Effects of a National Quality Improvement Collaborative on ABCDEF Bundle Implementation
- PMID: 34972842
- PMCID: PMC9972543
- DOI: 10.4037/ajcc2022768
Effects of a National Quality Improvement Collaborative on ABCDEF Bundle Implementation
Abstract
Background: The ABCDEF bundle (Assess, prevent, and manage pain and Delirium; Both spontaneous awakening and breathing trials; Choice of analgesia/sedation; Early mobility; and Family engagement) improves intensive care unit outcomes, but adoption into practice is poor.
Objective: To assess the effect of quality improvement collaborative participation on ABCDEF bundle performance.
Methods: This interrupted time series analysis included 20 months of bundle performance data from 15 226 adults admitted to 68 US intensive care units. Segmented regression models were used to quantify complete and individual bundle element performance changes over time and compare performance patterns before (6 months) and after (14 months) collaborative initiation.
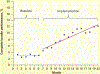
Results: Complete bundle performance rates were very low at baseline (<4%) but increased to 12% by the end. Complete bundle performance increased by 2 percentage points (SE, 0.9; P = .06) immediately after collaborative initiation. Each subsequent month was associated with an increase of 0.6 percentage points (SE, 0.2; P = .04). Performance rates increased significantly immediately after initiation for pain assessment (7.6% [SE, 2.0%], P = .002), sedation assessment (9.1% [SE, 3.7%], P = .02), and family engagement (7.8% [SE, 3%], P = .02) and then increased monthly at the same speed as the trend in the baseline period. Performance rates were lowest for spontaneous awakening/breathing trials and early mobility.
Conclusions: Quality improvement collaborative participation resulted in clinically meaningful, but small and variable, improvements in bundle performance. Opportunities remain to improve adoption of sedation, mechanical ventilation, and early mobility practices.
©2022 American Association of Critical-Care Nurses.
Figures


References
-
- Elliott D, Davidson JE, Harvey MA, et al. Exploring the scope of post-intensive care syndrome therapy and care: engagement of non-critical care providers and survivors in a second stakeholders meeting. Crit Care Med. 2014;42(12): 2518–2526. - PubMed
-
- Needham DM, Davidson J, Cohen H, et al. Improving long-term outcomes after discharge from intensive care unit: report from a stakeholders’ conference. Crit Care Med. 2012; 40(2):502–509. - PubMed
-
- Barr J, Fraser GL, Puntillo K, et al. ; American College of Critical Care Medicine. Clinical practice guidelines for the management of pain, agitation, and delirium in adult patients in the intensive care unit. Crit Care Med. 2013;41(1):263–306. - PubMed

