Prediction of preeclampsia throughout gestation with maternal characteristics and biophysical and biochemical markers: a longitudinal study
- PMID: 34998477
- PMCID: PMC8749051
- DOI: 10.1016/j.ajog.2021.01.020
Prediction of preeclampsia throughout gestation with maternal characteristics and biophysical and biochemical markers: a longitudinal study
Abstract
Background: The current approach to predict preeclampsia combines maternal risk factors and evidence from biophysical markers (mean arterial pressure, Doppler velocimetry of the uterine arteries) and maternal blood proteins (placental growth factor, soluble vascular endothelial growth factor receptor-1, pregnancy-associated plasma protein A). Such models require the transformation of biomarker data into multiples of the mean values by using population- and site-specific models. Previous studies have focused on a narrow window in gestation and have not included the maternal blood concentration of soluble endoglin, an important antiangiogenic factor up-regulated in preeclampsia.
Objective: This study aimed (1) to develop models for the calculation of multiples of the mean values for mean arterial pressure and biochemical markers; (2) to build and assess the predictive models for preeclampsia based on maternal risk factors, the biophysical (mean arterial pressure) and biochemical (placental growth factor, soluble vascular endothelial growth factor receptor-1, and soluble endoglin) markers collected throughout pregnancy; and (3) to evaluate how prediction accuracy is affected by the presence of chronic hypertension and gestational age.
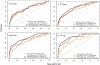
Study design: This longitudinal case-cohort study included 1150 pregnant women: women without preeclampsia with (n=49) and without chronic hypertension (n=871) and those who developed preeclampsia (n=166) or superimposed preeclampsia (n=64). Mean arterial pressure and immunoassay-based maternal plasma placental growth factor, soluble vascular endothelial growth factor receptor-1, and soluble endoglin concentrations were available throughout pregnancy (median of 5 observations per patient). A prior-risk model for preeclampsia was established by using Poisson regression based on maternal characteristics and obstetrical history. Next, multiple regression was used to fit biophysical and biochemical marker data as a function of maternal characteristics by using data collected at 8 to 15+6, 16 to 19+6, 20 to 23+6, 24 to 27+6, 28 to 31+6, and 32 to 36+6 week intervals, and observed values were converted into multiples of the mean values. Then, multivariable prediction models for preeclampsia were fit based on the biomarker multiples of the mean data and prior-risk estimates. Separate models were derived for overall, preterm, and term preeclampsia, which were evaluated by receiver operating characteristic curves and sensitivity at fixed false-positive rates.
Results: (1) The inclusion of soluble endoglin in prediction models for all preeclampsia, together with the prior-risk estimates, mean arterial pressure, placental growth factor, and soluble vascular endothelial growth factor receptor-1, increased the sensitivity (at a fixed false-positive rate of 10%) for early prediction of superimposed preeclampsia, with the largest increase (from 44% to 54%) noted at 20 to 23+6 weeks (McNemar test, P<.05); (2) combined evidence from prior-risk estimates and biomarkers predicted preterm preeclampsia with a sensitivity (false-positive rate, 10%) of 55%, 48%, 62%, 72%, and 84% at 8 to 15+6, 16 to 19+6, 20 to 23+6, 24 to 27+6, and 28 to 31+6 week intervals, respectively; (3) the sensitivity for term preeclampsia (false-positive rate, 10%) was 36%, 36%, 41%, 43%, 39%, and 51% at 8 to 15+6, 16 to 19+6, 20 to 23+6, 24 to 27+6, 28 to 31+6, and 32 to 36+6 week intervals, respectively; (4) the detection rate for superimposed preeclampsia among women with chronic hypertension was similar to that in women without chronic hypertension, especially earlier in pregnancy, reaching at most 54% at 20 to 23+6 weeks (false-positive rate, 10%); and (5) prediction models performed comparably to the Fetal Medicine Foundation calculators when the same maternal risk factors and biomarkers (mean arterial pressure, placental growth factor, and soluble vascular endothelial growth factor receptor-1 multiples of the mean values) were used as input.
Conclusion: We introduced prediction models for preeclampsia throughout pregnancy. These models can be useful to identify women at risk during the first trimester who could benefit from aspirin treatment or later in pregnancy to inform patient management. Relative to prediction performance at 8 to 15+6 weeks, there was a substantial improvement in the detection rate for preterm and term preeclampsia by using data collected after 20 and 32 weeks' gestation, respectively. The inclusion of plasma soluble endoglin improves the early prediction of superimposed preeclampsia, which may be valuable when Doppler velocimetry of the uterine arteries is not available.
Keywords: Poisson regression; aspirin; biomarker; chronic hypertension; placental growth factor; prediction; prevention; soluble Flt; soluble endoglin; soluble vascular endothelial growth factor receptor-1; superimposed preeclampsia; toxemia of pregnancy.
Copyright © 2021 Elsevier Inc. All rights reserved.
Conflict of interest statement
Figures
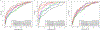

References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

