An early model to predict the risk of gestational diabetes mellitus in the absence of blood examination indexes: application in primary health care centres
- PMID: 34879850
- PMCID: PMC8653559
- DOI: 10.1186/s12884-021-04295-2
An early model to predict the risk of gestational diabetes mellitus in the absence of blood examination indexes: application in primary health care centres
Abstract
Background: Gestational diabetes mellitus (GDM) is one of the critical causes of adverse perinatal outcomes. A reliable estimate of GDM in early pregnancy would facilitate intervention plans for maternal and infant health care to prevent the risk of adverse perinatal outcomes. This study aims to build an early model to predict GDM in the first trimester for the primary health care centre.
Methods: Characteristics of pregnant women in the first trimester were collected from eastern China from 2017 to 2019. The univariate analysis was performed using SPSS 23.0 statistical software. Characteristics comparison was applied with Mann-Whitney U test for continuous variables and chi-square test for categorical variables. All analyses were two-sided with p < 0.05 indicating statistical significance. The train_test_split function in Python was used to split the data set into 70% for training and 30% for test. The Random Forest model and Logistic Regression model in Python were applied to model the training data set. The 10-fold cross-validation was used to assess the model's performance by the areas under the ROC Curve, diagnostic accuracy, sensitivity, and specificity.
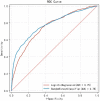
Results: A total of 1,139 pregnant women (186 with GDM) were included in the final data analysis. Significant differences were observed in age (Z=-2.693, p=0.007), pre-pregnancy BMI (Z=-5.502, p<0.001), abdomen circumference in the first trimester (Z=-6.069, p<0.001), gravidity (Z=-3.210, p=0.001), PCOS (χ2=101.024, p<0.001), irregular menstruation (χ2=6.578, p=0.010), and family history of diabetes (χ2=15.266, p<0.001) between participants with GDM or without GDM. The Random Forest model achieved a higher AUC than the Logistic Regression model (0.777±0.034 vs 0.755±0.032), and had a better discrimination ability of GDM from Non-GDMs (Sensitivity: 0.651±0.087 vs 0.683±0.084, Specificity: 0.813±0.075 vs 0.736±0.087).
Conclusions: This research developed a simple model to predict the risk of GDM using machine learning algorithm based on pre-pregnancy BMI, abdomen circumference in the first trimester, age, PCOS, gravidity, irregular menstruation, and family history of diabetes. The model was easy in operation, and all predictors were easily obtained in the first trimester in primary health care centres.
Keywords: Gestational diabetes mellitus; Machine Learning; Maternal and infant health care; Prediction model; Primary health care centre.
© 2021. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures


Similar articles
-
Establishment of gestational diabetes risk prediction model and clinical verification.J Endocrinol Invest. 2024 May;47(5):1281-1287. doi: 10.1007/s40618-023-02249-3. Epub 2023 Dec 12. J Endocrinol Invest. 2024. PMID: 38085430 Free PMC article.
-
Development and validation of a risk prediction model for gestational diabetes mellitus in women of advanced maternal age during the first trimester.FASEB J. 2025 Jan 31;39(2):e70334. doi: 10.1096/fj.202402129R. FASEB J. 2025. PMID: 39825726
-
Early Prediction of Gestational Diabetes Mellitus in the Chinese Population via Advanced Machine Learning.J Clin Endocrinol Metab. 2021 Mar 8;106(3):e1191-e1205. doi: 10.1210/clinem/dgaa899. J Clin Endocrinol Metab. 2021. PMID: 33351102 Free PMC article.
-
Gestational diabetes mellitus risk score: A practical tool to predict gestational diabetes mellitus risk in Tanzania.Diabetes Res Clin Pract. 2018 Nov;145:130-137. doi: 10.1016/j.diabres.2018.05.001. Epub 2018 May 28. Diabetes Res Clin Pract. 2018. PMID: 29852237 Review.
-
A Novel Early Pregnancy Risk Prediction Model for Gestational Diabetes Mellitus.Fetal Diagn Ther. 2019;45(2):76-84. doi: 10.1159/000486853. Epub 2018 Jun 13. Fetal Diagn Ther. 2019. PMID: 29898442 Review.
Cited by
-
MIDO GDM: an innovative artificial intelligence-based prediction model for the development of gestational diabetes in Mexican women.Sci Rep. 2023 Apr 28;13(1):6992. doi: 10.1038/s41598-023-34126-7. Sci Rep. 2023. PMID: 37117235 Free PMC article.
-
Low muscle mass index is associated with type 2 diabetes risk in a Latin-American population: a cross-sectional study.Front Nutr. 2024 Jul 30;11:1448834. doi: 10.3389/fnut.2024.1448834. eCollection 2024. Front Nutr. 2024. PMID: 39139651 Free PMC article.
-
Predicting Gestational Diabetes Mellitus in the first trimester using machine learning algorithms: a cross-sectional study at a hospital fertility health center in Iran.BMC Med Inform Decis Mak. 2025 Jan 3;25(1):3. doi: 10.1186/s12911-024-02799-3. BMC Med Inform Decis Mak. 2025. PMID: 39754258 Free PMC article.
-
Prediction of gestational diabetes mellitus by different obesity indices.BMC Pregnancy Childbirth. 2022 Apr 6;22(1):288. doi: 10.1186/s12884-022-04615-0. BMC Pregnancy Childbirth. 2022. PMID: 35387610 Free PMC article.
-
A Theoretical Exploration of Artificial Intelligence's Impact on Feto-Maternal Health from Conception to Delivery.Int J Womens Health. 2024 May 22;16:903-915. doi: 10.2147/IJWH.S454127. eCollection 2024. Int J Womens Health. 2024. PMID: 38800118 Free PMC article. Review.
References
-
- Hod M, Kapur A, Sacks DA, et al. The International Federation of Gynecology and Obstetrics (FIGO) Initiative on gestational diabetes mellitus: A pragmatic guide for diagnosis, management, and care. Int J Gynaecol Obstet. 2015;131(Suppl 3):S173–S211. doi: 10.1016/S0020-7292(15)30033-3. - DOI - PubMed
-
- Agarwal P, Morriseau TS, Kereliuk SM, Doucette CA, Wicklow BA, Dolinsky VW. Maternal obesity, diabetes during pregnancy and epigenetic mechanisms that influence the developmental origins of cardiometabolic disease in the offspring. Crit Rev Clin Lab Sci. 2018;55:71–101. doi: 10.1080/10408363.2017.1422109. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

