID: PMC8611327
- DOI: 10.1098/rsif.2021.0599
Transcatheter aortic valve thrombosis: a review of potential mechanisms
Abstract
Transcatheter aortic valve (TAV) thrombosis has been recognized as a significant problem that sometimes occurs as early as within 30 days after valve implantation, leading to increased concerns of stroke and long-term valve durability. In this article, a critical summary of the relevant literature on identifying potential mechanisms of TAV thrombosis from the perspective of the well-known Virchow's triad, which comprises blood flow, foreign materials and blood biochemistry, is presented. Blood flow mechanisms have been the primary focus thus far, with a general consensus on the flow mechanisms with respect to haemodynamic conditions, the influence of TAV placement and expansion and the influence of coronary flow. Less attention has been paid to the influence of blood biochemistry and foreign materials (and related endothelial damage), with little consensus among studies with regards to platelet and/or microparticle levels post-TAV implantation. Finally, we discuss the future outlook for research with unanswered scientific questions.
Keywords: mechanisms; thrombosis; transcatheter aortic valve.
Figures




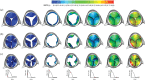
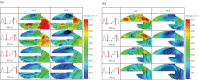
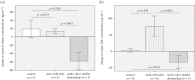
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
