Impact of Empirical Antibiotic Therapy on Outcomes of Outpatient Urinary Tract Infection Due to Nonsusceptible Enterobacterales
- PMID: 35138150
- PMCID: PMC8826825
- DOI: 10.1128/spectrum.02359-21
Impact of Empirical Antibiotic Therapy on Outcomes of Outpatient Urinary Tract Infection Due to Nonsusceptible Enterobacterales
Abstract
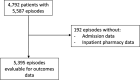
Resistance to oral antibiotics commonly used to treat outpatient urinary tract infections (UTIs) is increasing, but the implications of empirical treatment of resistant pathogens are not well described. Using an electronic records database, we reviewed the outcomes of patients >18 years of age who developed an outpatient UTI and had an outpatient urine culture result showing a member of the order Enterobacterales along with prescription data for an oral antibiotic filled on the day before, day of, or day after the culture was collected. Linear probability models were used to estimate partial effects of select clinical and demographic variables on the composite outcome. In all, 4,792 patients had 5,587 oral antibiotic prescriptions. Of 5,395 evaluable episodes, 22% of patients received an antibiotic to which the pathogen was resistant in vitro, and those patients were almost twice as likely to require a second prescription (34% versus 19%) or be hospitalized (15% versus 8%) within 28 days of the initial prescription fill compared to patients who received an antibiotic to which the pathogen was susceptible. Approximately 1% of Enterobacterales isolates were resistant to all commonly available classes of oral antibiotics. A greater risk of treatment failure was seen in patients over 60 years of age, patients with diabetes mellitus, men, and those treated with an antibiotic when prior culture identified an organism resistant to that class. The increasing resistance among members of Enterobacterales responsible for outpatient UTIs is limiting the effectiveness of empirical treatment with existing antibiotics, and consequently, outpatients with UTI are more likely to require additional courses of therapy or be hospitalized. IMPORTANCE Resistance rates for bacteria that cause urinary tract infections (UTIs) have increased dramatically. Regional rates of resistance to commonly prescribed antibiotics now exceed 20%, which is the threshold at which the Infectious Diseases Society of America recommends therapy be guided by culture. Our goals were to describe outcomes for outpatients with UTIs caused by bacteria resistant to empirically chosen antibiotics and to create a simple stratification schema for clinicians to identify UTI patients at increased risk of treatment failure due to antibiotic mismatch. These data are relevant to clinicians, given how common uncomplicated UTIs are, and highlight the need for clinicians to understand local resistance rates and the importance of culture-guided treatment, especially in vulnerable patients. These findings also showed that 1% of bacteria were resistant to all major classes of oral antibiotics, underscoring the need for new antibiotics to treat patients with UTIs due to resistant bacteria.
Keywords: Gram-negative bacteria; antimicrobial resistance; urinary tract infection.
Conflict of interest statement
The authors declare a conflict of interest. M.W.D., S.P. and S.I.A. were employed by Iterum Therapeutics. S.B., J.M. and V.G. were employed by Becton, Dickinson and Company.
References
-
- Symphony Healthcare. 2018. Ad hoc report performed for Iterum Therapeutics. Symphony Healthcare, Phoenix, AZ. Available at https://data.bloomberglp.com/professional/sites/10/Symphony-Health-In-Ac....
-
- Schappert SM, Rechtsteiner EA. 2011. Ambulatory medical care utilization estimates for 2007. National Center for Health Statistics. Vital Health Stat 13 2011:1–38. - PubMed
-
- CDC. 2019. CDC summary data. https://cdc.gov/gis/interactive-applications.htm. Accessed 20 May 2019.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical