Predictors of changes in cerebral perfusion and oxygenation during obstructive sleep apnea
- PMID: 34873232
- PMCID: PMC8648752
- DOI: 10.1038/s41598-021-02829-4
Predictors of changes in cerebral perfusion and oxygenation during obstructive sleep apnea
Abstract
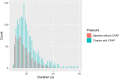
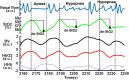
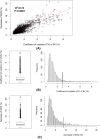
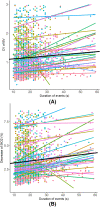
Obstructive sleep apnea syndrome (OSAS) is a common sleep disorder. Severe OSAS defined as apnea-hypopnea index (AHI) ≥ 30/h is a risk factor for developing cerebro-cardiovascular diseases. The mechanisms of how repetitive sleep apneas/hypopneas damage cerebral hemodynamics are still not well understood. In this study, changes in blood volume (BV) and oxygen saturation (StO2) in the left forehead of 29 newly diagnosed severe OSAS patients were measured by frequency-domain near-infrared spectroscopy during an incremental continuous positive airway pressure (CPAP) titration protocol together with polysomnography. The coefficients of variation of BV (CV-BV) and the decreases of StO2 (de-StO2) of more than 2000 respiratory events were predicted using linear mixed-effect models, respectively. We found that longer events and apneas rather than hypopneas induce larger changes in CV-BV and stronger cerebral desaturation. Respiratory events occurring during higher baseline StO2 before their onsets, during rapid-eye-movement sleep and those associated with higher heart rate induce smaller changes in CV-BV and de-StO2. The stepwise increased CPAP pressures can attenuate these changes. These results suggest that in severe OSAS the length and the type of respiratory event rather than widely used AHI may be better parameters to indicate the severity of cerebral hemodynamic changes.
© 2021. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
References
-
- Senaratna CV, et al. Prevalence of obstructive sleep apnea in the general population: A systematic review. Sleep Med. Rev. 2017;34:70–81. - PubMed
-
- Berry RB, et al. The AASM Manual for the Scoring of Sleep and Associated Events: Rules, Terminology and Technical Specifications. American Academy of Sleep Medicine; 2017.

