Aphasia recovery by language training using a brain-computer interface: a proof-of-concept study
- PMID: 35178518
- PMCID: PMC8846581
- DOI: 10.1093/braincomms/fcac008
Aphasia recovery by language training using a brain-computer interface: a proof-of-concept study
Abstract
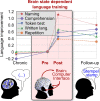
Aphasia, the impairment to understand or produce language, is a frequent disorder after stroke with devastating effects. Conventional speech and language therapy include each formal intervention for improving language and communication abilities. In the chronic stage after stroke, it is effective compared with no treatment, but its effect size is small. We present a new language training approach for the rehabilitation of patients with aphasia based on a brain-computer interface system. The approach exploits its capacity to provide feedback time-locked to a brain state. Thus, it implements the idea that reinforcing an appropriate language processing strategy may induce beneficial brain plasticity. In our approach, patients perform a simple auditory target word detection task whilst their EEG was recorded. The constant decoding of these signals by machine learning models generates an individual and immediate brain-state-dependent feedback. It indicates to patients how well they accomplish the task during a training session, even if they are unable to speak. Results obtained from a proof-of-concept study with 10 stroke patients with mild to severe chronic aphasia (age range: 38-76 years) are remarkable. First, we found that the high-intensity training (30 h, 4 days per week) was feasible, despite a high-word presentation speed and unfavourable stroke-induced EEG signal characteristics. Second, the training induced a sustained recovery of aphasia, which generalized to multiple language aspects beyond the trained task. Specifically, all tested language assessments (Aachen Aphasia Test, Snodgrass & Vanderwart, Communicative Activity Log) showed significant medium to large improvements between pre- and post-training, with a standardized mean difference of 0.63 obtained for the Aachen Aphasia Test, and five patients categorized as non-aphasic at post-training assessment. Third, our data show that these language improvements were accompanied neither by significant changes in attention skills nor non-linguistic skills. Investigating possible modes of action of this brain-computer interface-based language training, neuroimaging data (EEG and resting-state functional MRI) indicates a training-induced faster word processing, a strengthened language network and a rebalancing between the language- and default mode networks.
Keywords: aphasia rehabilitation; brain–computer interface; chronic stroke; language training; neurofeedback training.
© The Author(s) 2022. Published by Oxford University Press on behalf of the Guarantors of Brain.
Figures





References
-
- Dickey L, Kagan A, Lindsay MP, Fang J, Rowland A, Black S. Incidence and profile of inpatient stroke-induced aphasia in Ontario, Canada. Arch Phys Med Rehabil. 2010;91(2):196–202. - PubMed
-
- Dalemans RJ, De Witte LP, Beurskens AJ, Van Den Heuvel WJ, Wade DT. An investigation into the social participation of stroke survivors with aphasia. Disabil Rehabil. 2010;32(20):1678–1685. - PubMed
-
- Doucet T, Muller F, Verdun-Esquer C, Debelleix X, Brochard P. Returning to work after a stroke: A retrospective study at the Physical and Rehabilitation Medicine Center ‘La Tour de Gassies’. Ann Phys Rehabil Med. 2012;55(2):112–127. - PubMed
-
- Berthier ML. Poststroke aphasia: Epidemiology, pathophysiology and treatment. Drugs Aging. 2005;22(2):163–182. - PubMed
LinkOut - more resources
Full Text Sources
