Mortality Rates Among U.S. Women of Reproductive Age, 1999-2019
- PMID: 35135719
- PMCID: PMC8940663
- DOI: 10.1016/j.amepre.2021.10.009
Mortality Rates Among U.S. Women of Reproductive Age, 1999-2019
Abstract
Introduction: High and increasing levels of pregnancy-related mortality and morbidity in the U.S. indicate that the underlying health status of reproductive-aged women may be far from optimal, yet few studies have examined mortality trends and disparities exclusively among this population.
Methods: All-cause and cause-specific mortality data for 1999-2019 were obtained from the Centers for Disease Control and Prevention WONDER Underlying Cause of Death database. Levels and trends in mortality between 1999 and 2019 for women aged 15-44 years stratified by age, race/ethnicity, and state were examined. Given the urgent need to address pregnancy-related health disparities, the correlation between all-cause and pregnancy-related mortality rates across states for the years 2015-2019 was also examined.
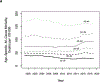
Results: Age-adjusted, all-cause mortality rates among women aged 15-44 years improved between 2003 and 2011 but worsened between 2011 and 2019. The recent increase in mortality among this age group was not driven solely by increases in external causes of death. Patterns differed by age, race/ethnicity, and geography, with non-Hispanic American Indian and Alaskan Native women having 2.3 and non-Hispanic Black women having 1.4 times the risk of all-cause mortality in 2019 compared with that of non-Hispanic White women. Age-adjusted all-cause mortality rates and pregnancy-related mortality rates were strongly correlated at the state level (r=0.75).
Conclusions: Increasing mortality among reproductive-aged women has substantial implications for maternal, women's, and children's health. Given the high correlation between pregnancy-related mortality and all-cause mortality at the state level, addressing the structural factors that shape mortality risks may have the greatest likelihood of improving women's health outcomes across the life course.
Copyright © 2021 American Journal of Preventive Medicine. Published by Elsevier Inc. All rights reserved.
Figures




References
-
- Trends in maternal mortality 2000 to 2017: estimates by WHO, UNICEF, UNFPA, World Bank Group and the United Nations Population Division. Geneva: WHO; 2019.
-
- Martin N, Cillekens E, Freitas A. Lost Mothers. ProPublica. https://www.propublica.org/article/lost-mothers-maternal-health-died-chi.... Published July 17, 2017. Accessed March 8, 2021.
-
- Declercq E, Shah N. Maternal deaths represent the canary in the coal mine for women’s health. STAT News. https://www.statnews.com/2018/08/22/maternal-deaths-women-health/. Published August 22, 2018. Accessed March 8, 2021.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

