COVID-19-Associated Pulmonary Aspergillosis in Russia
- PMID: 34947041
- PMCID: PMC8705636
- DOI: 10.3390/jof7121059
COVID-19-Associated Pulmonary Aspergillosis in Russia
Abstract
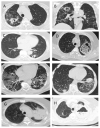
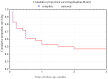
We studied the risk factors, etiology, clinical features and the effectiveness of therapy of COVID-19-associated pulmonary aspergillosis (CAPA) in adult patients. In this retrospective study, we included 45 patients with proven (7%) and probable (93%) CAPA. The ECMM/ISHAM, 2020 criteria were used to diagnose CAPA. A case-control study was conducted to study the risk factors of CAPA; the control group included 90 adult COVID-19 patients without IA. In CAPA patients, the main underlying diseases were diabetes mellitus (33%), and hematological and oncological diseases (31%). The probability of CAPA developing significantly increased with lymphocytopenia >10 days (OR = 8.156 (3.056-21.771), p = 0.001), decompensated diabetes mellitus (29% vs. 7%, (OR = 5.688 (1.991-16.246), p = 0.001)), use of glucocorticosteroids (GCS) in prednisolone-equivalent dose > 60 mg/day (OR = 4.493 (1.896-10.647), p = 0.001) and monoclonal antibodies to IL-1ß and IL-6 (OR = 2.880 (1.272-6.518), p = 0.01). The main area of localization of CAPA was the lungs (100%). The clinical features of CAPA were fever (98% vs. 85%, p = 0.007), cough (89% vs. 72%, p = 0.002) and hemoptysis (36% vs. 3%, p = 0.0001). Overall, 71% of patients were in intensive care units (ICU) (median-15.5 (5-60) days), mechanical ventilation was used in 52% of cases, and acute respiratory distress syndrome (ARDS) occurred at a rate of 31%. The lung CT scan features of CAPA were bilateral (93%) lung tissue consolidation (89% vs. 59%, p = 0.004) and destruction (47% vs. 1%, p = 0.00001), and hydrothorax (26% vs. 11%, p = 0.03). The main pathogens were A. fumigatus (44%) and A. niger (31%). The overall survival rate after 12 weeks was 47.2%.
Keywords: Aspergillus spp.; CAPA; COVID-19; COVID-19-associated pulmonary aspergillosis; invasive aspergillosis.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
-
- Schauwvlieghe A.F.A.D., Rijnders B.J.A., Philips N., Verwijs R., Vanderbeke L., Van Tienen C., Lagrou K., Verweij P.E., Van De Veerdonk F.L., Gommers D., et al. Invasive aspergillosis in patients admitted to the intensive care unit with severe influenza: A retrospective cohort study. Lancet Respir. Med. 2018;6:782–792. doi: 10.1016/S2213-2600(18)30274-1. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

