Neck Circumference and Risk of Incident Atrial Fibrillation in the Framingham Heart Study
- PMID: 35156385
- PMCID: PMC9245798
- DOI: 10.1161/JAHA.121.022340
Neck Circumference and Risk of Incident Atrial Fibrillation in the Framingham Heart Study
Abstract
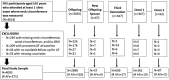
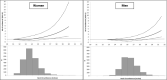
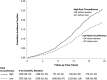
Background Increased neck circumference, a proxy for upper-body subcutaneous fat, is associated with cardiovascular risk and metabolic risk factors, accounting for body mass index (BMI) and waist circumference. The association between neck circumference and incident atrial fibrillation (AF) is unclear. The aim of current study was to evaluate the association between neck circumference and incident AF. Methods and Results We selected participants from the Framingham Heart Study aged ≥55 years without diagnosed AF and with available neck circumference, BMI, and waist circumference measurements. We defined high neck circumference as ≥14 inches in women and ≥17 inches in men on the basis of the Contal and O'Quigley changepoint method. We used Fine-Gray models to estimate subdistribution hazards ratios (sHRs) for the association between neck circumference and incident AF accounting for the competing risk of death. We adjusted models for clinical risk factors. We then additionally adjusted separately for BMI, waist circumference, and height/weight. The study sample included 4093 participants (mean age 64±7 years, 55% female). During 11.2±5.7 mean years of follow-up, incident AF occurred in 571 participants. High neck circumference was associated with incident AF (sHR for high versus low: 1.58; 95% CI, 1.32-1.90, P<0.0001). The association remained significant after adjustment for BMI (sHR, 1.51; 95% CI, 1.21-1.89; P=0.0003), waist circumference (sHR, 1.47; 95% CI, 1.18-1.83; P<0.0001), and height/weight (sHR, 1.37; 95% CI, 1.09-1.72; P=0.007). Conclusions High neck circumference was associated with incident AF adjusting for traditional adiposity measures such as BMI and waist circumference.
Keywords: atrial fibrillation; epidemiology; fat depot; incidence; neck circumference.
Figures
References
-
- Lavie CJ, Pandey A, Lau DH, Alpert MA, Sanders P. Obesity and atrial fibrillation prevalence, pathogenesis, and prognosis: effects of weight loss and exercise. J Am Coll Cardiol. 2017;70:2022–2035. - PubMed
-
- Huxley RR, Lopez FL, Folsom AR, Agarwal SK, Loehr LR, Soliman EZ, Maclehose R, Konety S, Alonso A. Absolute and attributable risks of atrial fibrillation in relation to optimal and borderline risk factors: the Atherosclerosis Risk in Communities (ARIC) study. Circulation. 2011;123:1501–1508. doi: 10.1161/CIRCULATIONAHA.110.009035 - DOI - PMC - PubMed
-
- Chatterjee NA, Giulianini F, Geelhoed B, Lunetta KL, Misialek JR, Niemeijer MN, Rienstra M, Rose LM, Smith AV, Arking DE, et al. Genetic obesity and the risk of atrial fibrillation: causal estimates from Mendelian randomization. Circulation. 2017;135:741–754. doi: 10.1161/CIRCULATIONAHA.116.024921 - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

