Clinical characteristics and outcomes of COVID-19 patients admitted to the intensive care unit during the first year of the pandemic in Brazil: a single center retrospective cohort study
- PMID: 34878071
- PMCID: PMC8664289
- DOI: 10.31744/einstein_journal/2021AO6739
Clinical characteristics and outcomes of COVID-19 patients admitted to the intensive care unit during the first year of the pandemic in Brazil: a single center retrospective cohort study
Abstract
Objective: To describe clinical characteristics, resource use, outcomes, and to identify predictors of in-hospital mortality of patients with COVID-19 admitted to the intensive care unit.
Methods: Retrospective single-center cohort study conducted at a private hospital in São Paulo (SP), Brazil. All consecutive adult (≥18 years) patients admitted to the intensive care unit, between March 4, 2020 and February 28, 2021 were included in this study. Patients were categorized between survivors and non-survivors according to hospital discharge.
Results: During the study period, 1,296 patients [median (interquartile range) age: 66 (53-77) years] with COVID-19 were admitted to the intensive care unit. Out of those, 170 (13.6%) died at hospital (non-survivors) and 1,078 (86.4%) were discharged (survivors). Compared to survivors, non-survivors were older [80 (70-88) versus 63 (50-74) years; p<0.001], had a higher Simplified Acute Physiology Score 3 [59 (54-66) versus 47 (42-53) points; p<0.001], and presented comorbidities more frequently. During the intensive care unit stay, 56.6% of patients received noninvasive ventilation, 32.9% received mechanical ventilation, 31.3% used high flow nasal cannula, 11.7% received renal replacement therapy, and 1.5% used extracorporeal membrane oxygenation. Independent predictors of in-hospital mortality included age, Sequential Organ Failure Assessment score, Charlson Comorbidity Index, need for mechanical ventilation, high flow nasal cannula, renal replacement therapy, and extracorporeal membrane oxygenation support.
Conclusion: Patients with severe COVID-19 admitted to the intensive care unit exhibited a considerable morbidity and mortality, demanding substantial organ support, and prolonged intensive care unit and hospital stay.
Objetivo:: Descrever características clínicas, uso de recursos e desfechos e identificar preditores de mortalidade intra-hospitalar de pacientes com COVID-19 admitidos na unidade de terapia intensiva.
Métodos:: Estudo de coorte retrospectivo, em centro único, realizado em um hospital privado localizado em São Paulo (SP). Pacientes adultos (≥18 anos) admitidos consecutivamente na unidade de terapia intensiva, entre 4 de março de 2020 a 28 de fevereiro de 2021, foram incluídos neste estudo. Os pacientes foram classificados como sobreviventes e não sobreviventes, de acordo com a alta hospitalar.
Resultados:: Durante o período do estudo, 1.296 pacientes [mediana (intervalo interquartil) de idade: 66 (53-77) anos] com COVID-19 foram admitidos na unidade de terapia intensiva. Destes, 170 (13,6%) pacientes morreram no hospital (não sobreviventes), e 1.078 (86,4%) receberam alta hospitalar (sobreviventes). Comparados aos sobreviventes, os não sobreviventes eram mais idosos [80 (70-88) versus 63 (50-74) anos; p<0,001], apresentavam pontuação mais alta no sistema prognóstico Simplified Acute Physiology Score 3 [59 (54-66) versus 47 (42-53); pontos p<0,001] e tinham mais comorbidades. Durante a internação na unidade de terapia intensiva, 56,6% dos pacientes usaram ventilação não invasiva, 32,9% usaram ventilação mecânica invasiva, 31,3% usaram cateter nasal de alto fluxo, 11,7% foram submetidos à terapia renal substitutiva, e 1,5% usou oxigenação por membrana extracorpórea. Os preditores independentes de mortalidade intra-hospitalar foram idade, Sequential Organ Failure Assessment, Índice de Comorbidade de Charlson, necessidade de ventilação mecânica, uso de cateter nasal de alto fluxo, uso de terapia renal substitutiva e suporte por oxigenação por membrana extracorpórea.
Conclusão:: Pacientes com quadros graves da COVID-19 admitidos na unidade de terapia intensiva apresentaram considerável mortalidade e morbidade, com alta demanda de terapia de suporte e internação prolongada em unidade de terapia intensiva e hospitalar.
Conflict of interest statement
none.
Figures

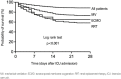

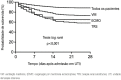
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

