Expert-based medication reviews to reduce polypharmacy in older patients in primary care: a northern-Italian cluster-randomised controlled trial
- PMID: 34814835
- PMCID: PMC8609829
- DOI: 10.1186/s12877-021-02612-0
Expert-based medication reviews to reduce polypharmacy in older patients in primary care: a northern-Italian cluster-randomised controlled trial
Abstract
Background: Evidence regarding clinically relevant effects of interventions aiming at reducing polypharmacy is weak, especially for the primary care setting. This study was initiated with the objective to achieve clinical benefits for older patients (aged 75+) by means of evidence-based reduction of polypharmacy (defined as ≥8 prescribed drugs) and inappropriate prescribing in general practice.
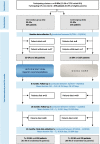
Methods: The cluster-randomised controlled trial involved general practitioners and patients in a northern-Italian region. The intervention consisted of a review of patient's medication regimens by three experts who gave specific recommendations for drug discontinuation. Main outcome measures were non-elective hospital admissions or death within 24 months (composite primary endpoint). Secondary outcomes were drug numbers, hospital admissions, mortality, falls, fractures, quality of life, affective status, cognitive function.
Results: Twenty-two GPs/307 patients participated in the intervention group, 21 GPs/272 patients in the control group. One hundred twenty-five patients (40.7%) experienced the primary outcome in the intervention group, 87 patients (32.0%) in the control group. The adjusted rates of occurrence of the primary outcome did not differ significantly between the study groups (intention-to-treat analysis: adjusted odds ratio 1.46, 95%CI 0.99-2.18, p = 0.06; per-protocol analysis: adjusted OR 1.33, 95%CI 0.87-2.04, p = 0.2). Hospitalisations as single endpoint occurred more frequently in the intervention group according to the unadjusted analysis (OR 1.61, 95%CI 1.03-2.51, p = 0.04) but not in the adjusted analysis (OR 1.39, 95%CI 0.95-2.03, p = 0.09). Falls occurred less frequently in the intervention group (adjusted OR 0.55, 95%CI 0.31-0.98; p = 0.04). No significant differences were found regarding the other outcomes. Definitive discontinuation was obtained for 67 (16.0%) of 419 drugs rated as inappropriate. About 6% of the prescribed drugs were PIMs.
Conclusions: No conclusive effects were found regarding mortality and non-elective hospitalisations as composite respectively single endpoints. Falls were significantly reduced in the intervention group, although definitive discontinuation was achieved for only one out of six inappropriate drugs. These results indicate that (1) even a modest reduction of inappropriate medications may entail positive clinical effects, and that (2) focusing on evidence-based new drug prescriptions and prevention of polypharmacy may be more effective than deprescribing.
Trial registration: Current Controlled Trials (ID ISRCTN: 38449870), date: 11/09/2013.
Keywords: General practice; Inappropriate prescribing; Medication review; Older adults; Polypharmacy.
© 2021. The Author(s).
Conflict of interest statement
All authors declare that they have no competing interests.
Figures
References
-
- Turnheim K. Drug therapy in the elderly. Exp Gerontol. 2004;39(11–12):1731–1738. - PubMed
-
- Muth C, Blom JW, Smith SM, Johnell K, Gonzalez-Gonzalez AI, Nguyen TS, et al. Evidence supporting the best clinical management of patients with multimorbidity and polypharmacy: a systematic guideline review and expert consensus. J Intern Med. 2019;285(3):272–288. - PubMed
-
- Garfinkel D, Zur-Gil S, Ben-Israel J. The war against polypharmacy: a new cost-effective geriatric-palliative approach for improving drug therapy in disabled elderly people. Isr Med Assoc J. 2007;9(6):430–434. - PubMed
-
- Franchi C, Tettamanti M, Pasina L, Djignefa CD, Fortino I, Bortolotti A, et al. Changes in drug prescribing to Italian community-dwelling elderly people: the EPIFARM-elderly project 2000-2010. Eur J Clin Pharmacol. 2014;70(4):437–443. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources