Healthcare Utilization Among Patients Diagnosed with COVID-19 in a Large Integrated Health System
- PMID: 34993879
- PMCID: PMC8735886
- DOI: 10.1007/s11606-021-07139-z
Healthcare Utilization Among Patients Diagnosed with COVID-19 in a Large Integrated Health System
Abstract
Background: The demands for healthcare resources following a COVID-19 diagnosis are substantial, but not currently quantified.
Objective: To describe trends in healthcare utilization within 180 days for patients diagnosed with COVID-19 and identify patient factors associated with increased healthcare use.
Design: Observational cohort study.
Patients: A total of 64,011 patients with a test-confirmed COVID-19 diagnosis from March to September 2020 in a large integrated healthcare system in Southern California.
Main measures: Overall healthcare utilization during the 180 days following COVID-19 diagnosis, as well as encounter types and reasons for visits during the first 30 days. Poisson regression was used to identify patient factors associated with higher utilization. Analyses were performed separately for patients who were and were not hospitalized for COVID-19.
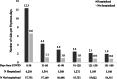
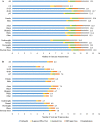
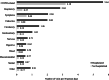
Key results: Healthcare utilization was about twice as high for hospitalized patients compared to non-hospitalized patients in all time periods. The average number of visits was highest in the first 30 days (hospitalized: 12.3 visits/30 person-days; non-hospitalized: 6.6) and gradually decreased over time. In the first 30 days, the majority of healthcare visits were telehealth encounters (hospitalized: 9.0 visits; non-hospitalized: 5.6 visits), and the most prevalent reasons for visits were COVID-related diagnoses, COVID-related symptoms, and respiratory-related conditions. For hospitalized patients, older age (≥65: RR 1.27, 95% CI 1.15-1.41), female gender (RR 1.07, 95% CI 1.05-1.09), and higher BMI (≥40: RR 1.07, 95% CI 1.03-1.10) were associated with higher total utilization. For non-hospitalized patients, older age, female gender, higher BMI, non-white race/ethnicity, former smoking, and greater number of pre-existing comorbidities were all associated with increased utilization.
Conclusions: Patients with COVID-19 seek healthcare frequently within 30 days of diagnosis, placing high demands on health systems. Identifying ways to support patients diagnosed with COVID-19 while adequately providing the usual recommended care to our communities will be important as we recover from the pandemic.
Keywords: COVID-19; SARS-CoV-2; utilization.
© 2021. Society of General Internal Medicine.
Conflict of interest statement
The authors declare that they do not have a conflict of interest.
Figures
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

