Contraception after in vitro fertilisation (IVF): a qualitative study of the views of women who have had spontaneous pregnancies after successful IVF
- PMID: 35135587
- PMCID: PMC8822864
- DOI: 10.1186/s12978-022-01349-2
Contraception after in vitro fertilisation (IVF): a qualitative study of the views of women who have had spontaneous pregnancies after successful IVF
Abstract
Background: The use of in vitro fertilisation (IVF) has increased rapidly since its inception in 1978. Women seeking IVF have a wide range of subfertility causes including unexplained subfertility. A growing subgroup of women seek treatment for other reasons than fertility problems, for example, women in same sex relationships and single women. This study aims to better understand the contraceptive needs of women after successful IVF pregnancy in order to improve service delivery and prevent unplanned and rapid-repeat pregnancies.
Methods: A qualitative study of views of women who have had spontaneous pregnancies after successful IVF. Participants were recruited using purposive and snowballing sampling methods from social media and peer networks. The framework method was used for analysis using NVivo12.
Results: The sample comprised 21 interviewees from the United Kingdom (UK), having a range of spontaneous pregnancy outcomes, including single and multiple livebirths, miscarriage, ectopic pregnancy and termination of pregnancy. Contraceptive choices were subject to a complex and dynamic interaction of influencing factors including beliefs regarding subfertility, desire for children and views on contraception. None of the women recalled receiving any information or useful counselling about contraception during fertility or maternity care. After IVF pregnancy, most women (n = 16) used no or ineffective contraception. Spontaneous pregnancy was not universally welcomed in this group and inter-pregnancy intervals were often short (n = 16, less than 18 months). Even after subsequent spontaneous pregnancy, use of contraception and the most effective methods remained low. Women held persistent beliefs regarding their subfertility despite subsequent spontaneous pregnancy. They associated aspects of the IVF process with a sense of personal failure, despite an ultimately "successful" outcome of livebirth. These aspects may reinforce their self-belief in subfertility. Other barriers to contraception use in women having IVF included: lack of knowledge of likelihood of spontaneous pregnancy, lack of contraceptive experience and inherent incentives towards shorter inter-pregnancy intervals.
Conclusions: The contraceptive needs of women having IVF pregnancies are real and are being overlooked. Fertility services should take responsibility for providing information on the risks of subsequent spontaneous pregnancy. Maternity and community healthcare professionals must address women's perceptions of their fertility in order to engage them in contraception counselling.
Keywords: Contraception; Fertilization in vitro; Infertility; Qualitative.
Plain language summary
Women who have difficulty getting pregnant may choose to use fertility treatment to help. Fertility treatment known as ‘in vitro fertilisation’, or IVF, was developed around 40 years ago and has been increasingly used ever since. Over 8 million babies have been born this way around the world. There are many different reasons why women can have problems getting pregnant and in a quarter of cases the cause is never found. We know that some women, who have babies using IVF, get pregnant again afterwards without fertility treatment. Getting pregnant again quickly, or when a woman isn’t ready, can be worse for the health of the mother and child. Therefore, this study aims to understand what contraception women need after IVF to plan and space their future pregnancies. We spoke to 21 women who became pregnant without fertility treatment after having their first babies using IVF. Although most of these women had not been using contraception after their first baby, they were shocked to get pregnant again as they firmly believed they could not get pregnant without fertility treatment. Most of these pregnancies had happened quickly and not all the women were happy to be pregnant again. These women were not given the information they needed about their chances of getting pregnant after IVF without fertility treatment. Fertility and maternity services must close this gap. Health professionals also need to explore women’s beliefs about their own fertility after IVF before they can start to have helpful conversations about contraception.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
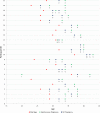

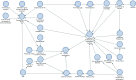
References
-
- Human Fertilisation and Embryology Authority. Fertility treatment 2018: trends and figures. 2020.
-
- More than 8 million babies born from IVF since the world's first in 1978 [press release]. ScienceDaily: European Society of Human Reproduction and EmbryologyJuly 3, 2018.
-
- Richardson A, Taylor M, Teoh J, Karasu T. Antenatal management of singleton pregnancies conceived using assisted reproductive technology. Obstet Gynaecol. 2020;22(1):34–44. doi: 10.1111/tog.12608. - DOI
-
- Fertility problems: assessment and treatment. National Institute for Health and Care Excellence; 2013 (last updated 2017). - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

