Physiological aspects of cardiopulmonary dysanapsis on exercise in adults born preterm
- PMID: 34961925
- PMCID: PMC9036864
- DOI: 10.1113/JP281848
Physiological aspects of cardiopulmonary dysanapsis on exercise in adults born preterm
Abstract
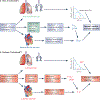
Progressive improvements in perinatal care and respiratory management of preterm infants have resulted in increased survival of newborns of extremely low gestational age over the past few decades. However, the incidence of bronchopulmonary dysplasia, the chronic lung disease after preterm birth, has not changed. Studies of the long-term follow-up of adults born preterm have shown persistent abnormalities of respiratory, cardiovascular and cardiopulmonary function, possibly leading to a lower exercise capacity. The underlying causes of these abnormalities are incompletely known, but we hypothesize that dysanapsis, i.e. discordant growth and development, in the respiratory and cardiovascular systems is a central structural feature that leads to a lower exercise capacity in young adults born preterm than those born at term. We discuss how the hypothesized system dysanapsis underscores the observed respiratory, cardiovascular and cardiopulmonary limitations. Specifically, adults born preterm have: (1) normal lung volumes but smaller airways, which causes expiratory airflow limitation and abnormal respiratory mechanics but without impacts on pulmonary gas exchange efficiency; (2) normal total cardiac size but smaller cardiac chambers; and (3) in some cases, evidence of pulmonary hypertension, particularly during exercise, suggesting a reduced pulmonary vascular capacity despite reduced cardiac output. We speculate that these underlying developmental abnormalities may accelerate the normal age-associated decline in exercise capacity, via an accelerated decline in respiratory, cardiovascular and cardiopulmonary function. Finally, we suggest areas of future research, especially the need for longitudinal and interventional studies from infancy into adulthood to better understand how preterm birth alters exercise capacity across the lifespan.
Keywords: bronchopulmonary dysplasia; cardiac development; exercise physiology; extremely low gestational age newborns; lung development; prematurity; pulmonary hypertension.
© 2021 The Authors. The Journal of Physiology © 2021 The Physiological Society.
Conflict of interest statement
Figures
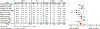
Similar articles
-
Respiratory and cardiopulmonary limitations to aerobic exercise capacity in adults born preterm.J Appl Physiol (1985). 2020 Oct 1;129(4):718-724. doi: 10.1152/japplphysiol.00419.2020. Epub 2020 Aug 13. J Appl Physiol (1985). 2020. PMID: 32790592 Free PMC article. Review.
-
Premature birth affects the degree of airway dysanapsis and mechanical ventilatory constraints.Exp Physiol. 2018 Feb 1;103(2):261-275. doi: 10.1113/EP086588. Epub 2017 Dec 20. Exp Physiol. 2018. PMID: 29193495
-
Normal pulmonary gas exchange efficiency and absence of exercise-induced arterial hypoxemia in adults with bronchopulmonary dysplasia.J Appl Physiol (1985). 2013 Oct 1;115(7):1050-6. doi: 10.1152/japplphysiol.00592.2013. Epub 2013 Jul 18. J Appl Physiol (1985). 2013. PMID: 23869070
-
Pulmonary Gas Exchange and Exercise Capacity in Adults Born Preterm.Ann Am Thorac Soc. 2015 Aug;12(8):1130-7. doi: 10.1513/AnnalsATS.201410-470OC. Ann Am Thorac Soc. 2015. PMID: 26053283 Free PMC article.
-
Impact of preterm birth and bronchopulmonary dysplasia on the developing lung: long-term consequences for respiratory health.Clin Exp Pharmacol Physiol. 2013 Nov;40(11):765-73. doi: 10.1111/1440-1681.12068. Clin Exp Pharmacol Physiol. 2013. PMID: 23414429 Review.
Cited by
-
Reply to Tepper et al.: Additional Thoughts on Intrinsic Dysanapsis.Am J Respir Crit Care Med. 2024 Apr 15;209(8):1041-1042. doi: 10.1164/rccm.202312-2345LE. Am J Respir Crit Care Med. 2024. PMID: 38301260 Free PMC article. No abstract available.
-
Dysanapsis as a Determinant of Lung Function in Development and Disease.Am J Respir Crit Care Med. 2023 Nov 1;208(9):956-963. doi: 10.1164/rccm.202306-1120PP. Am J Respir Crit Care Med. 2023. PMID: 37677135 Free PMC article. No abstract available.
-
Cardiac dysfunction during exercise in young adults with bronchopulmonary dysplasia.ERJ Open Res. 2024 Jun 17;10(3):00501-2023. doi: 10.1183/23120541.00501-2023. eCollection 2024 May. ERJ Open Res. 2024. PMID: 38887679 Free PMC article.
-
The tryptophan metabolite 3-hydroxyanthranilic acid alleviates hyperoxia-induced bronchopulmonary dysplasia via inhibiting ferroptosis.Redox Biol. 2025 May;82:103579. doi: 10.1016/j.redox.2025.103579. Epub 2025 Mar 8. Redox Biol. 2025. PMID: 40117887 Free PMC article.
-
Differing Impact of Preterm Birth on the Right and Left Atria in Adulthood.J Am Heart Assoc. 2022 Dec 6;11(23):e027305. doi: 10.1161/JAHA.122.027305. Epub 2022 Dec 1. J Am Heart Assoc. 2022. PMID: 36453643 Free PMC article.
References
-
- Abman SH, Bancalari E & Jobe A (2017b). The Evolution of Bronchopulmonary Dysplasia after 50 Years. Am J Respir Crit Care Med 195, 421–424. - PubMed
-
- Abman SH, Wolfe RR, Accurso FJ, Koops BL, Bowman CM & Wiggins JW (1985). Pulmonary vascular response to oxygen in infants with severe bronchopulmonary dysplasia. Pediatrics 75, 80–84. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

