Efficacy of Boron Neutron Capture Therapy in Primary Central Nervous System Lymphoma: In Vitro and In Vivo Evaluation
- PMID: 34943904
- PMCID: PMC8699713
- DOI: 10.3390/cells10123398
Efficacy of Boron Neutron Capture Therapy in Primary Central Nervous System Lymphoma: In Vitro and In Vivo Evaluation
Abstract
Background: Boron neutron capture therapy (BNCT) is a nuclear reaction-based tumor cell-selective particle irradiation method. High-dose methotrexate and whole-brain radiation therapy (WBRT) are the recommended treatments for primary central nervous system lymphoma (PCNSL). This tumor responds well to initial treatment but relapses even after successful treatment, and the prognosis is poor as there is no safe and effective treatment for relapse. In this study, we aimed to conduct basic research to explore the possibility of using BNCT as a treatment for PCNSL.
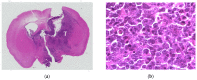
Methods: The boron concentration in human lymphoma cells was measured. Subsequently, neutron irradiation experiments on lymphoma cells were conducted. A mouse central nervous system (CNS) lymphoma model was created to evaluate the biodistribution of boron after the administration of borono-phenylalanine as a capture agent. In the neutron irradiation study of a mouse PCNSL model, the therapeutic effect of BNCT on PCNSL was evaluated in terms of survival.
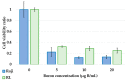
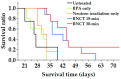
Results: The boron uptake capability of human lymphoma cells was sufficiently high both in vitro and in vivo. In the neutron irradiation study, the BNCT group showed a higher cell killing effect and prolonged survival compared with the control group.
Conclusions: A new therapeutic approach for PCNSL is urgently required, and BNCT may be a promising treatment for PCNSL. The results of this study, including those of neutron irradiation, suggest success in the conduct of future clinical trials to explore the possibility of BNCT as a new treatment option for PCNSL.
Keywords: boron neutron capture therapy (BNCT); malignant brain tumor; primary central nervous system lymphoma (PCNSL); radiation therapy.
Conflict of interest statement
The authors declare no conflict of interest.
Figures




Similar articles
-
Boron neutron capture therapy induces apoptosis of glioma cells through Bcl-2/Bax.BMC Cancer. 2010 Dec 2;10:661. doi: 10.1186/1471-2407-10-661. BMC Cancer. 2010. PMID: 21122152 Free PMC article.
-
Accelerator-based boron neutron capture therapy for malignant glioma: a pilot neutron irradiation study using boron phenylalanine, sodium borocaptate and liposomal borocaptate with a heterotopic U87 glioblastoma model in SCID mice.Int J Radiat Biol. 2020 Jul;96(7):868-878. doi: 10.1080/09553002.2020.1761039. Epub 2020 May 12. Int J Radiat Biol. 2020. PMID: 32339057
-
Boron neutron capture therapy delays the decline in neurological function in a mouse model of metastatic spinal tumors.Cancer Sci. 2024 Aug;115(8):2774-2785. doi: 10.1111/cas.16245. Epub 2024 Jun 11. Cancer Sci. 2024. PMID: 38860412 Free PMC article.
-
4-Borono-2-18F-fluoro-L-phenylalanine PET for boron neutron capture therapy-oriented diagnosis: overview of a quarter century of research.Ann Nucl Med. 2019 Apr;33(4):223-236. doi: 10.1007/s12149-019-01347-8. Epub 2019 Feb 28. Ann Nucl Med. 2019. PMID: 30820862 Free PMC article. Review.
-
In silico assessments of the small molecular boron agents to pave the way for artificial intelligence-based boron neutron capture therapy.Eur J Med Chem. 2024 Dec 5;279:116841. doi: 10.1016/j.ejmech.2024.116841. Epub 2024 Sep 6. Eur J Med Chem. 2024. PMID: 39244862 Review.
Cited by
-
L-Boronphenylalanine Biodistribution Dynamics in the Organs of Mice with Subcutaneous Tumor Xenograft is a Model to Assess Neuron Sources Efficiency in Boron Neutron Capture Therapy.Sovrem Tekhnologii Med. 2023;15(6):14-20. doi: 10.17691/stm2023.15.6.02. Epub 2023 Dec 27. Sovrem Tekhnologii Med. 2023. PMID: 39944369 Free PMC article.
-
Optimizing Boron Neutron Capture Therapy (BNCT) to Treat Cancer: An Updated Review on the Latest Developments on Boron Compounds and Strategies.Cancers (Basel). 2023 Aug 14;15(16):4091. doi: 10.3390/cancers15164091. Cancers (Basel). 2023. PMID: 37627119 Free PMC article. Review.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

