Predialysis serum lactate levels could predict dialysis withdrawal in Type 1 cardiorenal syndrome patients
- PMID: 35059613
- PMCID: PMC8760464
- DOI: 10.1016/j.eclinm.2021.101232
Predialysis serum lactate levels could predict dialysis withdrawal in Type 1 cardiorenal syndrome patients
Abstract
Background: Renal replacement therapy (RRT) is an effective rescue therapy for Type 1 cardiorenal syndrome (CRS). Previous studies have demonstrated that type 1 CRS patients with severe renal dysfunction were susceptible to sepsis, and that serum lactate has been correlated with the risk of mortality in patients with sepsis. However, the association between serum lactate level and the prognosis of type 1 CRS patients requiring RRT is unknown.
Methods: An inception cohort of 500 type 1 CRS patients who received RRT in a tertiary-care referral hospital in Taiwan from August 2011 to January 2018 were enrolled. The outcomes of interest were dialysis withdrawal and 90-day mortality. The results were further externally validated using sampling data of type 1 CRS patients requiring dialysis from multiple tertiary-care centers.
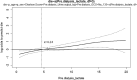
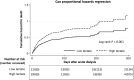
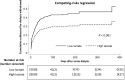
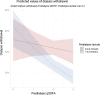
Findings: The 90-day mortality rate was 52.8% and the incidence rate of dialysis withdrawal was 34.8%. Lower pre-dialysis lactate was correlated with a higher rate of dialysis withdrawal and lower rate of mortality. Generalized additive model showed that 4.2 mmol/L was an adequate cut-off value of lactate to predict mortality. Taking mortality as a competing risk, Fine-Gray subdistribution hazard analysis further indicated that a low lactate level (≦ 4.2 mmol/L) was an independent predictor for the possibility of dialysis withdrawal, as also shown in external validation. The interaction of quick Sequential Organ Failure Assessment score and lactate was associated with dialysis dependence in a disease severity-dependent manner. Furthermore, the associations between hyperlactatemia and dialysis dependence were consistent in the patients with and without sepsis.
Interpretation: Serum lactate level is accurate and capable of forecasting the prognosis along with qSOFA severity for clinical decision-making for treating type 1 CRS patients. Further studies are needed to validate our results.
Funding: This study was supported by grants from Taiwan National Science Council [104-2314-B-002-125-MY3,106-2314-B-002-166-MY3,107-2314-B-002-026-MY3], National Taiwan University Hospital [106-FTN20,106-P02,UN106-014,106-S3582,107-S3809,107-T02,PC1246,VN109-09,109-S4634,UN109-041], Ministry of Science and Technology of the Republic of China [MOST106-2321-B-182-002,106-2314-B-182A-064,MOST107-2321-B-182-004,MOST107-2314-B-182A-138, MOST108-2321-B-182-003,MOST109-2321-B-182-001, MOST108-2314-B-182A-027], Chang Gung Memorial Hospital [CMRPG-2G0361,CMRPG-2H0161,CMRPG-2J0261, CMRPG-2K0091], and Ministry of Health and Welfare of the Republic of China [PMRPG-2L0011].
Keywords: Prognosis; Type 1 cardiorenal syndrome; renal replacement therapy; serum lactate; withdrawal.
© 2021 Published by Elsevier Ltd.
Conflict of interest statement
HCP, TMH, CYS, NKC, CHT, FYY, TSL, YMC, and VCW reported grants from Taiwan National Science Council, National Health Research Institutes, National Taiwan University Hospital, and Ministry of Science and Technology (MOST) of the Republic of China (Taiwan). No other disclosures were reported.
Figures
Similar articles
-
Outcomes associated with acute kidney disease: A systematic review and meta-analysis.EClinicalMedicine. 2022 Dec 13;55:101760. doi: 10.1016/j.eclinm.2022.101760. eCollection 2023 Jan. EClinicalMedicine. 2022. PMID: 36531983 Free PMC article.
-
Difference between elderly and non-elderly patients in using serum lactate level to predict mortality caused by sepsis in the emergency department.Medicine (Baltimore). 2018 Mar;97(13):e0209. doi: 10.1097/MD.0000000000010209. Medicine (Baltimore). 2018. PMID: 29595662 Free PMC article.
-
Diabetes prevalence and outcomes in hospitalized cardiorenal-syndrome patients with and without hyponatremia.BMC Nephrol. 2020 Sep 10;21(1):393. doi: 10.1186/s12882-020-02032-z. BMC Nephrol. 2020. PMID: 32912147 Free PMC article.
-
Acute Kidney Injury in Cardiorenal Syndrome Type 1 Patients: A Systematic Review and Meta-Analysis.Cardiorenal Med. 2016 Feb;6(2):116-28. doi: 10.1159/000442300. Epub 2015 Dec 19. Cardiorenal Med. 2016. PMID: 26989397 Free PMC article. Review.
-
Accelerated versus standard initiation of renal replacement therapy for critically ill patients with acute kidney injury: a systematic review and meta-analysis of RCT studies.Crit Care. 2021 Jan 5;25(1):5. doi: 10.1186/s13054-020-03434-z. Crit Care. 2021. PMID: 33402204 Free PMC article.
Cited by
-
Visceral adiposity as a predictor of new-onset diabetes in patients with primary aldosteronism: a cohort study.Ther Adv Chronic Dis. 2024 Nov 30;15:20406223241301892. doi: 10.1177/20406223241301892. eCollection 2024. Ther Adv Chronic Dis. 2024. PMID: 39619168 Free PMC article.
-
Circulating Fibroblast Growth Factor-23 Levels Can Predict Rapid Kidney Function Decline in a Healthy Population: A Community-Based Study.Biomolecules. 2022 Dec 24;13(1):31. doi: 10.3390/biom13010031. Biomolecules. 2022. PMID: 36671416 Free PMC article.
-
Unsupervised clustering identifies sub-phenotypes and reveals novel outcome predictors in patients with dialysis-requiring sepsis-associated acute kidney injury.Ann Med. 2023 Dec;55(1):2197290. doi: 10.1080/07853890.2023.2197290. Ann Med. 2023. PMID: 37043222 Free PMC article.
-
Serum Cystatin C Levels Could Predict Rapid Kidney Function Decline in A Community-Based Population.Biomedicines. 2022 Nov 2;10(11):2789. doi: 10.3390/biomedicines10112789. Biomedicines. 2022. PMID: 36359307 Free PMC article.
-
GLP-1 receptor agonists' impact on cardio-renal outcomes and mortality in T2D with acute kidney disease.Nat Commun. 2024 Jul 13;15(1):5912. doi: 10.1038/s41467-024-50199-y. Nat Commun. 2024. PMID: 39003287 Free PMC article.
References
-
- Ronco C., Cicoira M., McCullough P.A. Cardiorenal syndrome type 1: pathophysiological crosstalk leading to combined heart and kidney dysfunction in the setting of acutely decompensated heart failure. J Am Coll Cardiol. 2012;60(12):1031–1042. - PubMed
-
- Shirakabe A., Hata N., Kobayashi N., Shinada T., Tomita K., Tsurumi M., et al. Long-term prognostic impact after acute kidney injury in patients with acute heart failure. Int Heart J. 2012;53(5):313–319. - PubMed
LinkOut - more resources
Full Text Sources

