Postmortem 9.4-T MRI for Fetuses With Congenital Heart Defects Diagnosed in the First Trimester
- PMID: 35155595
- PMCID: PMC8830519
- DOI: 10.3389/fcvm.2021.764587
Postmortem 9.4-T MRI for Fetuses With Congenital Heart Defects Diagnosed in the First Trimester
Abstract
Objective: To evaluate the feasibility of 9. 4-T postmortem MRI (pm-MRI) for assessment of major congenital heart defects (CHD) cases terminated in the early stage of gestation.
Methods: Fetuses with CHD detected by the detailed first-trimester ultrasound scan and terminated before 18 gestational weeks were recruited between January 2018 and June 2020. All fetuses were offered 9.4-T pm-MRI examinations and those terminated over 13+6 weeks were offered conventional autopsies simultaneously. Findings of pm-MRI were compared with those of conventional autopsy and prenatal ultrasound.
Results: A total of 19 fetuses with major CHD were analyzed, including 6 cases of the atrioventricular septal defect, 5 cases of Tetralogy of Fallot, 3 cases of hypoplastic left heart syndrome, 1 case of tricuspid atresia, 1 case of transposition of the great arteries, 1 case of severe tricuspid regurgitation, and 2 cases of complex CHD. Pm-MRI had concordant findings in 73.7% (14/19) cases, discordant findings in 15.8% (3/19) cases, and additional findings in 10.5% (2/19) cases when compared with prenatal ultrasound. Pm-MRI findings were concordant with autopsy in all 8 CHD cases terminated over 13+6 weeks.
Conclusion: It is feasible to exhibit the structure of fetal heart terminated in the first trimester clearly on 9.4-T pm-MRI with an optimized scanning protocol. High-field pm-MRI could provide medical imaging information of CHD for those terminated in the early stage of gestation, especially for those limited by conventional autopsy.
Keywords: 94-T magnetic resonance images; congenital heart defects; first- trimester ultrasound scan; postmortem magnetic resonance imaging; prenatal ultrasound.
Copyright © 2022 Tang, Zhang, Dai, Ru, Li, Chen, Zhang, Zhou, Lv, Liu, Zhou and Zheng.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures





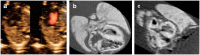


References
LinkOut - more resources
Full Text Sources

