Utility of the MISDEF2 Algorithm and Extent of Fusion in Open Adult Spinal Deformity Surgery With Minimum 2-Year Follow-up
- PMID: 35000336
- PMCID: PMC8752706
- DOI: 10.14245/ns.2142508.254
Utility of the MISDEF2 Algorithm and Extent of Fusion in Open Adult Spinal Deformity Surgery With Minimum 2-Year Follow-up
Abstract
Objective: Long-segment fusion in adult spinal deformity (ASD) is often needed, but more focal surgeries may provide significant relief with less morbidity. The minimally invasive spinal deformity surgery (MISDEF2) algorithm guides minimally invasive ASD surgery, but it may be useful in open ASD surgery. We classified ASD patients undergoing focal decompression, limited decompression and fusion, and full correction according to MISDEF2 and correlated outcomes.
Methods: A retrospective study of ASD patients treated by 2 surgeons at our hospital was performed. Inclusion criteria were: age > 50, minimum 2-year follow-up, and open ASD surgery. Tumor, trauma, and infections were excluded. Patients had open surgery including focal decompression, short segment fusion, or full scoliosis correction. All patients were categorized by MISDEF2 into 4 classes based upon spinopelvic parameters. Perioperative metrics were assessed. Radiographic correction, complications and reoperation were recorded.
Results: A total of 136 patients met inclusion criteria. Mean follow-up was 46 ± 15.8 months (range, 24-118 months). Forty-seven underwent full deformity correction, 71 underwent short segment fusion, and 18 underwent decompression alone. There were 24 cases of class I, 66 cases of class II, 23 cases of class III, and 23 cases of class IV patients. Patients in class I and II had perioperative complication rates of 0% and 16.7% and revision rates of 8% and 21.2% when undergoing focal decompression or limited fusion. However, class II patients undergoing full correction had higher perioperative complications rate (p = 0.03) and revision surgery rates (p = 0.047). This difference was not seen in class III patients (p > 0.05). All class IV patients underwent full correction, but they had higher perioperative complication rates (p < 0.019), comparable revision surgery rates (p = 0.27), and better radiographic realignment (p < 0.001). In addition, full deformity correction was associated with longer length of stay, increased blood loss, and longer operative time (p < 0.001).
Conclusion: The MISDEF2 algorithm may help guide ASD surgical decision making even in open surgery, with focal treatment used in class I and II patients as a viable alternative and full correction implemented in class IV patients because of severe malalignment. However, class II patients with ASD undergoing full deformity correction do have higher complication rates.
Keywords: Adult spinal deformity; Complications; MISDEF2; Minimally invasive surgery; Outcomes.
Conflict of interest statement
The authors have nothing to disclose.
Figures
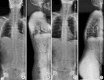

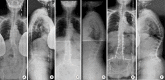

References
-
- Marchesi DG, Aebi M. Pedicle fixation devices in the treatment of adult lumbar scoliosis. Spine (Phila Pa 1976) 1992;17(8 Suppl):S304–9. - PubMed
-
- Tribus CB. Degenerative lumbar scoliosis: evaluation and management. J Am Acad Orthop Surg. 2003;11:174–83. - PubMed
-
- Houten JK, Nasser R. Symptomatic progression of degenerative scoliosis after decompression and limited fusion surgery for lumbar spinal stenosis. J Clin Neurosci. 2013;20:613–5. - PubMed
-
- Transfeldt EE, Topp R, Mehbod AA, et al. Surgical outcomes of decompression, decompression with limited fusion, and decompression with full curve fusion for degenerative scoliosis with radiculopathy. Spine (Phila Pa 1976) 2010;35:1872–5. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

