Functional and Radiological Outcomes after Treatment with Custom-Made Glenoid Components in Revision Reverse Shoulder Arthroplasty
- PMID: 35160000
- PMCID: PMC8837185
- DOI: 10.3390/jcm11030551
Functional and Radiological Outcomes after Treatment with Custom-Made Glenoid Components in Revision Reverse Shoulder Arthroplasty
Abstract
Glenoid implant position and fixation are challenging in severe glenoid defects in reverse total shoulder arthroplasty (rTSA). Custom-made glenoid implants are metal augmented implants that are specially produced for a certain defect. They provide the restoration of the joint line and proper fixation. This retrospective data analysis investigated the clinical and radiological outcomes after revision using custom-made glenoid implants. Between 2018 and 2020, nine patients (10 shoulders) with severe glenoid defects underwent revision rTSA using a custom-made glenoid implant (Materialise Glenius or Lima ProMade). The pre- and postoperative Constant Murley Score (CMS), UCLA Score and Subjective Shoulder Value (SSV) were assessed. Postoperative CT scans and X-rays in two planes were available. The minimum follow-up was 12 months, with a mean follow-up of 23.1 months. The mean preoperative CMS, UCLA Score and SSV were 10.9, 4.1 and 11.0, respectively. The mean postoperative CMS, UCLA Score and SSV showed significant increases of 51.7 (<0.001), 22.9 (<0.001) and 52.0 (<0.001), respectively. There were no signs of loosening implants or scapular notching, and no revision was necessary. This trial showed promising clinical and radiological short-term outcomes for custom-made glenoid components in revision rTSA.
Keywords: custom-made prosthesis; glenoid bone loss; reverse total shoulder arthroplasty; revision total shoulder arthroplasty.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
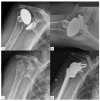
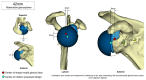


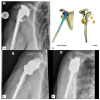
Similar articles
-
Clinical and radiologic outcomes of Lima ProMade custom 3D-printed glenoid components in primary and revision reverse total shoulder arthroplasty with severe glenoid bone loss: a minimum 2-year follow-up.J Shoulder Elbow Surg. 2023 Oct;32(10):2017-2026. doi: 10.1016/j.jse.2023.04.020. Epub 2023 May 30. J Shoulder Elbow Surg. 2023. PMID: 37263477
-
Minimum five-year outcomes of reverse total shoulder arthroplasty using a trabecular metal glenoid base plate.Bone Joint J. 2021 Aug;103-B(8):1333-1338. doi: 10.1302/0301-620X.103B8.BJJ-2020-2362.R1. Bone Joint J. 2021. PMID: 34334038
-
Early results of reverse total shoulder arthroplasty using a patient-matched glenoid implant for severe glenoid bone deficiency.J Shoulder Elbow Surg. 2020 Jul;29(7S):S139-S148. doi: 10.1016/j.jse.2020.04.024. J Shoulder Elbow Surg. 2020. PMID: 32643608
-
Clinical and Radiological Outcomes after Total Shoulder Arthroplasty Using Custom-Made Glenoid Components: A Systematic Review.J Clin Med. 2022 Dec 7;11(24):7268. doi: 10.3390/jcm11247268. J Clin Med. 2022. PMID: 36555886 Free PMC article. Review.
-
Custom-made reverse shoulder arthroplasty for severe glenoid bone loss: review of the literature and our preliminary results.J Orthop Traumatol. 2021 Jan 19;22(1):2. doi: 10.1186/s10195-020-00564-6. J Orthop Traumatol. 2021. PMID: 33464425 Free PMC article. Review.
Cited by
-
The Evolution of Reverse Total Shoulder Arthroplasty-Where Do We Stand and What Comes Next?J Clin Med. 2023 Mar 1;12(5):1945. doi: 10.3390/jcm12051945. J Clin Med. 2023. PMID: 36902731 Free PMC article.
-
Impact of transdermal buprenorphine patch combined with celecoxib on improving shoulder pain and function of patients with primary adhesive shoulder capsulitis.BMC Musculoskelet Disord. 2024 Nov 25;25(1):953. doi: 10.1186/s12891-024-07992-z. BMC Musculoskelet Disord. 2024. PMID: 39587547 Free PMC article.
-
A review of custom implants for glenoid bone deficiency in reverse shoulder arthroplasty.J Orthop. 2022 Dec 22;36:65-71. doi: 10.1016/j.jor.2022.11.016. eCollection 2023 Feb. J Orthop. 2022. PMID: 36605459 Free PMC article. Review.
-
Novel Custom 3D-Printed Glenoid in Reverse Total Shoulder Arthroplasty: A Case Report of Bilateral Total Shoulder Arthroplasties.Cureus. 2025 Feb 10;17(2):e78821. doi: 10.7759/cureus.78821. eCollection 2025 Feb. Cureus. 2025. PMID: 40078235 Free PMC article.
-
Patient-specific implants in reverse shoulder arthroplasty.Clin Shoulder Elb. 2024 Mar;27(1):108-116. doi: 10.5397/cise.2023.00038. Epub 2023 Aug 22. Clin Shoulder Elb. 2024. PMID: 37607862 Free PMC article.
References
LinkOut - more resources
Full Text Sources

