Assessment of Patient Preferences for Telehealth in Post-COVID-19 Pandemic Health Care
- PMID: 34851400
- PMCID: PMC8637257
- DOI: 10.1001/jamanetworkopen.2021.36405
Assessment of Patient Preferences for Telehealth in Post-COVID-19 Pandemic Health Care
Abstract
Importance: Telehealth use greatly increased in 2020 during the first year of the COVID-19 pandemic. Patient preferences for telehealth or in-person care are an important factor in defining the role of telehealth in the postpandemic world.
Objective: To ascertain patient preferences for video visits after the ongoing COVID-19 public health emergency and to identify patient perceptions of the value of video visits and the role of out-of-pocket cost in changing patient preference for each visit modality.
Design, setting, and participants: This survey study was conducted using a nationally representative sample of adult members of the RAND American Life Panel. The data were obtained from the American Life Panel Omnibus Survey, which was fielded between March 8 and 19, 2021.
Main outcomes and measures: Preferences for video visits vs in-person care were analyzed in the survey. The first question was about participants' baseline preference for an in-person or a video visit for a nonemergency health issue. The second question entailed choosing between the preferred visit modality with a cost of $30 and another modality with a cost of $10. Questions also involved demographic characteristics, experience with video visits, willingness to use video visits, and preferences for the amount of telehealth use after the COVID-19 pandemic.
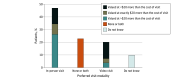
Results: A total of 2080 of 3391 sampled panel members completed the survey (participation rate, 61.3%). Participants in the weighted sample had a mean (SE) age of 51.1 (0.67) years and were primarily women (1079 [51.9%]). Most participants (66.5%) preferred at least some video visits in the future, but when faced with a choice between an in-person or a video visit for a health care encounter that could be conducted either way, more than half of respondents (53.0%) preferred an in-person visit. Among those who initially preferred an in-person visit when out-of-pocket costs were not a factor, 49.8% still preferred in-person care and 23.5% switched to a video visit when confronted with higher relative costs for in-person care. In contrast, among those who initially preferred a video visit, only 18.9% still preferred a video visit and 61.7% switched to in-person visit when confronted with higher relative costs for video visits.
Conclusions and relevance: This survey study found that participants were generally willing to use video visits but preferred in-person care, and those who preferred video visits were more sensitive to paying out-of-pocket cost. These results suggest that understanding patient preferences will help identify telehealth's role in future health care delivery.
Conflict of interest statement
Figures
Similar articles
-
Patient Perceptions of Video Visits Using Veterans Affairs Telehealth Tablets: Survey Study.J Med Internet Res. 2020 Apr 15;22(4):e15682. doi: 10.2196/15682. J Med Internet Res. 2020. PMID: 32293573 Free PMC article.
-
Telehealth Preferences Among Patients With Advanced Cancer in the Post COVID-19 Vaccine Era.J Pain Symptom Manage. 2024 Jun;67(6):525-534.e1. doi: 10.1016/j.jpainsymman.2024.02.572. Epub 2024 Mar 10. J Pain Symptom Manage. 2024. PMID: 38467349 Free PMC article.
-
People's Experiences and Satisfaction With Telehealth During the COVID-19 Pandemic in Australia: Cross-Sectional Survey Study.J Med Internet Res. 2020 Dec 10;22(12):e24531. doi: 10.2196/24531. J Med Internet Res. 2020. PMID: 33156806 Free PMC article.
-
Telemedicine and Its Perceptions in a Border Community: A Review of How Health Care Technology Has Helped Increase Access.Telemed J E Health. 2024 Apr;30(4):987-993. doi: 10.1089/tmj.2023.0179. Epub 2023 Nov 17. Telemed J E Health. 2024. PMID: 37976130 Review.
-
Impact of Asynchronous Electronic Communication-Based Visits on Clinical Outcomes and Health Care Delivery: Systematic Review.J Med Internet Res. 2021 May 5;23(5):e27531. doi: 10.2196/27531. J Med Internet Res. 2021. PMID: 33843592 Free PMC article.
Cited by
-
Reasons for Not Pursuing Virtual Prenatal Care in 2020 Through 2021 and Policy Implications.Telemed J E Health. 2023 Oct;29(10):1492-1503. doi: 10.1089/tmj.2022.0492. Epub 2023 Feb 14. Telemed J E Health. 2023. PMID: 36787485 Free PMC article.
-
Association between state payment parity policies and telehealth usage at community health centers during COVID-19.J Am Med Inform Assoc. 2022 Sep 12;29(10):1715-1721. doi: 10.1093/jamia/ocac104. J Am Med Inform Assoc. 2022. PMID: 35864736 Free PMC article.
-
Prescription Trends of Biologic DMARDs in Treating Rheumatologic Diseases: Changes of Medication Availability in COVID-19.J Pers Med. 2023 Jul 28;13(8):1199. doi: 10.3390/jpm13081199. J Pers Med. 2023. PMID: 37623450 Free PMC article.
-
Patient Preferences for Telerehabilitation Compared to In-Person Physiotherapy: A Binary Discrete Choice Experiment.Physiother Res Int. 2025 Apr;30(2):e70042. doi: 10.1002/pri.70042. Physiother Res Int. 2025. PMID: 40008766 Free PMC article.
-
Comparison of Use Rates of Telehealth Services for Substance Use Disorder During and Following COVID-19 Safety Distancing Recommendations: Two Cross-Sectional Surveys.JMIR Ment Health. 2024 Aug 12;11:e52363. doi: 10.2196/52363. JMIR Ment Health. 2024. PMID: 39136186 Free PMC article.
References
-
- The COVID-19 Healthcare Coalition Telehealth Impact Study Work Group . Telehealth impact: physician survey analysis. November 16, 2020. Accessed June 1, 2021. https://telehealth-c19hcc-org-bzh6faksvq-uk.a.run.app/telehealth/physici...
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical