Chronic Pancreatitis Is a Risk Factor for Pancreatic Cancer, and Incidence Increases With Duration of Disease: A Systematic Review and Meta-analysis
- PMID: 35142721
- PMCID: PMC8963838
- DOI: 10.14309/ctg.0000000000000463
Chronic Pancreatitis Is a Risk Factor for Pancreatic Cancer, and Incidence Increases With Duration of Disease: A Systematic Review and Meta-analysis
Abstract
Introduction: Observational studies have suggested an increased risk of pancreatic ductal adenocarcinoma (PDAC) in patients with acute and chronic pancreatitis. We conducted a systematic review and meta-analysis to evaluate the magnitude of this association and summarize the published epidemiological evidence.
Methods: We searched electronic databases (MEDLINE, Embase, Web of Science, Cochrane, and Scopus) and reference lists until January 18, 2021. Studies reporting quantitative association between pancreatitis and PDAC were included and assessed for eligibility, data abstraction, and risk of bias. Standardized incidence ratios (SIRs) were pooled using the random-effects model.
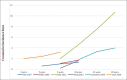
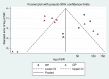
Results: Twenty-five cohort and case-control studies met inclusion criteria. Meta-analysis of 12 chronic pancreatitis (CP) studies demonstrated an increased risk of PDAC in patients with CP (SIR: 22.61, 95% confidence interval [CI]: 14.42-35.44). This elevated risk persisted in subgroup analysis of studies that excluded patients diagnosed with PDAC within 2 years of CP diagnosis (SIR: 21.77, 95% CI: 14.43-32.720). The risk was higher in hereditary pancreatitis (SIR: 63.36, 95% CI: 45.39-88.46). The cumulative incidence rates of PDAC in CP increased with follow-up duration. Limited evidence in acute pancreatitis indicates higher PDAC risk in the subset of patients eventually diagnosed with CP. PDAC seems to be uncommon in patients with autoimmune pancreatitis, with 8 reported cases in 358 patients with autoimmune pancreatitis across 4 studies.
Discussion: There is an increased risk of PDAC in patients with CP, and incidence rates increase with CP disease duration. Our results indicate that PDAC surveillance may be considered in individuals with long-standing CP.
Copyright © 2022 The Author(s). Published by Wolters Kluwer Health, Inc. on behalf of The American College of Gastroenterology.
Conflict of interest statement
Data, analytic methods, and study materials pertinent to this manuscript may be made available to other researchers on reasonable request.
Figures


Similar articles
-
Incidence and Risk of Pancreatic Cancer in Patients with a New Diagnosis of Chronic Pancreatitis.Dig Dis Sci. 2022 Feb;67(2):708-715. doi: 10.1007/s10620-021-06886-7. Epub 2021 Feb 25. Dig Dis Sci. 2022. PMID: 33630214
-
Association between chronic pancreatitis and pancreatic cancer: A 10-year retrospective study of endoscopically treated and surgical patients.Int J Cancer. 2020 Sep 1;147(5):1450-1460. doi: 10.1002/ijc.32971. Epub 2020 Apr 3. Int J Cancer. 2020. PMID: 32162688
-
Acute Pancreatitis Recurrences Augment Long-Term Pancreatic Cancer Risk.Am J Gastroenterol. 2023 Apr 1;118(4):727-737. doi: 10.14309/ajg.0000000000002081. Epub 2022 Dec 20. Am J Gastroenterol. 2023. PMID: 36473072 Free PMC article.
-
Prevalence of primary painless chronic pancreatitis: A systematic review and meta-analysis.Pancreatology. 2022 Jan;22(1):20-29. doi: 10.1016/j.pan.2021.11.006. Epub 2021 Nov 18. Pancreatology. 2022. PMID: 34840065 Free PMC article.
-
Endoscopic Ultrasound Guided Fine-Needle Aspiration for Solid Lesions in Chronic Pancreatitis: A Systematic Review and Meta-Analysis.Dig Dis Sci. 2022 Jun;67(6):2552-2561. doi: 10.1007/s10620-021-07066-3. Epub 2021 Jun 4. Dig Dis Sci. 2022. PMID: 34086166
Cited by
-
Macrophage-induced reactive oxygen species in the initiation of pancreatic cancer: a mini-review.Front Immunol. 2024 Mar 21;15:1278807. doi: 10.3389/fimmu.2024.1278807. eCollection 2024. Front Immunol. 2024. PMID: 38576613 Free PMC article. Review.
-
Multimodal Pancreatic Cancer Detection Using Methylated DNA Biomarkers in Pancreatic Juice and Plasma CA 19-9: A Prospective Multicenter Study.Clin Gastroenterol Hepatol. 2025 Apr;23(5):766-775. doi: 10.1016/j.cgh.2024.07.048. Epub 2024 Oct 28. Clin Gastroenterol Hepatol. 2025. PMID: 39477082
-
Pancreatic Cancer: A Review of Risk Factors.Life (Basel). 2024 Aug 5;14(8):980. doi: 10.3390/life14080980. Life (Basel). 2024. PMID: 39202722 Free PMC article. Review.
-
Pancreatic Cancer Resistance to Treatment: The Role of Microbiota.Biomedicines. 2023 Jan 7;11(1):157. doi: 10.3390/biomedicines11010157. Biomedicines. 2023. PMID: 36672664 Free PMC article. Review.
-
Association of Glycated Hemoglobin With a Risk of Pancreatic Cancer in High-Risk Individuals Based on Genetic and Family History.Clin Transl Gastroenterol. 2024 Jan 1;15(1):e00650. doi: 10.14309/ctg.0000000000000650. Clin Transl Gastroenterol. 2024. PMID: 37800692 Free PMC article.
References
-
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin 2020;70:7–30. - PubMed
-
- Society AC. Cancer Facts & Figures. American Cancer Society: Atlanta, GA, 2016.
-
- Huang J, Lok V, Ngai CH, et al. . Worldwide burden of, risk factors for, and trends in pancreatic cancer. Gastroenterology 2021;160:744–54. - PubMed
-
- Owens DK, Davidson KW, Krist AH, et al. . Screening for pancreatic cancer: US Preventive Services Task Force reaffirmation recommendation statement. JAMA 2019;322:438–44. - PubMed
-
- Majumder S, Chari ST. Chronic pancreatitis. Lancet 2016;387:1957–66. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

