The effects of bone-substitute augmentation on treatment of osteoporotic intertrochanteric fractures
- PMID: 35166210
- PMCID: PMC8847843
- DOI: 10.1016/j.bj.2020.05.013
The effects of bone-substitute augmentation on treatment of osteoporotic intertrochanteric fractures
Abstract
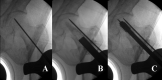
Background: Osteoporotic intertrochanteric fractures often have postoperative complications despite a perfect reduction and an optimal fixation. We describe a simple technique using bone substitute augmentation and hypothesize that this method would prevent excessive sliding of the lag screw and potential subsequent complications.
Methods: Between January 2009 and July 2017, patients with osteoporotic intertrochanteric fractures who were treated with a dynamic hip screw (DHS) were enrolled in this retrospective cohort study. DHS group patients received conventional DHS treatment and BSA-DHS group patients received bone-substitute augmented DHS treatment. Factors such as demographics, Parker and Palmer mobility scores, health-related quality of life (HRQoL) scores (short-form Health Survey-12 Physical Component Summary [SF-12-PCS], and SF-12 Mental Component Summary [SF-12-MCS]), morbidities, mortality, and radiographic outcomes were compared.
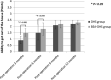
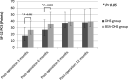
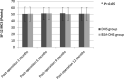
Results: We enrolled 85 patients: DHS group = 37 and BSA-DHS group = 48. There was significant lag-screw sliding (mean: 9 mm and 3 mm, p < 0.001), varus collapse (mean: 7° and 3°, p < 0.001), and femoral shortening (mean: 10 mm and 3 mm, p < 0.001) in the DHS group compared to the BSA-DHS group. The ability to get around the house was significantly different between the DHS and BSA-DHS groups (p = 0.031) at 3 months. Postoperative scores were not significantly different after 6, 9 or 12 months, however. Scores for the ability to get out of the house and to go shopping and the SF-12-PCS were significantly worse in the DHS group at 3 and 6 months. Malunion and lag-screw cutout were also significantly worse in the DHS group (p = 0.037 and p = 0.033, respectively).
Conclusions: Bone-substitute augmentation appears effective to prevent typical postoperative complications experienced by the DHS group patients, and to improve functional outcomes. Additional prospective randomized large-scale cohort studies are necessary to confirm this conclusion.
Level of evidence: Therapeutic Level III.
Keywords: Bone substitute; Health-related quality of life (HRQoL); Intertrochanteric fracture; Osteoporosis.
Copyright © 2020 Chang Gung University. Published by Elsevier B.V. All rights reserved.
Conflict of interest statement
Conflicts of interest All authors declare that they have no competing interests.
Figures




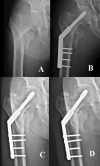
Comment in
-
Letter regarding "the effects of bone-substitute augmentation on treatment of osteoporotic intertrochanteric fractures".Biomed J. 2022 Jun;45(3):565-566. doi: 10.1016/j.bj.2022.03.005. Epub 2022 Mar 17. Biomed J. 2022. PMID: 35306224 Free PMC article. No abstract available.
Similar articles
-
Teriparatide Improves Fracture Healing and Early Functional Recovery in Treatment of Osteoporotic Intertrochanteric Fractures.Medicine (Baltimore). 2016 May;95(19):e3626. doi: 10.1097/MD.0000000000003626. Medicine (Baltimore). 2016. PMID: 27175673 Free PMC article.
-
Dynamic hip screws for unstable intertrochanteric fractures in elderly patients--encouraging results with a cement augmentation technique.J Trauma. 2010 Apr;68(4):954-64. doi: 10.1097/TA.0b013e3181c995ec. J Trauma. 2010. PMID: 20386288
-
Outcomes of dynamic hip screw augmented with trochanteric wiring for treatment of unstable type A2 intertrochanteric femur fractures.Injury. 2017 Aug;48 Suppl 2:S72-S77. doi: 10.1016/S0020-1383(17)30498-9. Injury. 2017. PMID: 28802425
-
[Trochanteric femoral fractures].Acta Chir Orthop Traumatol Cech. 2013;80(1):15-26. Acta Chir Orthop Traumatol Cech. 2013. PMID: 23452417 Review. Czech.
-
[Research advance of dynamic hip screw internal fixation in treatment of intertrochanteric fractures].Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2005 Oct;19(10):839-42. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2005. PMID: 16274138 Review. Chinese.
Cited by
-
Comparative effectiveness research on proximal femoral nail versus dynamic hip screw in patients with trochanteric fractures: a systematic review and meta-analysis of randomized trials.J Orthop Surg Res. 2022 Jun 3;17(1):292. doi: 10.1186/s13018-022-03189-z. J Orthop Surg Res. 2022. PMID: 35658909 Free PMC article.
-
Role of Augmentation in the Fixation of Osteoporotic Fractures.Indian J Orthop. 2025 Jan 16;59(3):294-299. doi: 10.1007/s43465-024-01323-z. eCollection 2025 Mar. Indian J Orthop. 2025. PMID: 40201925 Review.
-
A finger in every pie - The versatility of chemokines.Biomed J. 2022 Jun;45(3):427-431. doi: 10.1016/j.bj.2022.06.001. Epub 2022 Jun 10. Biomed J. 2022. PMID: 35697204 Free PMC article.
-
Letter regarding "the effects of bone-substitute augmentation on treatment of osteoporotic intertrochanteric fractures".Biomed J. 2022 Jun;45(3):565-566. doi: 10.1016/j.bj.2022.03.005. Epub 2022 Mar 17. Biomed J. 2022. PMID: 35306224 Free PMC article. No abstract available.
-
After me, the deluge: The intricacies of pulmonary surfactant.Biomed J. 2021 Dec;44(6):645-650. doi: 10.1016/j.bj.2021.12.003. Epub 2021 Dec 20. Biomed J. 2021. PMID: 34942391 Free PMC article.
References
-
- Lee P.C., Hsieh P.H., Chou Y.C., Wu C.C., Chen W.J. Dynamic hip screws for unstable intertrochanteric fractures in elderly patients–encouraging results with a cement augmentation technique. J Trauma. 2010;68:954–964. - PubMed
-
- Shen S.H., Huang K.C., Tsai Y.H., Yang T.Y., Lee M.S., Ueng S.W., et al. Risk analysis for second hip fracture in patients after hip fracture surgery: a nationwide population-based study. J Am Med Dir Assoc. 2014;15:725–731. - PubMed
-
- Chen I.J., Chiang C.Y., Li Y.H., Chang C.H., Hu C.C., Chen D.W., et al. Nationwide cohort study of hip fractures: time trends in the incidence rates and projections up to 2035. Osteoporos Int. 2015;26:681–688. - PubMed
-
- Strauss E., Frank J., Lee J., Kummer F.J., Tejwani N. Helical blade versus sliding hip screw for treatment of unstable intertrochanteric hip fractures: a biomechanical evaluation. Injury. 2006;37:984–989. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

