An autopsy case of granulomatous amebic encephalitis caused by Balamuthia mandrillaris involving prior amebic dermatitis
- PMID: 35165936
- PMCID: PMC9546287
- DOI: 10.1111/neup.12798
An autopsy case of granulomatous amebic encephalitis caused by Balamuthia mandrillaris involving prior amebic dermatitis
Abstract
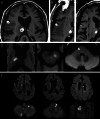
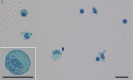
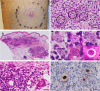
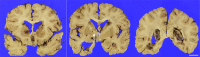
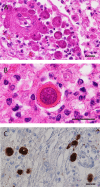
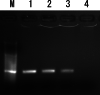
An 82-year-old man, who was healthy and had worked as a farmer, experienced worsening neurological symptoms over a seven-month period, which eventually caused his death. Multiple fluctuating brain lesions were detected radiographically. Clinically, sarcoidosis was ranked high among the differential diagnoses because of the presence of skin lesions showing granulomatous inflammation, confirmed by biopsy. The patient's cerebrospinal fluid was also examined, but no definitive diagnosis was made while he was alive. An autopsy revealed multiple granulomatous amebic encephalitis lesions in the brain. Genetic and immunohistochemical analyses identified Balamuthia (B.) mandrillaris, a free-living ameba, which resides in soil and fresh water, as the causative organism. A retrospective examination revealed B. mandrillaris in the biopsied skin as well as cerebrospinal fluid, strongly suggesting that the ameba had spread into the brain percutaneously. Few studies have detailed the cutaneous pathology of B. mandrillaris infections. In general, granulomatous amebic encephalitis is extremely difficult to diagnose without autopsy, but the present case provides a clue that could allow similar cases to be diagnosed earlier; that is, the presence of skin lesions.
Keywords: Balamuthia mandrillaris; amebic dermatitis; autopsy; free-living ameba; granulomatous amebic encephalitis.
© 2022 The Authors. Neuropathology published by John Wiley & Sons Australia, Ltd on behalf of Japanese Society of Neuropathology.
Figures
References
-
- Visvesvara GS, Schuster FL, Martinez AJ. Balamuthia mandrillaris, N. G., N. Sp., agent of amebic meningoencephalitis in humans and other animals. J Eukaryot Microbiol 1993; 40: 504–514. - PubMed
-
- Schuster FL, Visvesvara GS. Free‐living amoebae as opportunistic and non‐opportunistic pathogens of humans and animals. Int J Parasitol 2004; 34: 1001–1027. - PubMed
-
- Foreman O, Sykes J, Ball L, Yang N, de Cock H. Disseminated infection with Balamuthia mandrillaris in a dog. Vet Pathol 2004; 41: 506–510. - PubMed
-
- Visvesvara GS, Moura H, Schuster FL. Pathogenic and opportunistic free‐living amoebae: Acanthamoeba spp., Balamuthia mandrillaris, Naegleria fowleri, and Sappinia diploidea . FEMS Immunol Med Microbiol 2007; 50: 1–26. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

