Emergency department use for mental and substance use disorders: descriptive analysis of population-based, linked administrative data in British Columbia, Canada
- PMID: 35027424
- PMCID: PMC8762129
- DOI: 10.1136/bmjopen-2021-057072
Emergency department use for mental and substance use disorders: descriptive analysis of population-based, linked administrative data in British Columbia, Canada
Abstract
Objectives: Information on emergency department (ED) visits for mental and substance use disorders (MSUDs) is important for planning services but has not been explored in British Columbia (BC), Canada. We describe all MSUD ED visits for people ages 15 and older in the province of BC in 2017/2018 and document trends in MSUD ED visits between 2007/2008 and 2017/2018 by disorder group.
Design: Population-based linked administrative data comprised of ED records and physician billings capturing all MSUD ED visits in BC.
Setting: BC is Canada's westernmost province with a population of approximately 5 million. Permanent residents receive first-dollar coverage for all medically necessary services provided by licensed physicians or in hospitals, including ED services.
Population: All people age >15 with MSUD ED visits during the study period.
Measures: All claims with a service location in the ED or corresponding to fee items billed only in the ED were examined alongside ED visits reported through a national reporting system. Patient characteristics (sex/gender, age, location of residence, income, treated disorders and comorbidities) and previous outpatient service use for all ED visits by visit diagnosis are also described.
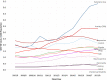
Results: A total of 72 363 people made 134 063 visits to the ED in 2017/2018 for needs related to MSUD. MSUD ED visits have increased since 2010, particularly visits for substance use and anxiety disorders. People with more frequent visits were more likely to be male, on public prescription drug plans for income assistance, prescribed psychiatric medications, and living in lower-income neighbourhoods. They used more community-based primary care and psychiatry services and had lower continuity of primary care.
Conclusions: MSUD ED visits are substantial and growing in BC. Findings underscore a need to strengthen and target community healthcare services and adequately resource and support EDs to manage growing patient populations.
Keywords: accident & emergency medicine; mental health; substance misuse.
© Author(s) (or their employer(s)) 2022. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: The authors have no relevant financial or non-financial interests to disclose. Dr. M Ruth Lavergne receives salary support from a Tier II Canada Research Chair in Primary Care and Dr. Joseph Puyat receives salary support from a Michael Smith Foundation for Health Research Scholar Award.
Figures
Similar articles
-
The relationship between outpatient service use and emergency department visits among people treated for mental and substance use disorders: analysis of population-based administrative data in British Columbia, Canada.BMC Health Serv Res. 2022 Apr 11;22(1):477. doi: 10.1186/s12913-022-07759-z. BMC Health Serv Res. 2022. PMID: 35410219 Free PMC article.
-
Socioeconomic factors and substances involved in poisoning-related emergency department visits in British Columbia, Canada.Health Promot Chronic Dis Prev Can. 2021 Jul-Aug;41(7-8):211-221. doi: 10.24095/hpcdp.41.7/8.02. Health Promot Chronic Dis Prev Can. 2021. PMID: 34427419 Free PMC article.
-
Characterizing people with frequent emergency department visits and substance use: a retrospective cohort study of linked administrative data in Ontario, Alberta, and B.C., Canada.BMC Emerg Med. 2022 Jul 14;22(1):127. doi: 10.1186/s12873-022-00673-x. BMC Emerg Med. 2022. PMID: 35836121 Free PMC article.
-
Costs of Emergency Department Visits for Mental and Substance Use Disorders in the United States, 2017.2020 May 12. In: Healthcare Cost and Utilization Project (HCUP) Statistical Briefs [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2006 Feb–. Statistical Brief #257. 2020 May 12. In: Healthcare Cost and Utilization Project (HCUP) Statistical Briefs [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2006 Feb–. Statistical Brief #257. PMID: 32550678 Free Books & Documents. Review.
-
Temporal Trends and Predictors of Thirty-Day Readmissions and Emergency Department Visits Following Total Knee Arthroplasty in Ontario Between 2003 and 2016.J Arthroplasty. 2020 Feb;35(2):364-370. doi: 10.1016/j.arth.2019.09.015. Epub 2019 Sep 14. J Arthroplasty. 2020. PMID: 31732370 Review.
Cited by
-
Experiences of individuals presenting to the emergency department for mental health reasons: A systematic mixed studies review.Aust N Z J Psychiatry. 2024 Oct;58(10):839-856. doi: 10.1177/00048674241259918. Epub 2024 Jun 16. Aust N Z J Psychiatry. 2024. PMID: 38880783 Free PMC article.
-
Improving emergency department care for adults presenting with mental illness: a systematic review of strategies and their impact on outcomes, experience, and performance.Front Psychiatry. 2024 Feb 29;15:1368129. doi: 10.3389/fpsyt.2024.1368129. eCollection 2024. Front Psychiatry. 2024. PMID: 38487586 Free PMC article. Review.
-
Regional Variation in Supply and Use of Psychiatric Services in 3 Canadian Provinces: Variation régionale de l'offre de services psychiatriques et de leur utilisation dans trois provinces canadiennes.Can J Psychiatry. 2025 Jun;70(6):511-523. doi: 10.1177/07067437251322404. Epub 2025 Mar 28. Can J Psychiatry. 2025. PMID: 40152051
-
Exploring the reliability and profile of frequent mental health presentations using different methods: An observational study using statewide ambulance data over a 4-year period.Aust N Z J Psychiatry. 2025 Jan;59(1):74-85. doi: 10.1177/00048674241289016. Epub 2024 Oct 26. Aust N Z J Psychiatry. 2025. PMID: 39460674 Free PMC article.
-
Trends and socioeconomic inequalities in acute mental health service use in Canada, 2004-2019: a nationally representative retrospective cohort study.BMJ Ment Health. 2025 May 2;28(1):e301600. doi: 10.1136/bmjment-2025-301600. BMJ Ment Health. 2025. PMID: 40316416 Free PMC article.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
