Clinical and Microbiological Characteristics of Culture-Positive, Influenza-Associated Pulmonary Aspergillosis: A Single-Center Study in Southern Taiwan, 2016-2019
- PMID: 35049989
- PMCID: PMC8780730
- DOI: 10.3390/jof8010049
Clinical and Microbiological Characteristics of Culture-Positive, Influenza-Associated Pulmonary Aspergillosis: A Single-Center Study in Southern Taiwan, 2016-2019
Abstract
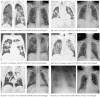
This study delineated the characteristics of 24 (11.2%) culture-positive, influenza-associated pulmonary aspergillosis (IAPA) patients out of 215 patients with severe influenza during 2016-2019 in a medical center in southern Taiwan. Twenty (83.3%) patients did not have EORTC/MSG-defined host factors. The mean time from influenza diagnosis to Aspergillus growth was 4.4 days, and 20 (83.3%) developed IAPA within seven days after influenza diagnosis. All patients were treated in intensive care units and all but one (95.8%) received mechanical ventilation. Aspergillus tracheobronchitis was evident in 6 (31.6%) of 19 patients undergoing bronchoscopy. Positive galactomannan testing of either serum or bronchoalveolar lavage was noted in all patients. On computed tomography imaging, IAPA was characterized by peribronchial infiltrates, multiple nodules, and cavities superimposed on ground-glass opacities. Pure Aspergillus growth without bacterial co-isolation in culture was found in 17 (70.8%) patients. A. fumigatus (15, 62.5%), A. flavus (6, 25.0%), and A. terreus (4, 16.7%) were the major causative species. Three patients had mixed Aspergillus infections due to two species, and two had mixed azole-susceptible and azole-resistant A. fumigatus infection. All patients received voriconazole with an all-cause mortality of 41.6%. Of 14 survivors, the mean duration of antifungal use was 40.5 days. In conclusion, IAPA is an early and rapidly deteriorating complication following influenza that necessitates clinical vigilance and prompt diagnostic workup.
Keywords: Aspergillus flavus; Aspergillus fumigatus; Aspergillus terreus; Taiwan; aspergillosis; azole resistance; bronchoscopy; galactomannan; influenza; radiology; tracheobronchitis.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- Schauwvlieghe A., Rijnders B.J.A., Philips N., Verwijs R., Vanderbeke L., Van Tienen C., Lagrou K., Verweij P.E., Van de Veerdonk F.L., Gommers D., et al. Invasive aspergillosis in patients admitted to the intensive care unit with severe influenza: A retrospective cohort study. Lancet Respir. Med. 2018;6:782–792. doi: 10.1016/S2213-2600(18)30274-1. - DOI - PubMed
-
- Van de Veerdonk F.L., Kolwijck E., Lestrade P.P., Hodiamont C.J., Rijnders B.J., van Paassen J., Haas P.J., Oliveira Dos Santos C., Kampinga G.A., Bergmans D.C., et al. Influenza-associated aspergillosis in critically ill patients. Am. J. Respir. Crit. Care Med. 2017;196:524–527. doi: 10.1164/rccm.201612-2540LE. - DOI - PubMed
-
- Wauters J., Baar I., Meersseman P., Meersseman W., Dams K., De Paep R., Lagrou K., Wilmer A., Jorens P., Hermans G. Invasive pulmonary aspergillosis is a frequent complication of critically ill H1N1 patients: A retrospective study. Intensive Care Med. 2012;38:1761–1768. doi: 10.1007/s00134-012-2673-2. - DOI - PMC - PubMed
-
- Donnelly J.P., Chen S.C., Kauffman C.A., Steinbach W.J., Baddley J.W., Verweij P.E., Clancy C.J., Wingard J.R., Lockhart S.R., Groll A.H., et al. Revision and update of the consensus definitions of invasive fungal disease from the European Organization for Research and Treatment of Cancer and the Mycoses Study Group Education and Research Consortium. Clin. Infect. Dis. 2020;71:1367–1376. doi: 10.1093/cid/ciz1008. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

