Impact of compensated cirrhosis on survival in patients with acute-on-chronic liver failure
- PMID: 34822057
- PMCID: PMC8844167
- DOI: 10.1007/s12072-021-10266-8
Impact of compensated cirrhosis on survival in patients with acute-on-chronic liver failure
Abstract
Background and aims: Acute-on-chronic liver failure (ACLF) is considered a main prognostic event in patients with chronic liver disease (CLD). We analyzed the 28-day and 90-day mortality in ACLF patients with or without underlying cirrhosis enrolled in the ACLF Research Consortium (AARC) database.
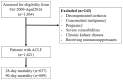
Methods: A total of 1,621 patients were prospectively enrolled and 637 (39.3%) of these patients had cirrhosis. Baseline characteristics, complications and mortality were compared between patients with and without cirrhosis.
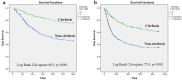
Results: Alcohol consumption was more common in cirrhosis than non-cirrhosis (66.4% vs. 44.2%, p < 0.0001), while non-alcoholic fatty liver disease/cryptogenic CLD (10.9% vs 5.8%, p < 0.0001) and chronic HBV reactivation (18.8% vs 11.8%, p < 0.0001) were more common in non-cirrhosis. Only 0.8% of patients underwent liver transplantation. Overall, 28-day and 90-day mortality rates were 39.3% and 49.9%, respectively. Patients with cirrhosis had a greater chance of survival compared to those without cirrhosis both at 28-day (HR = 0.48; 95% CI 0.36-0.63, p < 0.0001) and 90-day (HR = 0.56; 95% CI 0.43-0.72, p < 0.0001), respectively. In alcohol CLD, non-cirrhosis patients had a higher 28-day (49.9% vs. 23.6%, p < 0.001) and 90-day (58.4% vs. 35.2%, p < 0.001) mortality rate than cirrhosis patients. ACLF patients with cirrhosis had longer mean survival than non-cirrhosis patients (25.5 vs. 18.8 days at 28-day and 65.2 vs. 41.2 days at 90-day). Exaggerated systemic inflammation might be the reason why non-cirrhosis patients had a poorer prognosis than those with cirrhosis after ACLF had occurred.
Conclusions: The 28-day and 90-day mortality rates of ACLF patients without cirrhosis were significantly higher than those with cirrhosis in alcoholic CLD. The presence of cirrhosis and its stage should be evaluated at baseline to guide for management. Thai Clinical Trials Registry, TCTR20191226002.
Keywords: Acute-on-chronic liver failure; Chronic liver disease; Cirrhosis; Liver injury; Mortality; Prognosis.
© 2021. The Author(s).
Conflict of interest statement
Kessarin Thanapirom, Tongluk Teerasarntipan, Sombat Treeprasertsuk, Ashok Choudhury, Manoj K Sahu, Rakhi Maiwall, Viniyendra Pamecha, Richard Moreau, Mamun Al Mahtab, Yogesh Kumar Chawla, Harshad Devarbhavi, Chen Yu, Qin Ning, Deepak Amarapurkar, Chundamannil E. Eapen, Saeed Sadiq Hamid, Amna Subhan Butt, Dong Joon Kim, Guan H. Lee, Ajit Sood, Laurentious A. Lesmana, Zaigham Abbas, Gamal Shiha, Diana A Payawal , Man-Fung Yuen, Albert Chan, George Lau, Jidong Jia, Salimur Rahman, Barjesh C Sharma, Osamu Yokosuka, Shiv Kumar Sarin have nothing to disclose.
Figures
References
-
- Zheng YX, Zhong X, Li YJ, et al. Performance of scoring systems to predict mortality of patients with acute-on-chronic liver failure: a systematic review and meta-analysis. J Gastroenterol Hepatol 2017. (Epub 2017/03/18). - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

