Nomogram Predicting Overall Survival in Patients with FIGO II to III Squamous Cell Cervical Carcinoma Under Radical Radiotherapy: A Retrospective Analysis Based on 2018 FIGO Staging
- PMID: 35002316
- PMCID: PMC8722567
- DOI: 10.2147/CMAR.S336892
Nomogram Predicting Overall Survival in Patients with FIGO II to III Squamous Cell Cervical Carcinoma Under Radical Radiotherapy: A Retrospective Analysis Based on 2018 FIGO Staging
Abstract
Purpose: To present a nomogram to predict overall survival in patients with FIGO-2018 II to III squamous cell cervical carcinoma undergoing radical radiotherapy.
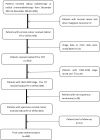
Patients and methods: Patients diagnosed with FIGO-2018 II to III squamous cell cervical cancer between December 2013 and December 2014 were analyzed retrospectively. The optimal cutoff point for tumor length and width were determined by R package. We identified prognostic factors by univariate and multivariate Cox proportional-hazard regression, then built a nomogram to visualize the prediction model. Our model was compared to the 2018 FIGO staging prediction model. Harrell's concordance index, receiver operating characteristic curve, calibration plot were used to evaluate the discriminability and accuracy of the predictive models, and decision curve analysis (DCA) was used to show the net benefits.
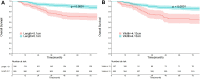
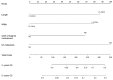
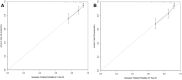
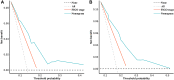
Results: Data from 469 patients were included in the final analyses. The cutoff values of tumor length and width were 5.10 cm and 4.13 cm, respectively. Four independent prognostic variables-tumor length, tumor width, lower one-third vaginal involvement, and lymph node metastases-were used to establish the nomogram. The C-index of the nomogram was 0.71 (95%, CI = 0.66-0.77), which was better than that of the 2018 FIGO stage prediction model (C-index: 0.62, 95% CI = 0.58-0.66, p = 0.009). The calibration plot of the nomogram was a good fit for both 3-year and 5-year overall survival predictions. And DCA curves showed that net benefits for our model were higher than FIGO-2018 staging system.
Conclusion: A clinically useful nomogram for calculating overall survival probability in FIGO-2018 II to III squamous cell cervical cancer patients who had received radical radiotherapy was developed. Tumor length, tumor width, lower one-third vaginal involvement, and lymph node metastases were found to be independent prognostic factors. Our model performed better than the 2018 FIGO staging model. The findings could help clinicians in China to predict the survival of these patients in clinical care and research.
Keywords: cervical carcinoma; nomogram; overall survival; radiotherapy.
© 2021 Zang et al.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Calculating the overall survival probability in patients with cervical cancer: a nomogram and decision curve analysis-based study.BMC Cancer. 2020 Sep 1;20(1):833. doi: 10.1186/s12885-020-07349-4. BMC Cancer. 2020. PMID: 32873257 Free PMC article.
-
A prognostic nomogram based on lymph node ratio for postoperative vulvar squamous cell carcinoma from the Surveillance, Epidemiology, and End Results database: a retrospective cohort study.Ann Transl Med. 2020 Nov;8(21):1382. doi: 10.21037/atm-20-3240. Ann Transl Med. 2020. PMID: 33313127 Free PMC article.
-
A prognostic model using FIGO 2018 staging and MRI-derived tumor volume to predict long-term outcomes in patients with uterine cervical squamous cell carcinoma who received definitive radiotherapy.World J Surg Oncol. 2023 Jul 21;21(1):210. doi: 10.1186/s12957-023-03116-4. World J Surg Oncol. 2023. PMID: 37475053 Free PMC article.
-
Postoperative nomogram for the prediction of disease-free survival in lymph node-negative stage I-IIA cervical cancer patients treated with radical hysterectomy.J Obstet Gynaecol. 2020 Jul;40(5):699-704. doi: 10.1080/01443615.2019.1652888. Epub 2019 Oct 12. J Obstet Gynaecol. 2020. PMID: 31607197
-
Development and validation of a nomogram to predict overall survival of T1 esophageal squamous cell carcinoma patients with lymph node metastasis.Transl Oncol. 2021 Aug;14(8):101127. doi: 10.1016/j.tranon.2021.101127. Epub 2021 May 18. Transl Oncol. 2021. PMID: 34020370 Free PMC article.
Cited by
-
Nomograms Predicting Survival of Cervical Cancer Patients Treated With Concurrent Chemoradiotherapy Based on the 2018 FIGO Staging System.Front Oncol. 2022 May 11;12:870670. doi: 10.3389/fonc.2022.870670. eCollection 2022. Front Oncol. 2022. PMID: 35646645 Free PMC article.
-
Assessing survival time of outpatients with cervical cancer: at the university of Gondar referral hospital using the Bayesian approach.BMC Womens Health. 2023 Feb 10;23(1):59. doi: 10.1186/s12905-023-02202-9. BMC Womens Health. 2023. PMID: 36765315 Free PMC article.
-
Nomogram models for the prognosis of cervical cancer: A SEER-based study.Front Oncol. 2022 Oct 6;12:961678. doi: 10.3389/fonc.2022.961678. eCollection 2022. Front Oncol. 2022. PMID: 36276099 Free PMC article.
-
Integrating Novel and Classical Prognostic Factors in Locally Advanced Cervical Cancer: A Machine Learning-Based Predictive Model (ESTHER Study).J Pers Med. 2025 Apr 15;15(4):153. doi: 10.3390/jpm15040153. J Pers Med. 2025. PMID: 40278332 Free PMC article.
-
Machine Learning of Dose-Volume Histogram Parameters Predicting Overall Survival in Patients with Cervical Cancer Treated with Definitive Radiotherapy.J Oncol. 2022 Jun 14;2022:2643376. doi: 10.1155/2022/2643376. eCollection 2022. J Oncol. 2022. PMID: 35747125 Free PMC article.
References
-
- Ping L. Evaluation of big data of clinical epidemiology of cervical cancer in 13 years in Chinese mainland (in Chinese).Chinese JPractical Gynecology and Obstetrics.. 2018;34(01):41–45.
-
- Toita T, Nakano M, Higashi M, Sakumoto K, Kanazawa K. Prognostic value of cervical size and pelvic lymph node status assessed by computed tomography for pa tients with uterine cervical cancer treated by radical radiation therapy. Int J Radiat Oncol Biol Phys. 1995;33(4):843–849. doi:10.1016/0360-3016(95)00204-5 - DOI - PubMed
-
- Kobierski J, Emerich J, Kr¨®likowska B, Majdak E. [Lymph node metastasis as a prognostic factor in cervical carcinoma]. Ginekol Pol. 2002;73(11):925–929. Polish - PubMed
LinkOut - more resources
Full Text Sources

