Post-LASIK keratectasia in the context of a thicker than intended flap detected by anterior segment optical coherence tomography
- PMID: 34987816
- PMCID: PMC8721368
- DOI: 10.1177/2050313X211050462
Post-LASIK keratectasia in the context of a thicker than intended flap detected by anterior segment optical coherence tomography
Abstract
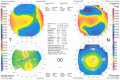
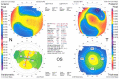
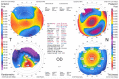
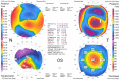
The corneal flap created in LASIK is responsible for most of its advantages in comparison with surface ablation. However, lamellar dissection of the corneal layers in LASIK can also result in serious complications such as corneal ectasia. A 23-year-old man underwent LASIK for correction of -4.75 -2.00@15 in the right eye and -4.50 -2.00@160 in the left eye with a preoperative thinnest corneal thickness of 518 µm/right eye and 513 µm/left eye in 2009. An intended flap thickness and ablation depth in both eyes were 160 µm and 94 µm, respectively, and subsequently, residual stromal bed thickness was 264 µm/right eye and 259 µm/left eye. Several years after surgery, he was referred for the decreased vision. His corrected-distance visual acuity was 0.50 in both eyes. A scissoring reflex was found in retinoscopy. Orbscan imaging was compatible with keratoconus. Anterior segment optical coherence tomography was performed to measure the LASIK flap. It was much thicker (200 µm) than intended (160 µm), and therefore, the residual stromal bed thickness was much thinner. In summary, keratectasia may develop in cases where thicker than expected flaps result in excessive thinning of the residual stromal bed. The obtained results from this case emphasize and remind the importance of intraoperative measurement of flap thickness and using femtosecond and new criteria for patient selection to avoid post-LASIK keratectasia.
Keywords: LASIK; flap thickness; keratectasia; keratoconus; residual stromal bed thickness.
© The Author(s) 2021.
Conflict of interest statement
Declaration of conflicting interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures

Similar articles
-
Keratectasia after laser in situ keratomileusis (LASIK): evaluation of the calculated residual stromal bed thickness.Am J Ophthalmol. 2002 Nov;134(5):771-3. doi: 10.1016/s0002-9394(02)01656-2. Am J Ophthalmol. 2002. PMID: 12429260
-
Posterior corneal curvature changes after undersurface ablation of the flap and in-the-bed LASIK retreatment.Ophthalmology. 2006 Jul;113(7):1125-33. doi: 10.1016/j.ophtha.2006.01.065. Epub 2006 May 19. Ophthalmology. 2006. PMID: 16713626
-
Flap and stromal bed thickness in laser in situ keratomileusis enhancement.J Cataract Refract Surg. 2004 Nov;30(11):2295-302. doi: 10.1016/j.jcrs.2004.02.080. J Cataract Refract Surg. 2004. PMID: 15519078
-
A longitudinal study of LASIK flap and stromal thickness with high-speed optical coherence tomography.Ophthalmology. 2007 Jun;114(6):1124-32. doi: 10.1016/j.ophtha.2006.09.031. Epub 2007 Feb 23. Ophthalmology. 2007. PMID: 17320959
-
[Analysis of flap thickness created with mechanical microkeratome in LASIK by using anterior segment optical coherence tomography].Zhonghua Yan Ke Za Zhi. 2010 Dec;46(12):1104-9. Zhonghua Yan Ke Za Zhi. 2010. PMID: 21211225 Chinese.
Cited by
-
Retinoscopes: Past and present.World J Methodol. 2024 Sep 20;14(3):91497. doi: 10.5662/wjm.v14.i3.91497. eCollection 2024 Sep 20. World J Methodol. 2024. PMID: 39310243 Free PMC article.
-
Comparison of errors in ablation depth calculation after myopic femtosecond laser in situ keratomileusis in patients with different degrees of myopia: a prospective study.BMC Ophthalmol. 2023 Nov 13;23(1):453. doi: 10.1186/s12886-023-03200-z. BMC Ophthalmol. 2023. PMID: 37957578 Free PMC article.
References
-
- Farah SG, Azar DT, Gurdal C, et al.. Laser in situ keratomileusis: literature review of a developing technique. J Cataract Refract Surg 1998; 24: 989–1006. - PubMed
-
- Wellish KL, Glasgow BJ, Beltran F, et al.. Corneal ectasia as a complication of repeated keratotomy surgery. J Refract Corneal Surg 1994; 10(3): 360–364. - PubMed
-
- Speicher L, Göttinger W. Progressive Keratektasie nach Laser-in-situ-Keratomileusis (LASIK). Klin Monatsb Augenheilkd 1998; 213: 247–251. - PubMed
-
- Seiler T, Koufala K, Richter G. Iatrogenic keratectasia after laser in situ keratomileusis. J Refract Surg 1998; 14: 312–317. - PubMed
-
- Javadi MA, Mohammadpour M, Rabei HM. Keratectasia after LASIK but not after PRK in one patient. J Refract Surg 2006; 22(8): 817–820. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

