Blood-brain barrier permeable β-blockers linked to lower risk of Alzheimer's disease in hypertension
- PMID: 35196379
- PMCID: PMC9976965
- DOI: 10.1093/brain/awac076
Blood-brain barrier permeable β-blockers linked to lower risk of Alzheimer's disease in hypertension
Abstract
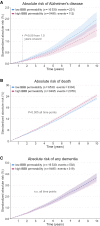
Alzheimer's disease is a neurodegenerative disorder in which the pathological accumulation of amyloid-β and tau begins years before symptom onset. Emerging evidence suggests that β-blockers (β-adrenergic antagonists) increase brain clearance of these metabolites by enhancing CSF flow. Our objective was to determine whether β-blocker treatments that easily cross the blood-brain barrier reduce the risk of Alzheimer's disease compared to less permeable β-blockers. Data from the Danish national registers were used to identify a retrospective cohort of individuals with hypertension, and those treated with β-blockers were included in the analysis. People with indications for β-blocker use other than hypertension (e.g. heart failure) were only retained in a sensitivity analysis. β-blockers were divided into three permeability groups: low, moderate and high. We used multivariable cause-specific Cox regression to model the effect of β-blocker blood-brain barrier permeability on time to dementia outcomes, adjusting for baseline comorbidities, demographics and socioeconomic variables. Death was modelled as a competing risk. The 10-year standardized absolute risk was estimated as the averaged person-specific risks per treatment. In a cohort of 69 081 (median age = 64.4 years, 64.8% female) people treated with β-blockers for hypertension, highly blood-brain barrier-permeable β-blockers were associated with reduced risk of Alzheimer's disease versus low permeability β-blockers (-0.45%, P < 0.036). This effect was specific to Alzheimer's diagnoses and did not extend to dementia in general. Propensity score analysis matching high and low blood-brain barrier-permeable patients also detected a decreased Alzheimer's risk (-0.92%, P < 0.001) in the high permeability group compared to the low, as did a 1-year landmark analysis (-0.57%, P < 0.029) in which events within the first year of follow-up were ignored as likely unrelated to treatment. Our results suggest that amongst people taking β-blockers for hypertension, treatment with highly blood-brain barrier permeable β-blockers reduces the risk of Alzheimer's disease compared to low permeability drugs. Our findings support the hypothesis that highly permeable β-blockers protect against Alzheimer's disease by promoting waste brain metabolite clearance.
Keywords: Alzheimer's disease; adrenergic antagonists; antihypertensive drugs; blood–brain barrier; glymphatic clearance.
© The Author(s) 2022. Published by Oxford University Press on behalf of the Guarantors of Brain.
Figures
References
-
- Villemagne VL, Burnham S, Bourgeat P, et al. . Amyloid β deposition, neurodegeneration, and cognitive decline in sporadic Alzheimer’s disease: a prospective cohort study. Lancet Neurol. 2013;12(4):357–367. - PubMed
-
- Reiss AB, Arain HA, Stecker MM, Siegart NM, Kasselman LJ. Amyloid toxicity in Alzheimer’s disease. Rev Neurosci. 2018;29(6):613–627. - PubMed
-
- Malpas CB, Sharmin S, Kalincik T. The histopathological staging of Tau, but not amyloid, corresponds to antemortem cognitive status, dementia stage, functional abilities and neuropsychiatric symptoms. Int J Neurosci. 2021;131(8):800–809. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

