Trend analysis of palliative care consultation service for terminally ill non-cancer patients in Taiwan: a 9-year observational study
- PMID: 34823512
- PMCID: PMC8614035
- DOI: 10.1186/s12904-021-00879-z
Trend analysis of palliative care consultation service for terminally ill non-cancer patients in Taiwan: a 9-year observational study
Abstract
Backgrounds: Early integration of palliative care for terminally ill non-cancer patients improves quality of life. However, there are scanty data on Palliative Care Consultation Service (PCCS) among non-cancer patients.
Methods: In this 9-year observational study Data were collected from the Hospice-Palliative Clinical Database (HPCD) of Taichung Veterans General Hospital (TCVGH). Terminally ill non-cancer patients with 9 categories of diagnoses who received PCCS during 2011 to 2019 were enrolled. Trend analysis was performed to evaluate differences in categories of diagnosis throughout study period, duration of PCCS, patient outcomes, DNR declaration, awareness of disease by patients and families before and after PCCS.
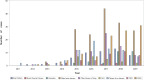
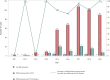
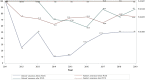
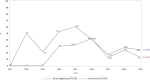
Results: In total, 536 non-cancer patients received PCCS from 2011 to 2019 with an average age of 70.7 years. The average duration of PCCS was 18.4 days. The distributions of age, gender, patient outcomes, family's awareness of disease before PCCS, and patient's awareness of disease after PCCS were significantly different among the diagnoses. Organic brain disease and Chronic kidney disease (CKD) were the most prevalent diagnoses in patients receiving PCCS in 2019. For DNR declaration, the percentage of patients signing DNR before PCCS remained high throughout the study period (92.8% in 2019). Patient outcomes varied according to the disease diagnoses.
Conclusion: This 9-year observational study showed that the trend of PCCS among non-cancer patients had changed over the duration of the study. An increasing number of terminally ill non-cancer patients received PCCS during late life, thereby increasing the awareness of disease for both patients and families, which would tend to better prepare terminally ill patients for end-of-life as they may consider DNR consent. Early integration of PCCS into ordinary care for terminally non-cancer patients is essential for better quality of life.
Keywords: Awareness; Do-not-resuscitate; Non-cancer; Palliative care consultation service.
© 2021. The Author(s).
Conflict of interest statement
The authors declare no conflicts of interests.
Figures
Similar articles
-
Use and impact of a novel nurse-led consultation model in a palliative care consultation service for terminally ill cancer patients in Taiwan: an 11-year observational study.Support Care Cancer. 2023 Mar 31;31(4):246. doi: 10.1007/s00520-023-07697-4. Support Care Cancer. 2023. PMID: 37000288
-
Palliative Care Consultation Services on Terminally Ill Cancer Patients and Non-Cancer Patients: Trend Analysis from a 9-Year-Long Observational Study in Taiwan.Int J Environ Res Public Health. 2021 Sep 19;18(18):9882. doi: 10.3390/ijerph18189882. Int J Environ Res Public Health. 2021. PMID: 34574805 Free PMC article.
-
Predictive factors for do-not-resuscitate designation among terminally ill cancer patients receiving care from a palliative care consultation service.J Pain Symptom Manage. 2014 Feb;47(2):271-82. doi: 10.1016/j.jpainsymman.2013.03.020. Epub 2013 Jul 12. J Pain Symptom Manage. 2014. PMID: 23856097
-
Developing an integrated model of community-based palliative care into the primary health care (PHC) for terminally ill cancer patients in Iran.BMC Palliat Care. 2021 Jun 28;20(1):100. doi: 10.1186/s12904-021-00795-2. BMC Palliat Care. 2021. PMID: 34182980 Free PMC article. Review.
-
Palliative and end-of-life care in prisons: a content analysis of the literature.Int J Prison Health. 2014;10(3):172-97. doi: 10.1108/IJPH-05-2013-0024. Int J Prison Health. 2014. PMID: 25764177 Review.
Cited by
-
Exploring Risk Factors of Unexpected Death, Using Palliative Care Outcomes Collaboration (PCOC) Measures, among Terminal Patients Receiving Palliative Care in Taiwan.Int J Environ Res Public Health. 2022 Oct 15;19(20):13294. doi: 10.3390/ijerph192013294. Int J Environ Res Public Health. 2022. PMID: 36293875 Free PMC article.
-
Effects of different palliative care models on decedents with kidney failure receiving maintenance dialysis: a nationwide population-based retrospective observational study in Taiwan.BMJ Open. 2023 Jul 10;13(7):e069835. doi: 10.1136/bmjopen-2022-069835. BMJ Open. 2023. PMID: 37429693 Free PMC article.
-
Patient and hospital characteristics associated with do-not-resuscitate/do-not-intubate orders: a cross-sectional study based on the Taiwan stroke registry.BMC Palliat Care. 2023 Sep 15;22(1):138. doi: 10.1186/s12904-023-01257-7. BMC Palliat Care. 2023. PMID: 37715158 Free PMC article.
-
The clinical effect evaluation of multidisciplinary collaborative team combined with palliative care model in patients with terminal cancer: a randomised controlled study.BMC Palliat Care. 2023 Jun 13;22(1):71. doi: 10.1186/s12904-023-01192-7. BMC Palliat Care. 2023. PMID: 37312118 Free PMC article. Clinical Trial.
-
Predictors and Assessment of Hospice Use for End-Stage Renal Disease Patients in Taiwan.Int J Environ Res Public Health. 2021 Dec 22;19(1):85. doi: 10.3390/ijerph19010085. Int J Environ Res Public Health. 2021. PMID: 35010349 Free PMC article.
References
-
- Beard JR, Officer A, de Carvalho IA, Sadana R, Pot AM, Michel JP, Lloyd-Sherlock P, Epping-Jordan JE, Peeters G, Mahanani WR, et al. The World report on ageing and health: a policy framework for healthy ageing. Lancet (London, England) 2016;387(10033):2145–2154. doi: 10.1016/S0140-6736(15)00516-4. - DOI - PMC - PubMed
-
- Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, Abraham J, Adair T, Aggarwal R, Ahn SY, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the global burden of disease study 2010. Lancet (London, England) 2012;380(9859):2095–2128. doi: 10.1016/S0140-6736(12)61728-0. - DOI - PMC - PubMed
-
- Lastrucci V, D'Arienzo S, Collini F, Lorini C, Zuppiroli A, Forni S, Bonaccorsi G, Gemmi F, Vannucci A. Diagnosis-related differences in the quality of end-of-life care: a comparison between cancer and non-cancer patients. PLoS One. 2018;13(9):e0204458. doi: 10.1371/journal.pone.0204458. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

