Handheld chromatic pupillometry can accurately and rapidly reveal functional loss in glaucoma
- PMID: 34853018
- PMCID: PMC10176376
- DOI: 10.1136/bjophthalmol-2021-319938
Handheld chromatic pupillometry can accurately and rapidly reveal functional loss in glaucoma
Abstract
Background/aims: Early detection and treatment of glaucoma can delay vision loss. In this study, we evaluate the performance of handheld chromatic pupillometry (HCP) for the objective and rapid detection of functional loss in glaucoma.
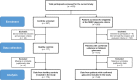
Methods: In this clinic-based, prospective study, we enrolled 149 patients (median (IQR) years: 68.5 (13.6) years) with confirmed glaucoma and 173 healthy controls (55.2 (26.7) years). Changes in pupil size in response to 9 s of exponentially increasing blue (469 nm) and red (640 nm) light-stimuli were assessed monocularly using a custom-built handheld pupillometer. Pupillometric features were extracted from individual traces and compared between groups. Features with the highest classification potential, selected using a gradient boosting machine technique, were incorporated into a generalised linear model for glaucoma classification. Receiver operating characteristic curve analyses (ROC) were used to compare the performance of HCP, optical coherence tomography (OCT) and Humphrey Visual Field (HVF).
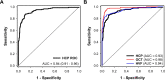
Results: Pupillary light responses were altered in glaucoma compared with controls. For glaucoma classification, HCP yielded an area under the ROC curve (AUC) of 0.94 (95% CI 0.91 to 0.96), a sensitivity of 87.9% and specificity of 88.4%. The classification performance of HCP in early-moderate glaucoma (visual field mean deviation (VFMD) > -12 dB; AUC=0.91 (95% CI 0.87 to 0.95)) was similar to HVF (AUC=0.91) and reduced compared with OCT (AUC=0.97; p=0.01). For severe glaucoma (VFMD ≤ -12 dB), HCP had an excellent classification performance (AUC=0.98, 95% CI 0.97 to 1) that was similar to HVF and OCT.
Conclusion: HCP allows for an accurate, objective and rapid detection of functional loss in glaucomatous eyes of different severities.
Keywords: glaucoma; optic nerve; pupil.
© Author(s) (or their employer(s)) 2023. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: DM has a patent application based on the pupillometry protocol used in the present study (PCT/SG2015/050494): A method and system for monitoring and/or assessing pupillary responses. RPN, TA and DM have a patent application based on the handheld pupillometer used in this study (PCT/SG2018/050204): Handheld ophthalmic and neurological screening device. The rest of the authors have no conflicts of interest to disclose.
Figures

Similar articles
-
Handheld chromatic pupillometry can reliably detect functional glaucomatous damage in eyes with high myopia.Br J Ophthalmol. 2024 May 21;108(6):818-825. doi: 10.1136/bjo-2023-323878. Br J Ophthalmol. 2024. PMID: 37524446
-
Pupillary Responses to Full-Field Chromatic Stimuli Are Reduced in Patients with Early-Stage Primary Open-Angle Glaucoma.Ophthalmology. 2018 Sep;125(9):1362-1371. doi: 10.1016/j.ophtha.2018.02.024. Epub 2018 Mar 21. Ophthalmology. 2018. PMID: 29573814
-
Binocular head-mounted chromatic pupillometry can detect structural and functional loss in glaucoma.Front Neurosci. 2023 Jun 29;17:1187619. doi: 10.3389/fnins.2023.1187619. eCollection 2023. Front Neurosci. 2023. PMID: 37456990 Free PMC article.
-
[New insights into the pathogenesis of glaucomatous optic neuropathy and refinement of the objective assessment of its functional damage].Nippon Ganka Gakkai Zasshi. 2012 Mar;116(3):298-344; discussion 345-6. Nippon Ganka Gakkai Zasshi. 2012. PMID: 22568105 Review. Japanese.
-
Evaluating State-of-the-Art Computerized Pupillary Assessments for Glaucoma Detection: A Systematic Review and Meta-Analysis.Front Neurol. 2020 Jul 29;11:777. doi: 10.3389/fneur.2020.00777. eCollection 2020. Front Neurol. 2020. PMID: 32849229 Free PMC article.
Cited by
-
Differences in the Pupillary Responses to Evening Light between Children and Adolescents.bioRxiv [Preprint]. 2023 Aug 14:2023.08.09.552691. doi: 10.1101/2023.08.09.552691. bioRxiv. 2023. Update in: J Physiol Anthropol. 2024 Jul 3;43(1):16. doi: 10.1186/s40101-024-00363-6. PMID: 37645820 Free PMC article. Updated. Preprint.
-
Retinal neural dysfunction in diabetes revealed with handheld chromatic pupillometry.Clin Exp Ophthalmol. 2022 Sep;50(7):745-756. doi: 10.1111/ceo.14116. Epub 2022 Jun 13. Clin Exp Ophthalmol. 2022. PMID: 35616273 Free PMC article.
-
Chromatic pupillometry for evaluating melanopsin retinal ganglion cell function in Alzheimer's disease and other neurodegenerative disorders: a review.Front Psychol. 2024 Jan 8;14:1295129. doi: 10.3389/fpsyg.2023.1295129. eCollection 2023. Front Psychol. 2024. PMID: 38259552 Free PMC article. Review.
-
The Structural Layers of the Porcine Iris Exhibit Inherently Different Biomechanical Properties.Invest Ophthalmol Vis Sci. 2023 Oct 3;64(13):11. doi: 10.1167/iovs.64.13.11. Invest Ophthalmol Vis Sci. 2023. PMID: 37796489 Free PMC article.
-
Evaluation of the Glaucomatous Macular Damage by Chromatic Pupillometry.Ophthalmol Ther. 2023 Aug;12(4):2133-2156. doi: 10.1007/s40123-023-00738-5. Epub 2023 Jun 7. Ophthalmol Ther. 2023. PMID: 37284935 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
