Moxibustion Regulates Gastrointestinal Motility via HCN1 in Functional Dyspepsia Rats
- PMID: 34845181
- PMCID: PMC8642983
- DOI: 10.12659/MSM.932885
Moxibustion Regulates Gastrointestinal Motility via HCN1 in Functional Dyspepsia Rats
Abstract
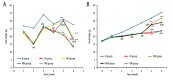
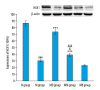
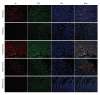
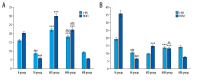
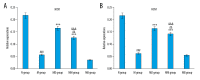
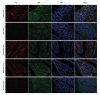
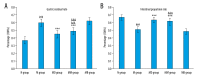
BACKGROUND Moxibustion therapy has been found to ameliorate clinical symptoms of functional dyspepsia (FD). We aimed to examine the regulatory effect of moxibustion on the gastrointestinal (GI) motility in FD and explore the underlying mechanism based on the hyperpolarization-activated cyclic nucleotide-gated cation channel 1 (HCN1). MATERIAL AND METHODS Moxibustion therapy was used in FD rats induced by using classic tail-pinch and irregular feeding. Weight gain and food intake were recorded weekly, followed by detecting gastric residual rate (GRR) and small intestine propulsion rate (IPR). Next, western blotting was performed to determine the expression levels of HCN1 in the gastric antrum. qRT-PCR was used to detect HCN1 in the small intestine and hypothalamic satiety center. Double immunolabeling was used for HCN1 and ICCs in gastric antrum and small intestine. RESULTS The obtained results suggested that moxibustion treatment could increase weight gain and food intake in FD rats. The GRR and IPR were compared among the groups, which showed that moxibustion treatment could decrease GRR and increase IPR. Moxibustion increased the expression of HCN1 in the gastric antrum, small intestine, and hypothalamic satiety center. Histologically, the co-expressions of HCN1 and ICCs tended to increase in gastric antrum and small intestine. Meanwhile, HCN channel inhibitor ZD7288 prevented the above-mentioned therapeutic effects of moxibustion. CONCLUSIONS The results of the present study suggest that moxibustion can effectively improve the GI motility of FD rats, which may be related to the upregulation of HCN1 expression in gastric antrum, small intestine, and satiety center.
Conflict of interest statement
Figures
Similar articles
-
Acupuncture and moxibustion intervention in functional dyspepsia: Gastric and duodenal regulation.Heliyon. 2024 Aug 6;10(17):e35696. doi: 10.1016/j.heliyon.2024.e35696. eCollection 2024 Sep 15. Heliyon. 2024. PMID: 39263151 Free PMC article. Review.
-
Involvement of hyperpolarization-activated, cyclic nucleotide-gated cation channels in dorsal root ganglion in neuropathic pain.Sheng Li Xue Bao. 2008 Oct 25;60(5):579-80. Sheng Li Xue Bao. 2008. PMID: 18958363
-
[Electroacupuncture at "Zusanli"(ST36) promotes gastrointestinal motility possibly by suppres-sing excessive autophagy via AMPK/ULK1 signaling in rats with functional dyspepsia].Zhen Ci Yan Jiu. 2019 Jul 25;44(7):486-91. doi: 10.13702/j.1000-0607.180571. Zhen Ci Yan Jiu. 2019. PMID: 31368278 Chinese.
-
Changes in hyperpolarization-activated cyclic nucleotide-gated channel expression and activity in bladder interstitial cells of Cajal from rats with detrusor overactivity.Int Urogynecol J. 2015 Aug;26(8):1139-45. doi: 10.1007/s00192-015-2632-x. Epub 2015 Feb 13. Int Urogynecol J. 2015. PMID: 25677606
-
Hyperpolarization-activated and cyclic nucleotide-gated channel proteins as emerging new targets in neuropathic pain.Rev Neurosci. 2019 Jul 26;30(6):639-649. doi: 10.1515/revneuro-2018-0094. Rev Neurosci. 2019. PMID: 30768426 Review.
Cited by
-
Electroacupuncture Improves Gastrointestinal Motility in Rats with Functional Dyspepsia via the GDNF/GFRα1/PI3K/Akt Signaling Pathway.Curr Med Sci. 2025 Aug;45(4):957-965. doi: 10.1007/s11596-025-00086-4. Epub 2025 Aug 8. Curr Med Sci. 2025. PMID: 40779005
-
A comparative metabolomics study between grain-sized moxibustion and suspended moxibustion on rats with gastric ulcers.Heliyon. 2023 Aug 11;9(8):e19108. doi: 10.1016/j.heliyon.2023.e19108. eCollection 2023 Aug. Heliyon. 2023. PMID: 37664739 Free PMC article.
-
Acupuncture and moxibustion intervention in functional dyspepsia: Gastric and duodenal regulation.Heliyon. 2024 Aug 6;10(17):e35696. doi: 10.1016/j.heliyon.2024.e35696. eCollection 2024 Sep 15. Heliyon. 2024. PMID: 39263151 Free PMC article. Review.
References
-
- Ford AC, Mahadeva S, Carbone MF, et al. Functional dyspepsia. Lancet. 2020;396:1689–702. - PubMed
-
- Black CJ, Drossman DA, Talley NJ, et al. Functional gastrointestinal disorders: Advances in understanding and management. Lancet. 2020;396:1664–74. - PubMed
-
- Stanghellini V, Chan FK, Hasler WL, et al. Gastroduodenal disorders. Gastroenterology. 2016;150:1380–92. - PubMed
-
- Talley NJ, Ford AC. Functional dyspepsia. N Engl J Med. 2016;374:896. - PubMed
-
- Mani J, Madani S, Thomas R. Economic impact and prognostic factors of functional dyspepsia in children. J Pediatr Gastroenterol Nutr. 2020;70:e65–70. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases

