Study of Profile of Mucormycosis During the Second Wave of COVID-19 in a Tertiary Care Hospital
- PMID: 35155019
- PMCID: PMC8824768
- DOI: 10.7759/cureus.21054
Study of Profile of Mucormycosis During the Second Wave of COVID-19 in a Tertiary Care Hospital
Abstract
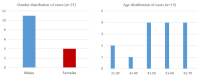
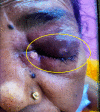
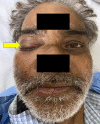
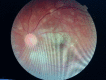
Introduction and aim Mucormycosis is a lethal opportunistic infection caused by filamentous fungi of the family Mucoraceae (black fungus). There has been a sudden increase in the incidence of these cases during the second wave of the COVID-19 pandemic due to the immunocompromised state caused by the disease and its treatment. Early diagnosis and appropriate medical management are essential to reduce disease morbidity and mortality. Through this study, we aim to study the clinical features, risk factors, laboratory investigations, and radiological findings of patients with mucormycosis as well as evaluate the clinical outcomes in each case. Methods and materials This was a prospective study that included only confirmed mucormycosis cases admitted in Tata Main Hospital (TMH) from April 2021 to July 2021. A case of mucormycosis was defined as the one in which clinical and radiological features were consistent with mucormycosis and fungus was demonstrated in the tissue by potassium hydroxide (KOH) mount/culture/histopathological examination (HPE). Data relating to epidemiology, risk factors, clinico-radiological features, and outcomes were analyzed and expressed as a percentage of total cases. Results Of the total 15 cases, three patients (33.3%) had active COVID-19 infection, eight (53.3%) were in the post-COVID-19 state, two (13.4%) had COVID-19 like illness and two (13.4%) patients did not have COVID-19 in the recent past. There was male predominance with the male to female ratio being 2.75:1. The commonest associated co-morbid condition was diabetes mellitus (13 patients, 86.7%). Amongst the myriad manifestations, periorbital swelling was the commonest symptom (11 patients, 73.3%). Among neurological manifestations, involvement of cranial nerves was found in nine (60%) patients with the third cranial nerve being the most commonly affected nerve (eight patients, 53.3%). Cavernous sinus thrombosis (CST) was found in one (6.7%) patient. Diagnostic nasal endoscopy (DNE) revealed eschar at various sites in 13 patients (86.7%). Central retinal artery occlusion (CRAO) was found bilaterally in one patient (6.7%) while two patients (13.3%) had CRAO on the left. Radiologically, the most commonly involved sinuses were maxillary and ethmoidal (eight patients, 53.3%). Bilateral sinus involvement was more common (46.7%) than unilateral sinus involvement. The average length of stay (LOS) was 17.5±7.8 days. The overall mortality was 40%. Five (33.3%) patients developed secondary bacterial infections. All patients received medical therapy with intravenous amphotericin B. In addition, seven (46.7%) patients underwent functional endoscopic sinus surgery (FESS) with debridement of which, five (71.4%) patients survived and made a good recovery. One patient (6.7%) with pulmonary mucormycosis underwent lobectomy. Conclusion New-onset headache, black nasal discharge, periorbital swelling, retro-orbital pain, visual diminution, restriction of eye movements should prompt an immediate search for mucormycosis especially in the background of history of diabetes mellitus in patient with recent or current COVID-19 disease. Radio-imaging with computerized tomography and magnetic resonance imaging are complementary to clinical evaluation in assessing the disease extent and diagnosis of complications. Prompt diagnosis is essential due to the angio-invasive nature of the mucor and requires aggressive anti-fungal therapy and debridement of the devitalized tissue.
Keywords: covid-19; fungal; immunocompromised; infections; mucor.
Copyright © 2022, Kamath et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
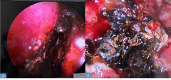
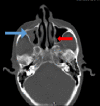
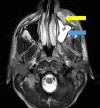
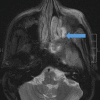
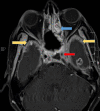
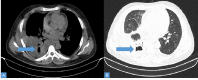
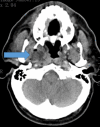

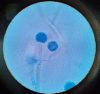
References
-
- Emerging cases of mucormycosis under COVID-19 pandemic in India: misuse of antibiotics. Gupta G, S R, Singh Y, et al. https://doi.org/10.1002/ddr.21862. Drug Dev Res. 2021;82:880–882. - PMC - PubMed
-
- Mucormycoses. Eucker J, Sezer O, Graf B, et al. Mycoses. 2001;44:253–260. - PubMed
-
- Sugar AM. Mandell, Douglas, and Bennett's principles and practice of infectious diseases. USA: Churchill Livingstone; 2000.
-
- Risk factors for fungal co-infections in critically ill COVID-19 patients, with a focus on immunosuppressants. Ezeokoli OT, Gcilitshana O, Pohl CH. https://doi.org/10.3390/jof7070545. J Fungi (Basel) 2021;7:545. - PMC - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
