PET/MR Imaging in Evaluating Treatment Failure of Head and Neck Malignancies: A Neck Imaging Reporting and Data System-Based Study
- PMID: 35177543
- PMCID: PMC8910793
- DOI: 10.3174/ajnr.A7427
PET/MR Imaging in Evaluating Treatment Failure of Head and Neck Malignancies: A Neck Imaging Reporting and Data System-Based Study
Abstract
Background and purpose: PET/MR imaging is a relatively new hybrid technology that holds great promise for the evaluation of head and neck cancer. The aim of this study was to assess the performance of simultaneous PET/MR imaging versus MR imaging in the evaluation of posttreatment head and neck malignancies, as determined by its ability to predict locoregional recurrence or progression after imaging.
Materials and methods: The electronic medical records of patients who had posttreatment PET/MR imaging studies were reviewed, and after applying the exclusion criteria, we retrospectively included 46 studies. PET/MR imaging studies were independently reviewed by 2 neuroradiologists, who recorded scores based on the Neck Imaging Reporting and Data System (using CT/PET-CT criteria) for the diagnostic MR imaging sequences alone and the combined PET/MR imaging. Treatment failure was determined with either biopsy pathology or initiation of new treatment. Statistical analyses including univariate association, interobserver agreement, and receiver operating characteristic analysis were performed.
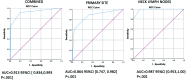
Results: There was substantial interreader agreement among PET/MR imaging scores (κ = 0.634; 95% CI, 0.605-0.663). PET/MR imaging scores showed a strong association with treatment failure by univariate association analysis, with P < .001 for the primary site, neck lymph nodes, and combined sites. Receiver operating characteristic curves of PET/MR imaging scores versus treatment failure indicated statistically significant diagnostic accuracy (area under curve range, 0.864-0.987; P < .001).
Conclusions: Simultaneous PET/MR imaging has excellent discriminatory performance for treatment outcomes of head and neck malignancy when the Neck Imaging Reporting and Data System is applied. PET/MR imaging could play an important role in surveillance imaging for head and neck cancer.
© 2022 by American Journal of Neuroradiology.
Figures
Similar articles
-
Qualitative and quantitative performance of ¹⁸F-FDG-PET/MRI versus ¹⁸F-FDG-PET/CT in patients with head and neck cancer.AJNR Am J Neuroradiol. 2014 Oct;35(10):1970-5. doi: 10.3174/ajnr.A3993. Epub 2014 Jun 12. AJNR Am J Neuroradiol. 2014. PMID: 24924545 Free PMC article.
-
Use of Diffusion-Weighted Imaging and 18F-Fluorodeoxyglucose Positron Emission Tomography Combined With Computed Tomography in the Response Assessment for (Chemo)radiotherapy in Head and Neck Squamous Cell Carcinoma.Clin Oncol (R Coll Radiol). 2018 Dec;30(12):780-792. doi: 10.1016/j.clon.2018.09.007. Epub 2018 Oct 11. Clin Oncol (R Coll Radiol). 2018. PMID: 30318343
-
Are Gadolinium-Enhanced MR Sequences Needed in Simultaneous 18F-FDG-PET/MRI for Tumor Delineation in Head and Neck Cancer?AJNR Am J Neuroradiol. 2020 Oct;41(10):1888-1896. doi: 10.3174/ajnr.A6764. Epub 2020 Sep 24. AJNR Am J Neuroradiol. 2020. PMID: 32972956 Free PMC article.
-
(18)F-Fluorodeoxyglucose PET/MR Imaging in Head and Neck Cancer.PET Clin. 2016 Oct;11(4):375-86. doi: 10.1016/j.cpet.2016.05.002. Epub 2016 Jul 7. PET Clin. 2016. PMID: 27593244 Review.
-
18 F-FDG PET/CT for locoregional surveillance following definitive treatment of head and neck cancer: A meta-analysis of reported studies.Head Neck. 2019 Feb;41(2):551-561. doi: 10.1002/hed.25513. Epub 2018 Nov 20. Head Neck. 2019. PMID: 30456825
Cited by
-
Performance of Neck Imaging Reporting and Data System (NI-RADS) for Diagnosis of Recurrence of Head and Neck Squamous Cell Carcinoma: A Systematic Review and Meta-analysis.AJNR Am J Neuroradiol. 2023 Oct;44(10):1184-1190. doi: 10.3174/ajnr.A7992. Epub 2023 Sep 14. AJNR Am J Neuroradiol. 2023. PMID: 37709352 Free PMC article.
-
The Role of Neck Imaging Reporting and Data System (NI-RADS) in the Management of Head and Neck Cancers.Bioengineering (Basel). 2025 Apr 8;12(4):398. doi: 10.3390/bioengineering12040398. Bioengineering (Basel). 2025. PMID: 40281758 Free PMC article. Review.
-
Recent advances in PET/MR imaging for head and neck tumors: a systematic review of the last three years.Radiol Med. 2025 Aug 28. doi: 10.1007/s11547-025-02075-y. Online ahead of print. Radiol Med. 2025. PMID: 40875092 Review.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
