Lymph Node Involvement in Early-Stage Cervical Cancer: Is Lymphangiogenesis a Risk Factor? Results from the MICROCOL Study
- PMID: 35008376
- PMCID: PMC8750515
- DOI: 10.3390/cancers14010212
Lymph Node Involvement in Early-Stage Cervical Cancer: Is Lymphangiogenesis a Risk Factor? Results from the MICROCOL Study
Abstract
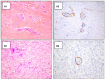
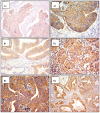
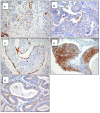
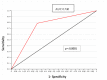
Background: In patients with cervical cancer, the presence of tumoral lymph-vascular space invasion (LVSI) is the main risk factor for pelvic lymph node metastasis (PLNM). The objective of this study was to evaluate the presence of several markers of lymphangiogenesis in early-stage cervical cancer and their correlation with PLNM and tumoral recurrence. Materials and Methods: Seventy-five patients with early-stage cervical carcinoma underwent sentinel lymph node (SLN) sampling in association with complete pelvic lymph node dissection. Primary tumors were stained with the following markers: Ki67, D2-40, CD31 and VEGF-C. A 3-year follow-up was performed to evaluate the disease-free survival. Results: Overall, 14 patients (18.6%) had PLNM. Positive LVSI was seen in 29 patients (38.6%). There was a significant correlation between LVSI evidenced by H/E staining and PLNM (p < 0.001). There was no correlation between high Ki67, CD31, D2-40, and VEGF-C staining with PLNM or tumor recurrence. Conclusions: Our data support that lymphatic spread does not require the proliferation of new lymphatic endothelial cells in early-stage cervical cancer. These results emphasize the importance of pre-existing peritumoral lymphatic vessels in the metastatic process in early cervical cancer. None of the markers of lymphangiogenesis and proliferation assessed in this study were predictive of PLNM or recurrence.
Keywords: angiogenesis; cervical cancer; lymph nodal metastasis; lymph-vascular space invasion; lymphangiogenesis.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures

Similar articles
-
Semaphorin 4D expression is associated with a poor clinical outcome in cervical cancer patients.Microvasc Res. 2014 May;93:1-8. doi: 10.1016/j.mvr.2014.02.007. Epub 2014 Mar 3. Microvasc Res. 2014. PMID: 24603190
-
Peritumoral lymphangiogenesis induced by vascular endothelial growth factor C and D promotes lymph node metastasis in breast cancer patients.World J Surg Oncol. 2012 Aug 20;10:165. doi: 10.1186/1477-7819-10-165. World J Surg Oncol. 2012. PMID: 22906075 Free PMC article.
-
Expression pattern of the lymphatic and vascular markers VEGFR-3 and CD31 does not predict regional lymph node metastasis in cutaneous melanoma.Arch Dermatol Res. 2006 Feb;297(8):352-7. doi: 10.1007/s00403-005-0633-1. Epub 2006 Jan 3. Arch Dermatol Res. 2006. PMID: 16395613
-
Conization and lymph node evaluation in low-risk cervical cancer. Is it time to avoid radical surgery? Retrospective series and literature review.Eur J Obstet Gynecol Reprod Biol. 2021 Nov;266:163-168. doi: 10.1016/j.ejogrb.2021.09.017. Epub 2021 Sep 17. Eur J Obstet Gynecol Reprod Biol. 2021. PMID: 34673464 Review.
-
[Metastatic mechanisms of uterine malignancies and therapeutic consequences].Pathologe. 2016 Nov;37(6):549-556. doi: 10.1007/s00292-016-0243-z. Pathologe. 2016. PMID: 27757531 Review. German.
Cited by
-
Inhibiting SNX10 induces autophagy to suppress invasion and EMT and inhibits the PI3K/AKT pathway in cervical cancer.Clin Transl Oncol. 2025 May;27(5):2084-2094. doi: 10.1007/s12094-024-03715-x. Epub 2024 Oct 5. Clin Transl Oncol. 2025. PMID: 39367898
-
Multiparametric mri-based radiomics nomogram for predicting lymph-vascular space invasion in cervical cancer.BMC Med Imaging. 2024 Jul 5;24(1):167. doi: 10.1186/s12880-024-01344-y. BMC Med Imaging. 2024. PMID: 38969972 Free PMC article.
-
Contrast-enhanced echocardiographic diagnosis of benign and malignant cardiac tumors and its correlation with pathology.Front Cardiovasc Med. 2023 Jun 8;10:1182334. doi: 10.3389/fcvm.2023.1182334. eCollection 2023. Front Cardiovasc Med. 2023. PMID: 37363101 Free PMC article.
-
Current Status of Lymphangiogenesis: Molecular Mechanism, Immune Tolerance, and Application Prospect.Cancers (Basel). 2023 Feb 11;15(4):1169. doi: 10.3390/cancers15041169. Cancers (Basel). 2023. PMID: 36831512 Free PMC article. Review.
-
Development and validation of a nomogram for predicting pelvic lymph node metastasis and prognosis in patients with cervical cancer.Front Oncol. 2022 Sep 2;12:952347. doi: 10.3389/fonc.2022.952347. eCollection 2022. Front Oncol. 2022. PMID: 36119526 Free PMC article.
References
-
- Sedlis A., Bundy B.N., Rotman M.Z., Lentz S.S., Muderspach L.I., Zaino R.J. A randomized trial of pelvic radiation therapy versus no further therapy in selected patients with stage IB carcinoma of the cervix after radical hysterectomy and pelvic lymphadenectomy: A Gynecologic Oncology Group Study. Gynecol. Oncol. 1999;73:177–183. doi: 10.1006/gyno.1999.5387. - DOI - PubMed
-
- Delgado G., Bundy B., Zaino R., Sevin B.U., Creasman W.T., Major F. Prospective surgical-pathological study of disease-free interval in patients with stage IB squamous cell carcinoma of the cervix: A Gynecologic Oncology Group study. Gynecol. Oncol. 1990;38:352–357. doi: 10.1016/0090-8258(90)90072-S. - DOI - PubMed
-
- Monk B.J., Wang J., Im S., Stock R.J., Peters W.A., III, Liu P.Y., Barrett R.J., II, Berek J.S., Souhami L., Grigsby P.W., et al. Rethinking the use of radiation and chemotherapy after radical hysterectomy: A clinical-pathologic analysis of a Gynecologic Oncology Group/Southwest Oncology Group/Radiation Therapy Oncology Group trial. Gynecol. Oncol. 2005;96:721–728. doi: 10.1016/j.ygyno.2004.11.007. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

