Models to predict the short-term survival of acute-on-chronic liver failure patients following liver transplantation
- PMID: 35196992
- PMCID: PMC8867783
- DOI: 10.1186/s12876-022-02164-6
Models to predict the short-term survival of acute-on-chronic liver failure patients following liver transplantation
Abstract
Background: Acute-on-chronic liver failure (ACLF) is featured with rapid deterioration of chronic liver disease and poor short-term prognosis. Liver transplantation (LT) is recognized as the curative option for ACLF. However, there is no standard in the prediction of the short-term survival among ACLF patients following LT.
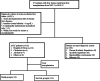
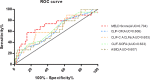
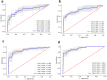
Method: Preoperative data of 132 ACLF patients receiving LT at our center were investigated retrospectively. Cox regression was performed to determine the risk factors for short-term survival among ACLF patients following LT. Five conventional score systems (the MELD score, ABIC, CLIF-C OFs, CLIF-SOFAs and CLIF-C ACLFs) in forecasting short-term survival were estimated through the receiver operating characteristic (ROC). Four machine-learning (ML) models, including support vector machine (SVM), logistic regression (LR), multi-layer perceptron (MLP) and random forest (RF), were also established for short-term survival prediction.
Results: Cox regression analysis demonstrated that creatinine (Cr) and international normalized ratio (INR) were the two independent predictors for short-term survival among ACLF patients following LT. The ROC curves showed that the area under the curve (AUC) ML models was much larger than that of conventional models in predicting short-term survival. Among conventional models the model for end stage liver disease (MELD) score had the highest AUC (0.704), while among ML models the RF model yielded the largest AUC (0.940).
Conclusion: Compared with the traditional methods, the ML models showed good performance in the prediction of short-term prognosis among ACLF patients following LT and the RF model perform the best. It is promising to optimize organ allocation and promote transplant survival based on the prediction of ML models.
Keywords: ACLF; Liver transplantation; MELD; Machine-learning models; Prognosis.
© 2022. The Author(s).
Conflict of interest statement
None of the authors have competing interests to declare.
Figures


References
-
- Belli L, Duvoux C, Artzner T, Bernal W, Conti S, Cortesi P, Sacleux S, Pageaux G, Radenne S, Trebicka J et al: Liver transplantation for patients with acute-on-chronic liver failure (ACLF) in Europe: results of the ELITA/EF-CLIF collaborative study (ECLIS). J Hepatol 2021. - PubMed
-
- Artru F, Louvet A, Ruiz I, Levesque E, Labreuche J, Ursic-Bedoya J, Lassailly G, Dharancy S, Boleslawski E, Lebuffe G, et al. Liver transplantation in the most severely ill cirrhotic patients: a multicenter study in acute-on-chronic liver failure grade 3. J Hepatol. 2017;67(4):708–715. doi: 10.1016/j.jhep.2017.06.009. - DOI - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

