Albumin Substitution in Decompensated Liver Cirrhosis: Don't Forget Zinc
- PMID: 34836265
- PMCID: PMC8618355
- DOI: 10.3390/nu13114011
Albumin Substitution in Decompensated Liver Cirrhosis: Don't Forget Zinc
Abstract
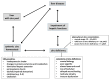
Decompensated liver cirrhosis has a dismal prognosis, with patients surviving on average for 2-4 years after the first diagnosis of ascites. Albumin is an important tool in the therapy of cirrhotic ascites. By virtue of its oncotic properties, it reduces the risk of cardiovascular dysfunction after paracentesis. Treatment with albumin also counteracts the development of hepatorenal syndrome and spontaneous bacterial peritonitis. More recently, the positive impact of long-term albumin supplementation in liver disease, based on its pleiotropic non-oncotic activities, has been recognized. These include transport of endo- and exogenous substances, anti-inflammatory, antioxidant and immunomodulatory activities, and stabilizing effects on the endothelium. Besides the growing recognition that effective albumin therapy requires adjustment of the plasma level to normal physiological values, the search for substances with adjuvant activities is becoming increasingly important. More than 75% of patients with decompensated liver cirrhosis do not only present with hypoalbuminemia but also with zinc deficiency. There is a close relationship between albumin and the essential trace element zinc. First and foremost, albumin is the main carrier of zinc in plasma, and is hence critical for systemic distribution of zinc. In this review, we discuss important functions of albumin in the context of metabolic, immunological, oxidative, transport, and distribution processes, alongside crucial functions and effects of zinc and their mutual dependencies. In particular, we focus on the major role of chronic inflammatory processes in pathogenesis and progression of liver cirrhosis and how albumin therapy and zinc supplementation may affect these processes.
Keywords: albumin; liver cirrhosis; zinc.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


Similar articles
-
[News for usage of albumin in patients with liver disease].Dtsch Med Wochenschr. 2020 Jun;145(11):722-726. doi: 10.1055/a-1012-6991. Epub 2020 Jun 3. Dtsch Med Wochenschr. 2020. PMID: 32492740 German.
-
Albumin administration in patients with cirrhosis: Current role and novel perspectives.World J Gastroenterol. 2022 Sep 7;28(33):4773-4786. doi: 10.3748/wjg.v28.i33.4773. World J Gastroenterol. 2022. PMID: 36156923 Free PMC article. Review.
-
Role of albumin in the treatment of decompensated liver cirrhosis.Curr Opin Gastroenterol. 2022 May 1;38(3):200-205. doi: 10.1097/MOG.0000000000000838. Epub 2022 Mar 11. Curr Opin Gastroenterol. 2022. PMID: 35275900 Review.
-
Current indications for the use of albumin in the treatment of cirrhosis.Ann Hepatol. 2011 May;10 Suppl 1:S15-20. Ann Hepatol. 2011. PMID: 21566250
-
Position statement on the use of albumin in liver cirrhosis.Ann Hepatol. 2022 Jul-Aug;27(4):100708. doi: 10.1016/j.aohep.2022.100708. Epub 2022 May 10. Ann Hepatol. 2022. PMID: 35550187
Cited by
-
Transferrin levels are associated with malnutrition markers in hemodialysis patients in KwaZulu-Natal, South Africa.Ren Fail. 2024 Dec;46(1):2337292. doi: 10.1080/0886022X.2024.2337292. Epub 2024 Apr 14. Ren Fail. 2024. PMID: 38616181 Free PMC article.
-
Acute and sub-acute toxicity study of aqueous and methanol root extract of Tetracera alnifolia in male albino rats.Toxicol Rep. 2024 Oct 22;13:101786. doi: 10.1016/j.toxrep.2024.101786. eCollection 2024 Dec. Toxicol Rep. 2024. PMID: 39526239 Free PMC article.
-
Serum trace element alterations in Indian patients with metabolic dysfunction-associated steatotic liver disease.Indian J Gastroenterol. 2024 Aug;43(4):845-848. doi: 10.1007/s12664-024-01587-1. Indian J Gastroenterol. 2024. PMID: 38703301 No abstract available.
-
Zinc's Association with the CmPn/CmP Signaling Network in Breast Cancer Tumorigenesis.Biomolecules. 2022 Nov 11;12(11):1672. doi: 10.3390/biom12111672. Biomolecules. 2022. PMID: 36421686 Free PMC article. Review.
-
Therapeutic potential of zinc 64Zn aspartate for obesity management: impact on oxidative stress, lipid metabolism, pancreas and liver in high-calorie diet model.Front Pharmacol. 2025 May 16;16:1543166. doi: 10.3389/fphar.2025.1543166. eCollection 2025. Front Pharmacol. 2025. PMID: 40453670 Free PMC article.
References
-
- Domenicali M., Baldassarre M., Giannone F.A., Naldi M., Mastroroberto M., Biselli M., Laggetta M., Patrono D., Bertucci C., Bernardi M., et al. Posttranscriptional changes of serum albumin: Clinical and prognostic significance in hospitalized patients with cirrhosis. Hepatology. 2014;60:1851–1860. doi: 10.1002/hep.27322. - DOI - PubMed
-
- Sauerbruch T. (D)ILC–Entwicklungen in der Hepatologie. Z. Gastroenterol. 2020;58:83–86.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

