Ivermectin induces apoptosis of esophageal squamous cell carcinoma via mitochondrial pathway
- PMID: 34876051
- PMCID: PMC8650430
- DOI: 10.1186/s12885-021-09021-x
Ivermectin induces apoptosis of esophageal squamous cell carcinoma via mitochondrial pathway
Abstract
Background: Esophageal squamous cell carcinoma (ESCC) is the most predominant primary malignant tumor among worldwide, especially in China. To date, the successful treatment remains a mainly clinical challenge, it is imperative to develop successful therapeutic agents.
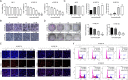
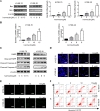
Methods: The anti-proliferative effect of ivermectin on ESCC is investigated in cell model and in nude mice model. Cell apoptosis was assessed using flow cytometry, TUNEL assay and western blotting. Mitochondrial dysfunction was determined by reactive oxygen species accumulation, mitochondrial membrane potential and ATP levels.
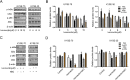
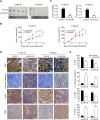
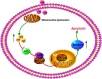
Results: Our results determined that ivermectin significantly inhibited the proliferation of ESCC cells in vitro and in vivo. Furthermore, we found that ivermectin markedly mediated mitochondrial dysfunction and induced apoptosis of ESCC cells, which indicated the anti-proliferative effect of ivermectin on ESCC cells was implicated in mitochondrial apoptotic pathway. Mechanistically, ivermectin significantly triggered ROS accumulation and inhibited the activation of NF-κB signaling pathway and increased the ratio of Bax/Bcl-2.
Conclusions: These finding indicated that ivermectin has significant anti-tumour potential for ESSC and may be a potential therapeutic candidate against ESCC.
Keywords: Apoptosis; ESCC; Ivermectin; Mitochondrial; NF-κB.
© 2021. The Author(s).
Conflict of interest statement
The authors declare that there is no conflict of interest.
Figures

Similar articles
-
Ivermectin suppresses tumour growth and metastasis through degradation of PAK1 in oesophageal squamous cell carcinoma.J Cell Mol Med. 2020 May;24(9):5387-5401. doi: 10.1111/jcmm.15195. Epub 2020 Mar 31. J Cell Mol Med. 2020. PMID: 32237037 Free PMC article.
-
α-Hederin Induces Apoptosis of Esophageal Squamous Cell Carcinoma via an Oxidative and Mitochondrial-Dependent Pathway.Dig Dis Sci. 2019 Dec;64(12):3528-3538. doi: 10.1007/s10620-019-05689-1. Epub 2019 Jul 4. Dig Dis Sci. 2019. PMID: 31273592
-
IFI6 depletion inhibits esophageal squamous cell carcinoma progression through reactive oxygen species accumulation via mitochondrial dysfunction and endoplasmic reticulum stress.J Exp Clin Cancer Res. 2020 Jul 29;39(1):144. doi: 10.1186/s13046-020-01646-3. J Exp Clin Cancer Res. 2020. PMID: 32727517 Free PMC article.
-
The 3-deoxysappanchalcone induces ROS-mediated apoptosis and cell cycle arrest via JNK/p38 MAPKs signaling pathway in human esophageal cancer cells.Phytomedicine. 2021 Jun;86:153564. doi: 10.1016/j.phymed.2021.153564. Epub 2021 Apr 4. Phytomedicine. 2021. PMID: 33895649
-
Triptolide reverses cis‑diamminedichloroplatinum resistance in esophageal squamous cell carcinoma by suppressing glycolysis and causing mitochondrial malfunction.Mol Med Rep. 2025 Mar;31(3):74. doi: 10.3892/mmr.2025.13439. Epub 2025 Jan 31. Mol Med Rep. 2025. PMID: 39886972 Free PMC article.
Cited by
-
Ivermectin and gemcitabine combination treatment induces apoptosis of pancreatic cancer cells via mitochondrial dysfunction.Front Pharmacol. 2022 Aug 26;13:934746. doi: 10.3389/fphar.2022.934746. eCollection 2022. Front Pharmacol. 2022. PMID: 36091811 Free PMC article.
-
Hepatocyte-Conditional Knockout of Phosphatidylethanolamine Binding Protein 4 Aggravated LPS/D-GalN-Induced Acute Liver Injury via the TLR4/NF-κB Pathway.Front Immunol. 2022 Jul 8;13:901566. doi: 10.3389/fimmu.2022.901566. eCollection 2022. Front Immunol. 2022. PMID: 35874667 Free PMC article.
-
Ivermectin Synergizes with Modulated Electro-hyperthermia and Improves Its Anticancer Effects in a Triple-Negative Breast Cancer Mouse Model.ACS Pharmacol Transl Sci. 2024 Jul 17;7(8):2496-2506. doi: 10.1021/acsptsci.4c00314. eCollection 2024 Aug 9. ACS Pharmacol Transl Sci. 2024. PMID: 39144564 Free PMC article.
-
Ivermectin induces cell cycle arrest and caspase-dependent apoptosis in human urothelial carcinoma cells.Int J Med Sci. 2022 Sep 11;19(10):1567-1575. doi: 10.7150/ijms.76623. eCollection 2022. Int J Med Sci. 2022. PMID: 36185334 Free PMC article.
-
Unraveling the Complexity of Regulated Cell Death in Esophageal Cancer: from Underlying Mechanisms to Targeted Therapeutics.Int J Biol Sci. 2023 Jul 31;19(12):3831-3868. doi: 10.7150/ijbs.85753. eCollection 2023. Int J Biol Sci. 2023. PMID: 37564206 Free PMC article. Review.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

