Differences in Characteristics, Hospital Care, and Outcomes between Acute Critically Ill Emergency Department Patients Receiving Palliative Care and Usual Care
- PMID: 34886271
- PMCID: PMC8656613
- DOI: 10.3390/ijerph182312546
Differences in Characteristics, Hospital Care, and Outcomes between Acute Critically Ill Emergency Department Patients Receiving Palliative Care and Usual Care
Abstract
Background: The early integration of palliative care in the emergency department (ED-PC) provides several benefits, including improved quality of life with optimal comfort measures, and symptom control. Whether palliative care could affect the intensive care unit admissions, hospital care and resource utilization requires further investigation.
Aim: To determine the differences in inpatient characteristics, hospital care, survival, and resource utilization between patients receiving palliative care (ED-PC) and usual care (UC).
Design: Retrospective observational study.
Setting/participants: We enrolled consecutive, acute, critically ill patients admitted to the emergency intensive care unit at Taipei Veterans General Hospital from 1 February 2018 to 31 January 2020.
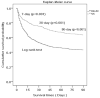
Results: A total of 1273 patients were evaluated for unmet palliative care needs; 685 patients received ED-PC and 588 received UC. The palliative care patients were more severely frail (AOR 2.217 (1.295-3.797), p = 0.004), had functional deterioration with three ADLs (AOR 1.348 (1.040-1.748), p = 0.024), biopsychosocial discomfort (AOR 1.696 (1.315-2.187), p < 0.001), higher Taiwan Triage and Acuity Scale 1 (p = 0.024), higher in-hospital mortality (AOR 1.983 (1.540-2.555), p < 0.001), were four times more likely to sign an DNR (AOR 4.536 (2.522-8.158), p < 0.001), and were twice as likely to sign an DNR at admission (AOR 2.1331.619-2.811), p < 0.001). Palliative care patients received less epinephrine (AOR 0.424 (0.265-0.678), p < 0.001), more frequent withdrawal of an endotracheal tube (AOR 8.780 (1.122-68.720), p = 0.038), and more narcotics (AOR1.675 (1.132-2.477), p = 0.010). Palliative care patients exhibited lower 7-day, 30-day, and 90-day survival rates (p < 0.001). There was no significant difference in the hospital length of stay (LOS) (21.2 ± 26.6 vs. 21.7 ± 20.6, p = 0.709) nor total hospital expenses (293,169 ± 350,043 vs. 294,161 ± 315,275, p = 0.958).
Conclusion: Acute critically ill patients receiving palliative care were more frail, more critical, and had higher in-hospital mortality. Palliative care patients received less epinephrine, more endotracheal extubation, and more narcotics. There was no difference in the hospital LOS or hospital costs between the palliative and usual care groups. The synthesis of ED-PC is new but achievable with potential benefits to align care with patient goals.
Keywords: emergency department; end-of-life care; palliative care.
Conflict of interest statement
We declare there is no conflict of interest.
Figures
References
-
- World Health Organization Palliative Care. [(accessed on 30 January 2009)]. Available online: http://www.who.int/cancer/palliative/definition/en/
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical