Cerebral Venous Sinus Thrombosis Associated With Coronavirus Disease 2019: Case Report and Review of the Literature
- PMID: 34855659
- PMCID: PMC9439631
- DOI: 10.1097/NRL.0000000000000390
Cerebral Venous Sinus Thrombosis Associated With Coronavirus Disease 2019: Case Report and Review of the Literature
Abstract
Introduction: Coronavirus disease 2019 (COVID-19) is associated with significant risk of acute thrombosis. We present a case report of a patient with cerebral venous sinus thrombosis (CVST) associated with COVID-19 and performed a literature review of CVST associated with COVID-19 cases.
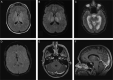
Case report: A 38-year-old woman was admitted with severe headache and acute altered mental status a week after confirmed diagnosis of COVID-19. Magnetic resonance imaging brain showed diffuse venous sinus thrombosis involving the superficial and deep veins, and diffuse edema of bilateral thalami, basal ganglia and hippocampi because of venous infarction. Her neurological exam improved with anticoagulation (AC) and was subsequently discharged home. We identified 43 patients presenting with CVST associated with COVID-19 infection. 56% were male with mean age of 51.8±18.2 years old. The mean time of CVST diagnosis was 15.6±23.7 days after onset of COVID-19 symptoms. Most patients (87%) had thrombosis of multiple dural sinuses and parenchymal changes (79%). Almost 40% had deep cerebral venous system thrombosis. Laboratory findings revealed elevated mean D-dimer level (7.14/mL±12.23 mg/L) and mean fibrinogen level (4.71±1.93 g/L). Less than half of patients had prior thrombotic risk factors. Seventeen patients (52%) had good outcomes (mRS <=2). The mortality rate was 39% (13 patients).
Conclusion: CVST should be in the differential diagnosis when patients present with acute neurological symptoms in this COVID pandemic. The mortality rate of CVST associated with COVID-19 can be very high, therefore, early diagnosis and prompt treatment are crucial to the outcomes of these patients.
Copyright © 2021 Wolters Kluwer Health, Inc. All rights reserved.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


References
-
- Worldometers.info. 2021. Coronavirus Update (Live): 105,870,383 cases and 2,306,868 deaths from COVID-19 virus pandemic—Worldometer. 2021. Available at: https://www.worldometers.info/coronavirus/. Accessed February 5, 2021.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

