Comparison of Beinaglutide Versus Metformin for Weight Loss in Overweight and Obese Non-diabetic Patients
- PMID: 34856624
- PMCID: PMC9286864
- DOI: 10.1055/a-1608-0345
Comparison of Beinaglutide Versus Metformin for Weight Loss in Overweight and Obese Non-diabetic Patients
Abstract
Purpose: We compared the efficacy and safety of beinaglutide, a glucagon-like peptide-1 (GLP-1) analogue with metformin in lowering the bodyweight of patients who were overweight/obese and non-diabetic.
Patients and methods: Seventy-eight non-diabetic patients were randomly selected and beinaglutide or metformin was administered for 12 weeks. The primary endpoints were changes in body weight and the proportions of patients who lost≥5 and≥10% of their baseline body weights.
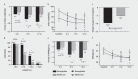
Results: A total of 64 patients completed the study; patients in the beinaglutide group exhibited more bodyweight loss than those in the metformin group [(9.5±0.8%; 9.1±0.9 kg) and (5.1±0.9%; 4.5±0.8 kg), respectively, corresponding to a difference of approximately 4.5 kg (95% confidence interval, 2.2-6.9 kg; P<0.01)]. In the beinaglutide group, 90.6 and 40.6% of the patients lost≥5 and≥10% of their body weight, respectively, whereas, in the metformin group, these rates were 46.9 and 12.5%, respectively (P<0.01 and P<0.05). Weight loss following beinaglutide treatment mainly resulted from the loss of fat mass. Compared to metformin, beinaglutide induced a greater decrease in the body mass index, weight circumference, percent body fat, and body fat mass (total, trunk, limb, android, and gynoid). Additionally, beinaglutide decreased serum insulin levels and ameliorated insulin resistance.
Conclusions: Beinaglutide is more efficient than metformin at reducing weight and fat mass in patients who are overweight/obese and non-diabetic. Beinaglutide may be a useful therapeutic option for overweight/obesity control in the Chinese population.
The Author(s). This is an open access article published by Thieme under the terms of the Creative Commons Attribution-NonDerivative-NonCommercial-License, permitting copying and reproduction so long as the original work is given appropriate credit. Contents may not be used for commercial purposes, or adapted, remixed, transformed or built upon. (https://creativecommons.org/licenses/by-nc-nd/4.0/).
Conflict of interest statement
All authors have no conflicts of interest, financial ties, or grant support to disclose.
Figures

Similar articles
-
Effect of beinaglutide combined with metformin versus aspart 30 with metformin on metabolic profiles and antidrug antibodies in patients with type 2 diabetes: a randomized clinical trial.Front Endocrinol (Lausanne). 2023 Dec 6;14:1267503. doi: 10.3389/fendo.2023.1267503. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 38125788 Free PMC article. Clinical Trial.
-
Beinaglutide for weight management in Chinese individuals with overweight or obesity: A phase 3 randomized controlled clinical study.Diabetes Obes Metab. 2024 Feb;26(2):690-698. doi: 10.1111/dom.15360. Epub 2023 Nov 9. Diabetes Obes Metab. 2024. PMID: 37945546 Clinical Trial.
-
Short-term effect of beinaglutide combined with metformin versus metformin alone on weight loss and metabolic profiles in obese patients with polycystic ovary syndrome: a pilot randomized trial.Front Endocrinol (Lausanne). 2023 Jun 6;14:1156521. doi: 10.3389/fendo.2023.1156521. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 37347114 Free PMC article. Clinical Trial.
-
Efficacy of Metformin Treatment with Respect to Weight Reduction in Children and Adults with Obesity: A Systematic Review.Drugs. 2018 Dec;78(18):1887-1901. doi: 10.1007/s40265-018-1025-0. Drugs. 2018. PMID: 30511324
-
Role of metformin for weight management in patients without type 2 diabetes.Ann Pharmacother. 2008 Jun;42(6):817-26. doi: 10.1345/aph.1K656. Epub 2008 May 13. Ann Pharmacother. 2008. PMID: 18477733 Review.
Cited by
-
Current status, perceptions, and barriers regarding weight loss approaches in China.Endocrine. 2025 Jul 1. doi: 10.1007/s12020-025-04315-7. Online ahead of print. Endocrine. 2025. PMID: 40593266
-
The efficacy and safety of beinaglutide alone or in combination with insulin glargine in Chinese patients with type 2 diabetes mellitus who are inadequately controlled with oral antihyperglycemic therapy: A multicenter, open-label, randomized trial.J Diabetes. 2023 Oct 20;16(2):e13483. doi: 10.1111/1753-0407.13483. Online ahead of print. J Diabetes. 2023. PMID: 37864379 Free PMC article.
-
Pharmacological Treatments and Natural Biocompounds in Weight Management.Pharmaceuticals (Basel). 2023 Jan 30;16(2):212. doi: 10.3390/ph16020212. Pharmaceuticals (Basel). 2023. PMID: 37139804 Free PMC article. Review.
-
Effect of beinaglutide combined with metformin versus aspart 30 with metformin on metabolic profiles and antidrug antibodies in patients with type 2 diabetes: a randomized clinical trial.Front Endocrinol (Lausanne). 2023 Dec 6;14:1267503. doi: 10.3389/fendo.2023.1267503. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 38125788 Free PMC article. Clinical Trial.
-
GLP-1 receptor agonists for the treatment of obesity: Role as a promising approach.Front Endocrinol (Lausanne). 2023 Feb 1;14:1085799. doi: 10.3389/fendo.2023.1085799. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 36843578 Free PMC article. Review.
References
-
- American Diabetes A Obesity management for the treatment of type 2 diabetes: standards of medical care in diabetes-2020. Diabetes Care. 2020;43:S89–S97. - PubMed
-
- Mertens I L, Gaal L F. Overweight, obesity, and blood pressure: the effects of modest weight reduction. Obesity (Silver Spring, Md.) 2000;8:270–278. - PubMed
-
- Warkentin L M, Das D, Majumdar S R. The effect of weight loss on health-related quality of life: systematic review and meta-analysis of randomized trials. Obesity Rev. 2014;15:169–182. - PubMed
-
- Bray G A, Fruhbeck G, Ryan D H. Management of obesity. Lancet. 2016;387:1947–1956. - PubMed
MeSH terms
Substances
Grants and funding
- National Natural Science Foundation of China/81970704
- National Natural Science Foundation of China/81970689
- National Natural Science Foundation of China/81900787
- National Natural Science Foundation of China/81800752
- National Natural Science Foundation of China/81800719
- National Key Research and Development Program of China/2016YFC1304804
- National Key Research and Development Program of China/2017YFC1309605
- Jiangsu Provincial Key Medical Discipline/ZDXKB2016012
- Key Project of Nanjing Clinical Medical Science, Key Research and Development Program of Jiangsu Province of China/BE2015604
- Key Project of Nanjing Clinical Medical Science, Key Research and Development Program of Jiangsu Province of China/BE2016606
- Medical and Health Research Projects of Nanjing in Jiangsu Province of China/YKK18067
- Project of Standardised Diagnosis and Treatment of Key Diseases in Jiangsu Province of China/2015604
- Natural Science Foundation of Jiangsu Province of China/BK20201115
LinkOut - more resources
Full Text Sources
Medical

