Recent Advances in Anticoagulant Treatment of Immune Thrombosis: A Focus on Direct Oral Anticoagulants in Heparin-Induced Thrombocytopenia and Anti-Phospholipid Syndrome
- PMID: 35008518
- PMCID: PMC8744910
- DOI: 10.3390/ijms23010093
Recent Advances in Anticoagulant Treatment of Immune Thrombosis: A Focus on Direct Oral Anticoagulants in Heparin-Induced Thrombocytopenia and Anti-Phospholipid Syndrome
Abstract
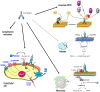
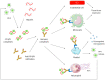
For more than 10 years, direct oral anticoagulants (DOACs) have been increasingly prescribed for the prevention and treatment of thrombotic events. However, their use in immunothrombotic disorders, namely heparin-induced thrombocytopenia (HIT) and antiphospholipid syndrome (APS), is still under investigation. The prothrombotic state resulting from the autoimmune mechanism, multicellular activation, and platelet count decrease, constitutes similarities between HIT and APS. Moreover, they both share the complexity of the biological diagnosis. Current treatment of HIT firstly relies on parenteral non-heparin therapies, but DOACs have been included in American and French guidelines for a few years, providing the advantage of limiting the need for treatment monitoring. In APS, vitamin K antagonists are conversely the main treatment (+/- anti-platelet agents), and the use of DOACs is either subject to precautionary recommendations or is not recommended in severe APS. While some randomized controlled trials have been conducted regarding the use of DOACs in APS, only retrospective studies have examined HIT. In addition, vaccine-induced immune thrombotic thrombocytopenia (VITT) is now a part of immunothrombotic disorders, and guidelines have been created concerning an anticoagulant strategy in this case. This literature review aims to summarize available data on HIT, APS, and VITT treatments and define the use of DOACs in therapeutic strategies.
Keywords: antiphospholipid syndrome; direct oral anticoagulants; heparin-induced thrombocytopenia; immune thrombosis; vaccine-induced immune thrombotic thrombocytopenia.
Conflict of interest statement
L.D. has received speaker fees from Werfen and has served on advisory board for Stago. N.G. reports personal fees and non-financial support from Boehringer Ingelheim, personal fees and non-financial support from Bayer, personal fees from Bristol-Myers Squibb/Pfizer, personal fees from LEO-Pharma, personal fees from Aspen, personal fees from SANOFI, outside the submitted work. The other authors declare no conflict of interest.
Figures
Similar articles
-
Recurrent Thrombosis With Direct Oral Anticoagulants in Antiphospholipid Syndrome: A Systematic Literature Review and Meta-analysis.Clin Ther. 2019 Sep;41(9):1839-1862. doi: 10.1016/j.clinthera.2019.06.015. Epub 2019 Aug 10. Clin Ther. 2019. PMID: 31405527
-
Anticoagulating patients with high-risk acquired thrombophilias.Blood. 2018 Nov 22;132(21):2219-2229. doi: 10.1182/blood-2018-05-848697. Blood. 2018. PMID: 30463994 Review.
-
Monitoring of anticoagulation in thrombotic antiphospholipid syndrome.J Thromb Haemost. 2021 Apr;19(4):892-908. doi: 10.1111/jth.15217. Epub 2021 Feb 20. J Thromb Haemost. 2021. PMID: 33325604 Review.
-
Direct oral anticoagulants in antiphospholipid syndrome: Meta-analysis of randomized controlled trials.Autoimmun Rev. 2021 Jan;20(1):102711. doi: 10.1016/j.autrev.2020.102711. Epub 2020 Nov 13. Autoimmun Rev. 2021. PMID: 33197580
-
Potential Role of Direct Oral Anticoagulants in the Management of Heparin-induced Thrombocytopenia.Pharmacotherapy. 2019 Aug;39(8):837-853. doi: 10.1002/phar.2298. Epub 2019 Jul 18. Pharmacotherapy. 2019. PMID: 31233222 Review.
Cited by
-
Anticoagulant therapy in renal insufficiency theme: Anticoagulation in complex situations.Thromb Res. 2024 Sep;241:109097. doi: 10.1016/j.thromres.2024.109097. Epub 2024 Jul 23. Thromb Res. 2024. PMID: 39094333 Review.
-
The Inflammatory Link of Rheumatoid Arthritis and Thrombosis: Pathogenic Molecular Circuits and Treatment Approaches.Curr Issues Mol Biol. 2025 Apr 18;47(4):291. doi: 10.3390/cimb47040291. Curr Issues Mol Biol. 2025. PMID: 40699690 Free PMC article. Review.
-
A Review of the Past, Present and Future of Cancer-associated Thrombosis Management.Heart Int. 2022 Aug 23;16(2):117-123. doi: 10.17925/HI.2022.16.2.117. eCollection 2022. Heart Int. 2022. PMID: 36721704 Free PMC article. Review.
-
Complex management of pulmonary embolism in APLA syndrome: a case study of ECMO and bivalirudin utilization.Indian J Thorac Cardiovasc Surg. 2024 Mar;40(2):254-258. doi: 10.1007/s12055-023-01667-5. Epub 2023 Dec 19. Indian J Thorac Cardiovasc Surg. 2024. PMID: 38389757 Free PMC article.
References
-
- Miyakis S., Lockshin M.D., Atsumi T., Branch D.W., Brey R.L., Cervera R., Derkesen R.H.W.M., De Groot P.G., Koike T., Meroni P.L., et al. International consensus statement on an update of the classification criteria for definite antiphospholipid syndrome (APS) J. Thromb. Haemost. 2006;4:295–306. doi: 10.1111/j.1538-7836.2006.01753.x. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

