Incidence, Clinical Characteristics, Risk Factors and Outcomes of Acute Coronary Syndrome in Patients With COVID-19: Results of the UMC-19-S1010
- PMID: 35065863
- PMCID: PMC8563352
- DOI: 10.1016/j.jemermed.2021.10.046
Incidence, Clinical Characteristics, Risk Factors and Outcomes of Acute Coronary Syndrome in Patients With COVID-19: Results of the UMC-19-S1010
Abstract
Background: There is a lack of knowledge about the real incidence of acute coronary syndrome (ACS) in patients with COVID-19, their clinical characteristics, and their prognoses.
Objective: We investigated the incidence, clinical characteristics, risk factors, and outcomes of ACS in patients with COVID-19 in the emergency department.
Methods: We retrospectively reviewed all COVID-19 patients diagnosed with ACS in 62 Spanish emergency departments between March and April 2020 (the first wave of COVID-19). We formed 2 control groups: COVID-19 patients without ACS (control A) and non-COVID-19 patients with ACS (control B). Unadjusted comparisons between cases and control subjects were performed regarding 58 characteristics and outcomes.
Results: We identified 110 patients with ACS in 74,814 patients with COVID-19 attending the ED (1.48% [95% confidence interval {CI} 1.21-1.78%]). This incidence was lower than that observed in non-COVID-19 patients (3.64% [95% CI 3.54-3.74%]; odds ratio [OR] 0.40 [95% CI 0.33-0.49]). The clinical characteristics of patients with COVID-19 associated with a higher risk of presenting ACS were: previous coronary artery disease, age ≥60 years, hypertension, chest pain, raised troponin, and hypoxemia. The need for hospitalization and admission to intensive care and in-hospital mortality were higher in cases than in control group A (adjusted OR [aOR] 6.36 [95% CI 1.84-22.1], aOR 4.63 [95% CI 1.88-11.4], and aOR 2.46 [95% CI 1.15-5.25]). When comparing cases with control group B, the aOR of admission to intensive care was 0.41 (95% CI 0.21-0.80), while the aOR for in-hospital mortality was 5.94 (95% CI 2.84-12.4).
Conclusions: The incidence of ACS in patients with COVID-19 attending the emergency department was low, around 1.48%, but could be increased in some circumstances. Patients with COVID-19 with ACS had a worse prognosis than control subjects with higher in-hospital mortality.
Keywords: COVID-19; SARS-Cov-2; acute coronary syndrome; clinical characteristics; incidence; outcome; risk factors.
Copyright © 2021 Elsevier Ltd. All rights reserved.
Figures

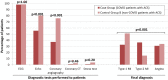

References
-
- World Health Organization. WHO coronavirus (COVID-19) dashboard. Available at: https://covid19.who.int/?gclid=EAIaIQobChMI9sDNu–k7QIVFxkGAB0V-wB5EAAYAS.... Accessed November 21, 2021.
-
- Clerkin KJ, Fried JA, Raikhelkar J, et al. COVID-19 and cardiovascular disease. Circulation. 2020;141:1648–1655. - PubMed
-
- Madjid M, Safavi-Naeini P, Solomon SD, Vardeny O. Potential effects of coronaviruses on the cardiovascular system: a review. JAMA Cardiol. 2020;5:831–840. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

