Reverse Shoulder Arthroplasty with Bony and Metallic versus Standard Bony Reconstruction for Severe Glenoid Bone Loss. A Retrospective Comparative Cohort Study
- PMID: 34830556
- PMCID: PMC8622484
- DOI: 10.3390/jcm10225274
Reverse Shoulder Arthroplasty with Bony and Metallic versus Standard Bony Reconstruction for Severe Glenoid Bone Loss. A Retrospective Comparative Cohort Study
Abstract
There are different techniques to address severe glenoid erosion during reverse shoulder arthroplasty (RSA). This study assessed the clinical and radiological outcomes of RSA with combined bony and metallic augment (BMA) glenoid reconstruction compared to bony augmentation (BA) alone. A review of patients who underwent RSA with severe glenoid bone loss requiring reconstruction from January 2017 to January 2019 was performed. Patients were divided into two groups: BMA versus BA alone. Clinical outcome measurements included two years postoperative ROM, Constant score, subjective shoulder value (SSV), and the American Shoulder and Elbow Surgeons Shoulder (ASES) score. Radiological outcomes included radiographic evidence of scapular complications and graft incorporation. The BMA group had significantly different glenoid morphology (p < 0.001) and greater bone loss thickness than the BA group (16.3 ± 3.8 mm vs. 12.0 ± 0.0 mm, p = 0.020). Both groups had significantly improved ROM (anterior forward flexion and external rotation) and clinical scores (Constant, SSV and ASES scores) at 2 years. Greater improvement was observed in the BMA group in terms of anterior forward flexion (86.3° ± 27.9° vs. 43.8° ± 25.6°, p = 0.013) and Constant score (56.6 ± 10.1 vs. 38.3 ± 16.7, p = 0.021). The BA group demonstrated greater functional and clinical improvements with higher postoperative active external rotation and ASES results (active external rotation, 49.4° ± 17.0° vs. 29.4° ± 14.7°, p = 0.017; ASES, 89.1 ± 11.3 vs. 76.8 ± 11.0, p = 0.045). The combination use of bone graft and metallic augments in severe glenoid bone loss during RSA is safe and effective and can be considered in cases of severe glenoid bone loss where bone graft alone may be insufficient.
Keywords: autologous graft; defect; integration; loosening; prosthesis; reconstruction; shoulder; survivorship.
Conflict of interest statement
Marko Nabergoj reports no conflict of interest. Lionel Neyton reports that he is a paid consultant for Arthrex and Tornier/Stryker and receives royalties from Tornier/Stryker. He is member of the Advisory Board of Sparta Biopharma and owns stock options. Hugo Bothorel reports no conflict of interest. Sean WL Ho reports no conflict of interest. Sidi Wang reports no conflict of interest. Xueling Chong reports no conflict of interest. Dr. Lädermann reports that he is a paid consultant for Arthrex, Inc., Stryker, and Medacta, and he receives royalties from Stryker. He is the founder of the FORE Foundation, Med4cast, and BeeMed. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures

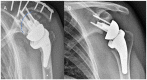


References
-
- Blix M. Die Länge und die Spannung des Muskels. 1 Skandinavisches. Arch. Physiol. 1892;3:295–318.
-
- Roche C.P., Diep P., Hamilton M., Crosby L.A., Flurin P.H., Wright T.W., Zuckerman J.D., Routman H.D. Impact of inferior glenoid tilt, humeral retroversion, bone grafting, and design parameters on muscle length and deltoid wrapping in reverse shoulder arthroplasty. Bull. Hosp. Jt. Dis. 2013;71:284–293. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

