The Prognostic Capacity of the Radiographic Assessment for Lung Edema Score in Patients With COVID-19 Acute Respiratory Distress Syndrome-An International Multicenter Observational Study
- PMID: 35071263
- PMCID: PMC8766516
- DOI: 10.3389/fmed.2021.772056
The Prognostic Capacity of the Radiographic Assessment for Lung Edema Score in Patients With COVID-19 Acute Respiratory Distress Syndrome-An International Multicenter Observational Study
Abstract
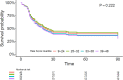
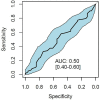
Background: The radiographic assessment for lung edema (RALE) score has an association with mortality in patients with acute respiratory distress syndrome (ARDS). It is uncertain whether the RALE scores at the start of invasive ventilation or changes thereof in the next days have prognostic capacities in patients with COVID-19 ARDS. Aims and Objectives: To determine the prognostic capacity of the RALE score for mortality and duration of invasive ventilation in patients with COVID-19 ARDS. Methods: An international multicenter observational study included consecutive patients from 6 ICUs. Trained observers scored the first available chest X-ray (CXR) obtained within 48 h after the start of invasive ventilation ("baseline CXR") and each CXRs thereafter up to day 14 ("follow-up CXR"). The primary endpoint was mortality at day 90. The secondary endpoint was the number of days free from the ventilator and alive at day 28 (VFD-28). Results: A total of 350 CXRs were scored in 139 patients with COVID-19 ARDS. The RALE score of the baseline CXR was high and was not different between survivors and non-survivors (33 [24-38] vs. 30 [25-38], P = 0.602). The RALE score of the baseline CXR had no association with mortality (hazard ratio [HR], 1.24 [95% CI 0.88-1.76]; P = 0.222; area under the receiver operating characteristic curve (AUROC) 0.50 [0.40-0.60]). A change in the RALE score over the first 14 days of invasive ventilation, however, had an independent association with mortality (HR, 1.03 [95% CI 1.01-1.05]; P < 0.001). When the event of death was considered, there was no significant association between the RALE score of the baseline CXR and the probability of being liberated from the ventilator (HR 1.02 [95% CI 0.99-1.04]; P = 0.08). Conclusion: In this cohort of patients with COVID-19 ARDS, with high RALE scores of the baseline CXR, the RALE score of the baseline CXR had no prognostic capacity, but an increase in the RALE score in the next days had an association with higher mortality.
Keywords: ARDS; RALE score; chest X-ray (CXR); corona virus (COVID-19); intensive and critical care; mechanical ventilated; prognostication; radiograph (X-ray).
Copyright © 2022 Valk, Zimatore, Mazzinari, Pierrakos, Sivakorn, Dechsanga, Grasso, Beenen, Bos, Paulus, Schultz and Pisani.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

References
LinkOut - more resources
Full Text Sources

