Analysis of separate training and validation radical prostatectomy cohorts identifies 0.25 mm diameter as an optimal definition for "large" cribriform prostatic adenocarcinoma
- PMID: 35145197
- PMCID: PMC9314256
- DOI: 10.1038/s41379-022-01009-7
Analysis of separate training and validation radical prostatectomy cohorts identifies 0.25 mm diameter as an optimal definition for "large" cribriform prostatic adenocarcinoma
Abstract
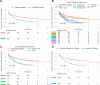
Cribriform growth pattern is well-established as an adverse pathologic feature in prostate cancer. The literature suggests "large" cribriform glands associate with aggressive behavior; however, published studies use varying definitions for "large". We aimed to identify an outcome-based quantitative cut-off for "large" vs "small" cribriform glands. We conducted an initial training phase using the tissue microarray based Canary retrospective radical prostatectomy cohort. Of 1287 patients analyzed, cribriform growth was observed in 307 (24%). Using Kaplan-Meier estimates of recurrence-free survival curves (RFS) that were stratified by cribriform gland size, we identified 0.25 mm as the optimal cutoff to identify more aggressive disease. In univariable and multivariable Cox proportional hazard analyses, size >0.25 mm was a significant predictor of worse RFS compared to patients with cribriform glands ≤0.25 mm, independent of pre-operative PSA, grade, stage and margin status (p < 0.001). In addition, two different subset analyses of low-intermediate risk cases (cases with Gleason score ≤ 3 + 4 = 7; and cases with Gleason score = 3 + 4 = 7/4 + 3 = 7) likewise demonstrated patients with largest cribriform diameter >0.25 mm had a significantly lower RFS relative to patients with cribriform glands ≤0.25 mm (each subset p = 0.004). Furthermore, there was no significant difference in outcomes between patients with cribriform glands ≤ 0.25 mm and patients without cribriform glands. The >0.25 mm cut-off was validated as statistically significant in a separate 419 patient, completely embedded whole-section radical prostatectomy cohort by biochemical recurrence, metastasis-free survival, and disease specific death, even when cases with admixed Gleason pattern 5 carcinoma were excluded. In summary, our findings support reporting cribriform gland size and identify 0.25 mm as an optimal outcome-based quantitative measure for defining "large" cribriform glands. Moreover, cribriform glands >0.25 mm are associated with potential for metastatic disease independent of Gleason pattern 5 adenocarcinoma.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures



Similar articles
-
Proposal for an optimised definition of adverse pathology (unfavourable histology) that predicts metastatic risk in prostatic adenocarcinoma independent of grade group and pathological stage.Histopathology. 2024 Oct;85(4):598-613. doi: 10.1111/his.15231. Epub 2024 Jun 3. Histopathology. 2024. PMID: 38828674
-
Large cribriform growth pattern identifies ISUP grade 2 prostate cancer at high risk for recurrence and metastasis.Mod Pathol. 2019 Jan;32(1):139-146. doi: 10.1038/s41379-018-0157-9. Epub 2018 Oct 22. Mod Pathol. 2019. PMID: 30349027 Free PMC article.
-
Histologic Grading of Prostatic Adenocarcinoma Can Be Further Optimized: Analysis of the Relative Prognostic Strength of Individual Architectural Patterns in 1275 Patients From the Canary Retrospective Cohort.Am J Surg Pathol. 2016 Nov;40(11):1439-1456. doi: 10.1097/PAS.0000000000000736. Am J Surg Pathol. 2016. PMID: 27635949
-
The 2014 International Society of Urological Pathology (ISUP) Consensus Conference on Gleason Grading of Prostatic Carcinoma: Definition of Grading Patterns and Proposal for a New Grading System.Am J Surg Pathol. 2016 Feb;40(2):244-52. doi: 10.1097/PAS.0000000000000530. Am J Surg Pathol. 2016. PMID: 26492179 Review.
-
Contemporary Gleason Grading of Prostatic Carcinoma: An Update With Discussion on Practical Issues to Implement the 2014 International Society of Urological Pathology (ISUP) Consensus Conference on Gleason Grading of Prostatic Carcinoma.Am J Surg Pathol. 2017 Apr;41(4):e1-e7. doi: 10.1097/PAS.0000000000000820. Am J Surg Pathol. 2017. PMID: 28177964
Cited by
-
Significance of the cribriform morphology area ratio for biochemical recurrence in Gleason score 4 + 4 prostate cancer patients following robot-assisted radical prostatectomy.Cancer Med. 2024 Mar;13(5):e7086. doi: 10.1002/cam4.7086. Cancer Med. 2024. PMID: 38477506 Free PMC article.
-
WHO Classification of Tumours fifth edition: evolving issues in the classification, diagnosis, and prognostication of prostate cancer.Histopathology. 2022 Oct;81(4):447-458. doi: 10.1111/his.14711. Epub 2022 Aug 2. Histopathology. 2022. PMID: 35758185 Free PMC article. Review.
-
Prostate Pathology: What is New in the 2022 WHO Classification of Urinary and Male Genital Tumors?Pathologica. 2022 Feb;115(1):41-56. doi: 10.32074/1591-951X-822. Epub 2023 Jan 16. Pathologica. 2022. PMID: 36645399 Free PMC article. Review.
-
Current practices in prostate pathology reporting: results from a survey of genitourinary and general pathologists.Histopathology. 2025 Aug;87(2):206-222. doi: 10.1111/his.15469. Epub 2025 May 13. Histopathology. 2025. PMID: 40364451 Free PMC article.
-
[Current grading of prostate cancer. German version].Pathologie (Heidelb). 2025 Sep;46(5):267-273. doi: 10.1007/s00292-025-01446-6. Epub 2025 Jul 2. Pathologie (Heidelb). 2025. PMID: 40601000 Free PMC article. Review. German.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

