Non-PCOS Hyperandrogenic Disorders in Adolescents
- PMID: 35052005
- PMCID: PMC11875083
- DOI: 10.1055/s-0041-1742259
Non-PCOS Hyperandrogenic Disorders in Adolescents
Abstract
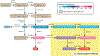
Hyperandrogenism-clinical features resulting from increased androgen production and/or action-is not uncommon in peripubertal girls. Hyperandrogenism affects 3 to 20% of adolescent girls and often is associated with hyperandrogenemia. In prepubertal girls, the most common etiologies of androgen excess are premature adrenarche (60%) and congenital adrenal hyperplasia (CAH; 4%). In pubertal girls, polycystic ovary syndrome (PCOS; 20-40%) and CAH (14%) are the most common diagnoses related to androgen excess. Androgen-secreting ovarian or adrenal tumors are rare (0.2%). Early pubic hair, acne, and/or hirsutism are the most common clinical manifestations, but signs of overt virilization in adolescent girls-rapid progression of pubic hair or hirsutism, clitoromegaly, voice deepening, severe cystic acne, growth acceleration, increased muscle mass, and bone age advancement past height age-should prompt detailed evaluation. This article addresses the clinical manifestations of and management considerations for non-PCOS-related hyperandrogenism in adolescent girls. We propose an algorithm to aid diagnostic evaluation of androgen excess in this specific patient population.
Thieme. All rights reserved.
Conflict of interest statement
Christopher R. McCartney reports all support for the present manuscript (e.g., funding, provision of study materials, medical writing, and article processing charges) from NIH/NICHD for NIH R01 HD102060 (co-PI), “Role of Androgens in the Neuroendocrine Dysfunction of Nascent PCOS”; funds paid to institution, and grants or contracts from Waterloo Foundation research grant (coinvestigator), “Does Treatment of Androgen Excess Using Spironolactone Improve Ovulatory Rates in Girls with Androgen Excess?”; funds paid to institution, leadership or fiduciary role in other board, society, committee or advocacy group, paid or unpaid from Endocrine Society (editorial board,
Figures
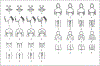

Similar articles
-
AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS, AMERICAN COLLEGE OF ENDOCRINOLOGY, AND ANDROGEN EXCESS AND PCOS SOCIETY DISEASE STATE CLINICAL REVIEW: GUIDE TO THE BEST PRACTICES IN THE EVALUATION AND TREATMENT OF POLYCYSTIC OVARY SYNDROME--PART 1.Endocr Pract. 2015 Nov;21(11):1291-300. doi: 10.4158/EP15748.DSC. Endocr Pract. 2015. PMID: 26509855
-
[Evaluation and treatment of adolescent girls with hirsutism].Ginekol Pol. 2009 May;80(5):374-8. Ginekol Pol. 2009. PMID: 19548458 Review. Polish.
-
Extensive clinical experience: relative prevalence of different androgen excess disorders in 950 women referred because of clinical hyperandrogenism.J Clin Endocrinol Metab. 2006 Jan;91(1):2-6. doi: 10.1210/jc.2005-1457. Epub 2005 Nov 1. J Clin Endocrinol Metab. 2006. PMID: 16263820
-
The clinical evaluation of hirsutism.Dermatol Ther. 2008 Sep-Oct;21(5):376-91. doi: 10.1111/j.1529-8019.2008.00219.x. Dermatol Ther. 2008. PMID: 18844715 Review.
-
Non polycystic ovary syndrome-related endocrine disorders associated with hirsutism.Eur J Clin Invest. 2012 Jan;42(1):86-94. doi: 10.1111/j.1365-2362.2011.02550.x. Epub 2011 May 30. Eur J Clin Invest. 2012. PMID: 21623779 Review.
Cited by
-
Criteria for Diagnosis of Polycystic Ovary Syndrome during Adolescence: Literature Review.Diagnostics (Basel). 2022 Aug 10;12(8):1931. doi: 10.3390/diagnostics12081931. Diagnostics (Basel). 2022. PMID: 36010282 Free PMC article. Review.
-
Application value of tumor necrosis factor inhibitors in in vitro fertilization-embryo transfer in infertile women with polycystic ovary syndrome.BMC Pregnancy Childbirth. 2023 Apr 13;23(1):247. doi: 10.1186/s12884-023-05546-0. BMC Pregnancy Childbirth. 2023. PMID: 37055769 Free PMC article.
-
The Influences of Perinatal Androgenic Exposure on Cardiovascular and Metabolic Disease of Offspring of PCOS.Reprod Sci. 2023 Nov;30(11):3179-3189. doi: 10.1007/s43032-023-01286-w. Epub 2023 Jun 28. Reprod Sci. 2023. PMID: 37380913 Review.
-
Impact of dehydroepiandrosterone sulfate and free androgen index on pregnancy and neonatal outcomes in PCOS patients.Reprod Biol Endocrinol. 2024 Apr 16;22(1):43. doi: 10.1186/s12958-024-01212-y. Reprod Biol Endocrinol. 2024. PMID: 38627777 Free PMC article.
-
A New Heterozygous Variant of c.1225_1227delTTC (p.Phe409del) in Insulin Receptor Gene Associated with Severe Insulin Resistance and Hyperandrogenemia in an Adolescent Female with Type A Severe Insulin Resistance Syndrome.Diabetes Metab Syndr Obes. 2024 Nov 25;17:4389-4396. doi: 10.2147/DMSO.S481745. eCollection 2024. Diabetes Metab Syndr Obes. 2024. PMID: 39619220 Free PMC article.
References
-
- Hickey M, Doherty DA, Atkinson H, et al. Clinical, ultrasound and biochemical features of polycystic ovary syndrome in adolescents: implications for diagnosis. Hum Reprod. 2011;26(6):1469–1477. - PubMed
-
- Gambineri A, Fanelli F, Prontera O, et al. Prevalence of hyperandrogenic states in late adolescent and young women: epidemiological survey on italian high-school students. J Clin Endocrinol Metab. 2013;98(4):1641–1650. - PubMed
-
- Dubey P, Reddy SY, Alvarado L, Manuel SL, Dwivedi AK. Prevalence of at-risk hyperandrogenism by age and race/ethnicity among females in the United States using NHANES III. Eur J Obstet Gynecol Reprod Biol. 2021;260:189–197. - PubMed
-
- van Hooff MH, Voorhorst FJ, Kaptein MB, Hirasing RA, Koppenaal C, Schoemaker J. Endocrine features of polycystic ovary syndrome in a random population sample of 14–16 year old adolescents. Hum Reprod. 1999;14(9):2223–2229. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

