Risk factors of nonalcoholic fatty liver disease in lean body mass population: A systematic review and meta-analysis
- PMID: 34816009
- PMCID: PMC8593777
- DOI: 10.1002/jgh3.12658
Risk factors of nonalcoholic fatty liver disease in lean body mass population: A systematic review and meta-analysis
Abstract
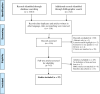
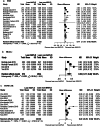
The pathophysiology and risk factors of nonalcoholic fatty liver disease (NAFLD) among lean patients is poorly understood and therefore investigated. We performed a meta-analysis of observational studies. Of 1175 articles found through searching from Medline/PubMed, Banglajol, and Google Scholar by two independent investigators, 22 were selected. Data from lean (n = 6768) and obese (n = 9253) patients with NAFLD were analyzed; lean (n = 43 398) and obese (n = 9619) subjects without NAFLD served as controls. Age, body mass index, waist circumference, systolic blood pressure, and diastolic blood pressure (DBP) had significantly higher estimates in lean NAFLD patients than in lean non-NAFLD controls. Fasting blood sugar [MD(mean difference) 5.17 mg/dl, 95% CI(confidence interval) 4.14-6.16], HbA1c [MD 0.29%, 95% CI 0.11-0.48], and insulin resistance [HOMA-IR] [MD 0.49 U, 95% CI 0.29-0.68]) were higher in lean NAFLD patients than in lean non-NAFLD controls. All components of the lipid profile were raised significantly in the former group except high-density lipoprotein. An increased uric acid (UA) level was found to be associated with the presence of NAFLD among lean. Cardio-metabolic profiles of nonlean NAFLD patients significantly differs from the counter group. However, the magnitude of the difference of lipid and glycemic profile barely reached statistical significance when subjects were grouped according to lean and nonlean NAFLD. But DBP (slope: 0.19, P < 0.037), HOMA-IR (slope: 0.58, P < 0.001), and UA (slope: 0.36, P = 0.022) were significantly higher if NAFLD was present compared to that of non-NAFLD group. Lean and nonlean NAFLD patients are metabolically similar and share common risk factors.
Keywords: lean; meta‐analysis; nonalcoholic fatty liver disease; nonalcoholic steatohepatitis; nonlean; nonobese; risk factors; systematic review.
© 2021 The Authors. JGH Open published by Journal of Gastroenterology and Hepatology Foundation and John Wiley & Sons Australia, Ltd.
Figures




References
-
- Cotter TG, Rinella M. Nonalcoholic fatty liver disease 2020: the state of the disease. Gastroenterology. 2020; 158: 1851–64. - PubMed
-
- Eslam M, Newsome PN, Sarin SK et al. A new definition for metabolic dysfunction‐associated fatty liver disease: an international expert consensus statement. J. Hepatol. 2020; 73: 202–9. - PubMed
-
- Huang T, Behary J, Zekry A. Non‐alcoholic fatty liver disease (NAFLD): a review of epidemiology, risk factors, diagnosis and management. Intern. Med. J. 2019; 50:1038–47. - PubMed
-
- Younossi ZM, Koenig AB, Abdelatif D, Fazel Y, Henry L, Wymer M. Global epidemiology of nonalcoholic fatty liver disease‐Meta‐analytic assessment of prevalence, incidence, and outcomes. Hepatology. 2016; 64: 73–84. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

